STAND UP TO CANCER
INTRODUCING

STEPHANIE HERRON, STAND UP’S NEW CDO

THE CREATIVITY ISSUE
SIX ARTISTS DRAW INSPIRATION FROM THEIR CANCER JOURNEYS
TOUCH BBCA
THIS NONPROFIT ADVOCATES FOR BETTER REPRESENTATION OF BLACK WOMEN IN THE WHITE-WASHED WORLD OF BREAST CANCER
2023 US $10.00
SPRING
Introducing CancerBuddy™




The first social support network for people facing cancer.



Patients

Bond with a cancer community as you navigate treatment together.
Survivors
Meet cancer survivors, join support groups, and mentor others in treatment.

Learn more at bonemarrow.org/cancerbuddy
Caregivers
Find practical assistance, resources, and emotional support.

Spring is officially here. As the first buds of spring break ground and the air gets warmer, it’s easier to remember that beauty is all around us — and within us. We are happy to introduce you to Issue 18, the Creativity Issue. This issue is rife with creative works from thrivers, survivors and caregivers; each piece exploring themes of grief, strength, hope and perseverance in its own special way. While each person’s cancer journey is unique, art allows us to find connection in shared experience, reminding us that we are not alone. From oil paintings to floral designs to “blackout” poetry and more, this issue features amazing creative work inspired by each artist’s personal cancer journey.

Now, we must turn to something that has arisen suddenly yet unavoidably — we must regretfully inform you that we are concluding the production of Cancer Wellness magazine. Issue 18 is our final, farewell issue.
Throughout our 18 issues, we have had the pleasure of sharing news about the remarkable doctors, hospitals and organizations working tirelessly for the cancer community, along with true-to-life stories from people who have been personally affected by cancer. We could not have done this without the hard work and dedication shown by our contributors and partners.
Cancer Wellness has been a labor of love, and we’re so proud to have been able to provide hope, community and resources to cancer warriors, thrivers, supporters and caregivers over the last five years. It is our hope that, despite the magazine’s closure, the legacy of Cancer Wellness will live on through the ever-inspiring cancer community that has faithfully rallied around us and each other. We’re talking about you, dear reader. Our website, CancerWellness.com, will be maintained indefinitely as a community resource available to anyone who needs it.
Thank you so much for your loyalty and support over the last five years. We are so grateful to have been a beacon of encouragement and hope for many of you, and it is with heavy hearts we must say goodbye for now.
— cW Staff
Cancer Wellness 3
CAYLEI VOGELZANG
Founder
NATALIA ESPINOSA
Editor-in-Chief + Creative Director
CATHERINE EVES
Editorial Director
FEATURES
Editor-at-Large MIRELA KOPIER Editorial Associate FRANCESCA HALIKIAS
SOCIAL MEDIA STRATEGIST
MOLLY MUSSELWHITE
CONTRIBUTING WRITERS
MEGAN KIRBY, AMBER SULLIVAN, MAURA KELLER, SARAH DIMURO, STACIE FLEMING, VIRGINIA CARNESALE, MEGHAN MCCALLUM, LEA GUCCIONE, JOHN OTROMPKE
COVER PHOTOGRAPHER
JUSTIN FOX BURKS
EDITORIAL ADVISORY BOARD
GAIL PRINS, PHD GLEN STEVENS, DO, PHD
OPERATIONS MANAGER
ISABEL GARCIA
SYSTEMS ADMINISTRATOR
JACK SAXE-STARAL
EXECUTIVE ASSISTANT
ANTONIJA ROGIC
DISTRIBUTION
Cancer Wellness is distributed nationally through hospitals, support networks, select nurse navigators, subscriptions, and other outlets. If you would like to know more about distributing Cancer Wellness in your facility or group, please email: info@cancerwellness.com
ADVERTISING
For advertising, advertorial, and special project opportunities, please email: ads@cancerwellness.com
@cancerwellmag
401 N. MICHIGAN AVE. SUITE 325 CHICAGO,
60611 ALL RIGHTS RESERVED. NO PART OF THIS PUBLICATION MAY BE REPRODUCED IN WHOLE OR PART WITHOUT PERMISSION FROM THE PUBLISHER. THE VIEWS EXPRESSED IN CANCER WELLNESS ARE THOSE OF THE RESPECTIVE CONTRIBUTORS AND ARE NOT NECESSARILY SHARED BY CANCER WELLNESS AND ITS STAFF. Cancer Wellness 4
IL
cW
SPRING 2023
12
AFTERMATH
Writer and comics artist Megan Kirby reflects on losing her mother.
13
KEEP IT FRESH
Celebrate spring with these delightfully fresh kitchen staples.
29
COUTURE CANCER
Stacie Fleming struts her stuff on the “chemo catwalk.”
34
LASHING OUT
Celebrity lash expert Dionne Phillips shares a message of hope.
45
39 ROOTS & WINGS
This nonprofit is fighting to improve outcomes for those living with metastatic breast cancer.

56
TUNING INTO HOPE
Hosted by Dr. Diane Reidy-Lagunes, the podcast “Cancer Straight Talk” entertains, enlightens and empowers listeners touched by cancer.
Cancer Wellness 5
STEPHANIE HERRON Stand Up To Cancer’s new CDO
cW Online
Our supporters are our biggest allies. Over on our Instagram @cancerwellmag, we asked questions about how to show support to yourself and your loved ones through a cancer diagnosis. Read on for some thoughts from our followers.


@ASPEYLYNN
I received my diagnosis of chronic lymphocytic lymphoma the day I retired. My CEO called and asked me to come back to work, which I did. Mentally and emotionally, it was the best solution for me. It kept my mind off of me.
—
Lynn Aspey, chronic lymphocytic lymphoma
@CHRISTINE. WILSON.ARTIST
By being creative in some way like art journaling! Write down my feelings and then I’m free to paint over. It could be angry scribbles, a beautiful flower doodle or collage paper. It helps just acknowledging the feelings and get it out on paper in a safe way. No need to share that journal with anyone either. Easy self-care.
— Christine Wilson, breast cancer
@
REMEMBER_
KONJO

I am a breast cancer thriver in Japan. I made 15 minutes [of] drawing my morning routine and kept posting on the Instagram @akipon809. I found drawing is a powerful self-healing tool. Last year I published e-books, and now I am working to make them paperbacks, as well as creating a new one. Great gift from cancer experience.
— Kiyoe Aki
@OHIOCOOPER
@ANGELLOUBJR33
I try to keep my mind occupied by doing crosswords, but it is hard to return to the old you after cancer, as you’re never the same person.
—
Louise Warner, breast cancer

@DLASHES
I stay creative, which keeps me inspired for the future. Hardship is hard; however, I just work on keeping my mind stress-free. Knowing deep inside it’ll all work out! My life is way too important [to worry] about those things.
—
Dionne Phillips, breast cancer


How do you help your son with his cancer when he is helping you with yours? We FaceTime every day (we live in different countries), sadly we compare treatment notes and make each other laugh.

— Kimberly Cooper, lung cancer
@PINKRIBBONMOUNTAINS
It actually helps me mentally by supporting someone. It actually makes me feel less alone by knowing they aren’t alone.
— Noshin Saloojee, breast cancer

Cancer Wellness 6
The cW Agenda
ALL THE NEWS YOU NEED TO KNOW
GENETICALLY BOUND

At the University of Tokyo, scientists are developing an artificial “hairpin-like” DNA molecule that can target and kill cancer cells. It works by binding mRNA molecules that are overproduced in certain cancers. This new method was effective in lab tests against human cervical cancer and breast cancer-derived cells.


TUMOR TAG

Cambridge scientists were able to identify different cancer cell types in a breast tumor by using viruses to tag each type of cancer cell with a unique genetic barcode. Information includes type, quantity and characteristics of the cells in the tumor. Scientists were able to specifically target and kill tumor cells that evaded chemotherapy in lymphoblastic leukemia.
LIGHT IT UP
The FDA has approved Cytalux, a fluorescent imaging agent that lights up cancer cells for easier detection and helps surgeons find and remove lung cancer cells without damaging healthy tissue. This prescription medication was first approved to detect ovarian cancer, and will be used for additional uses. Cytalux is administered to lung cancer patients via intravenous injection prior to surgery.
A GREAT FALL
The American Association for Cancer Research’s annual Cancer Progress Report found that death rates from cancer have been falling over the past two decades, and sharply in recent years. There are now over 18 million cancer thrivers in the U.S., a number credited to the growing use of immunotherapies and early detection.
BUNDLE OF POSITIVITY

Results from a new study called the POSITIVE trial showed that women who paused protective post-cancer therapies to get pregnant had no increased risk of their cancer coming back. The study followed 518 women who were ages 42 or younger and had early-stage breast cancer (up to stage III), who paused their endocrine therapy for around two years while trying to get pregnant.
DREAM DRUG
Adstiladrin, the first gene therapy to treat high-risk, nonmuscle-invasive bladder cancer, has been approved by the U.S. Food and Drug Administration (FDA). Clinical trials showed that 51% of enrolled patients saw the disappearance of all signs of cancer as seen on cystoscopy, biopsied tissue and urine samples.
STEP INTO THE SUN
Are you sick of gloomy weather this past winter? Your body might be, too. The absence of the sun can cause a deficiency in Vitamin D. According to the Academy of Nutrition and Dietetics, vitamin D is crucial for calcium absorption and the maintenance of healthy bones, and can also play a role in cognitive function. As spring arrives, go out and get some sunlight.
CANINE COMPANIONS

Dogs are not only our best friends but might also be able to help us fight cancer. Dogs diagnosed with naturally developing cancers are being enrolled in clinical trials so that doctors can use what they learn to speed potential treatments for both dogs and humans. Because we share many similar genes with dogs, scientists are hoping these studies will lead to a better understanding of cancers in both species.
SLOW IT DOWN
Findings published in the journal Nature show that cancer cells move faster when surrounded by thicker fluids. When cancer spreads to the lymph nodes, lymph drainage is affected, thus causing thicker fluids in some cases. Knowing this information, drugs can potentially be used to short-circuit the signaling pathway and encourage cancer cells to slow down or possibly stop, providing a new way to hopefully stop metastasis.
Cancer Wellness 7
Livia, Laugh, Love.
Marbled walls, glowing white shelves and splashes of pink throughout make Livia Boutique a picture of modern elegance. Featuring products uniquely tailored to the cancer experience, this safe space in the heart of New York City offers breast cancer warriors and thrivers a way to connect, relax and support each other throughout their journeys.
 BY FRANCESCA HALIKIAS
BY FRANCESCA HALIKIAS
Cancer Wellness 8
Before Sarah Rotenstreich founded Livia Boutique, a nonprofit serving women with breast cancer, she was focused on taking care of her family and serving others. As the founder of Batsheva, an organization dedicated to empowering women in their careers, and the founder and executive director of Philip Berley Preschool of the Arts, her life was anything but laid back.
And it wasn’t about to get any easier. While on vacation in Hawaii for her niece’s wedding, Rotenstreich felt a lump in her breast while putting on a bathing suit. She had no history of cancer in her family and no other symptoms, but to be on the safe side, she made an appointment with her doctor when she came home. The results? Stage II breast cancer.
“I remember someone telling me that it’s blessed [to have] lots of problems,” says Rotenstreich. “The reason it’s a blessing is that when you’re worried about a lot of other things, it means there’s nothing super important that’s taking up all your brain space. I remember thinking about that after my diagnosis, because everything else took second place.” Nothing else was more important for Rotenstreich than getting herself and her family through her cancer journey. The drama and deadlines of daily life paled in comparison to what she was about to undergo.
Having five children between the ages of five and 17 at the time — including two sets of twins — meant that Rotenstreich had to figure out the best way to share the news of her cancer diagnosis with her children in a way they would all understand. “I think children are very savvy,” she says. “They pick up on things right away, so your best bet is to share with them age appropriately what is going on and give them space for questions. It was important for me that they [didn’t] see this as a secret or something we were hiding from the world.”
And yet, as many cancer warriors know, sometimes when it comes to supporting your friends and your family through the news of a cancer diagnosis, the support you show yourself falls to the side. Rotenstreich kept working through her cancer treatment — oftentimes going straight to work from chemotherapy or radiation appointments. “I just kept my life flowing in a very similar way, as much as possible,” she says. “I was focused on supporting my family, supporting my siblings, supporting my community, supporting the people who worked with me, and I had less time of actually thinking of what I needed to do to support myself.”
One of the first people Rotenstreich called after receiving her diagnosis was Nancy Brinker, founder of the breast cancer organization Susan G. Komen for the Cure. Rotenstreich’s organization, Batsheva, hosted a gala for 500 women, with Brinker as one of the honorees. “I had just met the woman who founded this huge organization for breast cancer, and she was my first phone call,” says Rotenstreich. “I was like, ‘OK, Nancy, what do I need to know? Which doctor do I go to?’ Just having a network in your life is very important and very supportive.”
But as Rotenstreich knows, sometimes that support can be hard to come by, even in the most unlikely places. When she was first shopping for clothes after her mastectomy, she visited a boutique inside of a large hospital, and the experience was negative. “I went in, and it was very clinical feeling,” she says. “[The employees] were a bit abrupt, and what I needed in such a vulnerable time was just a little bit of love, sensitivity and softness.” Instead, Rotenstreich says her experience was “abrasive, abrupt and very humiliating” — and it takes a lot to humiliate her, she explains.
Despite the negative experience, it was the catalyst to help her conceive of what would eventually become Livia Boutique — a place specifically catered to cancer warriors and thrivers. “I really knew with certainty, it wasn’t even a question in my mind, that this was something I was going to do,” she says.
She spoke with doctors, breast cancer warriors and thrivers to help build her vision of how she could provide this community with what she felt was missing from her own cancer journey. She asked herself, What did breast cancer warriors need that wasn’t easily accessible to them?
“Doctors are amazing at saving your life,” says Rotenstreich. “It’s what we want right then and there, but what they don’t necessarily touch upon is quality of life or making the aftereffects [of cancer] more manageable or gentler.” So, she began reaching out to brands and companies to partner with — for anything from lingerie to products that help women after surgery, chemo or radiation. “There are a lot of little things you could do to make the whole process more comfortable, and that’s the focus of the boutique. How to make post-mastectomy, post-chemo, post-radiation a little easier than it has to be,” Rotenstreich says.
Located in Chelsea, New York, Livia Boutique is delightfully intimate — reaching capacity at 20 to 25 people. Rotenstreich describes it as “one big hug,” but it’s a place for empowerment as well. “Livia” means “lioness” in Hebrew, and Rotenstreich wants to make sure that she can help provide beauty and strength to women on their cancer journeys. “I think it’s so nice for a cancer patient to feel like someone should just catch them, without any explanation or responsibility one way or another,” she says. “I’m here for you, I got you, whatever you need, this is your space, and that’s what I’m looking to provide for the people who come through our door.”
Rotenstreich remembers her own cancer treatment and how at her last radiation appointment, she expected to feel excited she was finally done with treatments. Instead, she felt overwhelmed. For so much of her journey, she was focused on getting better, but there was no focus on the “after.”
“You’re left with a body that’s changed, or skin that barely moves, or arms that don’t raise as high,” she says. “So much of your life changes on a day-to-day basis, and people don’t recognize that when treatment is over, your life has been altered, not just at an emotional level, but very physically you’re a different person too.”
Cancer Wellness 9
“[P]eople don’t recognize that when treatment is over, your life has been altered, not just at an emotional level, but very physically you’re a different person too.”
That’s another aspect that Rotenstreich wants to address at Livia Boutique: the “now what.” What happens when treatment is finished? Rotenstreich explains there are so many post-treatment experiences that women go through that are overlooked, because the cancer is gone, so shouldn’t you feel better? Not quite so, she says. She aims to alter this outlook and include the many ranges of the cancer experience, from pre-treatment to post-treatment and all the challenges that come with each category.
Being an in-person boutique was also one of Rotenstreich’s goals. “There is a lot of info that comes your way that you need to learn how to filter, that you need to learn how to put back on that person in a kind, gentle way. And I wanted a space for the women to just exhale. Literally exhale. Come in and breathe, this is your space.” Rotenstreich believes there is a potential negative of living in the digital age, where everything is online. While there are many benefits to that, she notes, sometimes human connection can get lost amidst technology. Rotenstreich’s hope is that cancer thrivers will feel less alone and more connected to themselves and each other in the in-person space she’s created.

In addition to having beauty and wellness items for pre- and post-treatment needs, Livia will also carry mastectomy products and packing lists for the hospital. The inspiration behind the products in the boutique came from a WhatsApp group of breast cancer survivors of similar age to Rotenstreich. “I felt like I had a testers club,” she says. “I got everybody to share [their] favorite product or favorite support [they received], the best item [they] took to the hospital, and we’ve been creating resources based on a group that’s been using [these items]. There’s no guesswork in what we’ve been designing for the boutique; it’s all been my own personal experience or experience by other patients.”

Products curated specifically for post-mastectomy include robes that have pockets for drains, sweatshirts with inside pockets so you can get dressed after surgery, and creams that help with scars and radiation burns. “My goal is to showcase [these products], and then lead [people] to wherever they need to get them. If someone wants to get it out of town, they can; if someone wants to try it, share it… It’s really just a resource. It’s not a business,” Rotenstreich says.
Overall, however, Rotenstreich wants breast cancer warriors to feel comfortable in their own skin, and to learn how to listen to their body and honor those needs. She hopes Livia Boutique can be a quiet space where women can listen to their inner voice. “I do believe that when we pause long enough to listen to our own inner voice,” she says, “we know what’s best.”
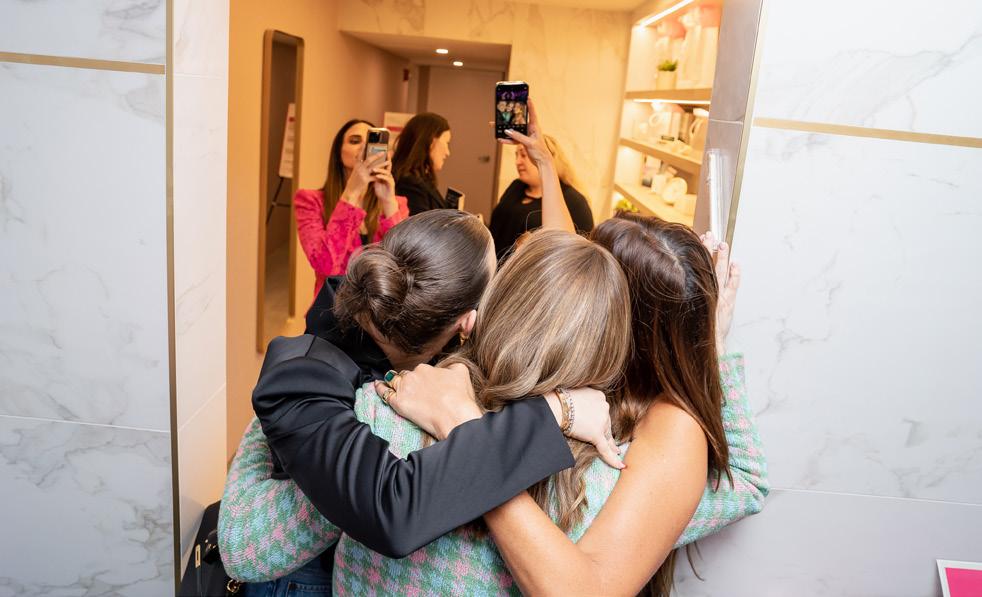
Cancer Wellness 10
Hello, MBC thriver. We see you. We honor you. We support you. Everyday. “What cannot be cured, must be endured.” This quote by Salman Rushdie perfectly reflects our mission at ROOTS & WINGS—to support integrative & wellness programs that increase emotional, physical & spiritual well-being during the continuous oncology treatment for Metastatic Breast Cancer. Visit our site to donate and learn more. And mark your calendar for our annual event, Move IV MBC, coming August 6, 2023. rootswingsfoundation.org
BY MEGAN KIRBY
When I drew this comic, I was living out my worst case scenario. I was 22. My mom had just died from lung cancer — stage IV by the time they caught it. I moved into a basement room in my college town and didn’t know what to do with myself. Drawing comics didn’t make me feel better — but it didn’t make me feel worse, and that was good enough.
I released my first zine, called “Coffee Spoons,” when I was 19. My mom came and cheered me on at the release party at a coffee shop, with blow-up posters of my art hanging on all the walls. I loved the control zinemaking gave me. Being in charge of the content, the printing and the distribution made me feel powerful. I promptly began the second issue — and halfway through finishing it, my mom got her diagnosis.
She didn’t live to see its release.
I drew this comic very late one night, hunched over a desk that used to be hers in that basement room I was renting. It became the final pages in “Coffee Spoons 2.” When I look at it now, I appreciate that the trauma is a little out of focus. It doesn’t mention my mom’s cancer, her death, her absence, but she’s very much at the center of it. I feel that way about most of my art. She always shows up, whether it’s explicit or not.

I will always, always, always miss my mom, but as I get older, I find myself grieving for my past selves, too. Now, I spare some kindness for that 22-year-old girl, feeling so lost in the world, up too late trying to capture something with ink and printer paper.
My mom has been gone for a decade now. I have a job, an apartment to myself. The ground is steady under my feet. I talk to her often, and I know she talks back, in her own way. And I know she’d love my zines. In fact, I’m working on “Coffee Spoons 6” right now.
Cancer Wellness 12
KeepItFresh
Springtime isn’t just for salads! With the changing season comes a new batch of in-season produce for all different palates. Swing into the joy of spring with these light and fresh kitchen favorites.
 BY AMBER SULLIVAN
BY AMBER SULLIVAN
Cancer Wellness 13
BROCCOLI AND CHEDDAR FRITTATA

Yield: 6 servings
Ingredients
Frittata
Nonstick cooking spray
1 tbsp avocado oil
5 small sweet peppers, thinly sliced
8 eggs
1/2 cup milk (or half and half)
1/2 cup grated cheddar cheese
4 scallions or spring onions, chopped
2 cups broccoli, grated or chopped
Cracked black pepper
1 tsp smoked paprika
1 ¼ tsp salt
Side salad
2 cups fresh arugula (or greens of choice)
1 tbsp fresh dill, chopped
Toppings: lemon juice, olive oil, and salt and pepper to taste
Shaved radishes or halved baby tomatoes
Directions
1. Preheat oven to 400 degrees F; generously coat a cast iron or ovenproof pan with with nonstick spray and add the avocado oil
2. Sauté peppers, scallions and chopped broccoli for 5 to 6 minutes until soft; add a pinch of salt and lower the heat
3. Whisk 8 eggs together in a large bowl, and add milk, most of the grated cheese, paprika, salt and pepper; stir to combine
4. Pour mixture over vegetables in pan; add remaining grated cheese on top, then transfer pan to oven for 10 to 14 minutes, until set and golden brown (frittata mixture can also be baked in individual portions in muffin tins — adjust oven temperature to 375 degrees F and bake for 20 minutes)
5. In another bowl, mix together greens, fresh dill, a squeeze of lemon, a drizzle of olive oil, a pinch of salt and some shaved radishes or baby tomatoes
Cancer Wellness 14
PEA PESTO GRAIN BOWL
Yield: 4 servings
Ingredients
3 shallots or 1 large red onion, sliced into 1/2-inch pieces
4 medium-sized carrots, chopped into 1-inch pieces
1 tbsp avocado oil
1 tbsp maple syrup
1 tbsp harissa paste (or to taste; alternatively, replace with a pinch of chili flakes or cayenne pepper)
1 tbsp salt
1 Persian cucumber, s liced into thin rounds
Handful baby kale
Handful baby greens
Quinoa base
1 tbsp avocado oil
1 tsp salt
1 cup quinoa
1⅓ cup water
Dressing
1/3 cup yogurt (vegan or regular)
1 tbsp whole grain mustard
1 tsp salt
1½ tbsp olive oil
Juice of half a lemon or 1 tsp apple cider vinegar
1 tbsp fresh dill, chopped Cracked black pepper
Pea Pesto
2 cups frozen peas, thawed
1/2 cup blanched, skinless almonds (alternatively, Marcona almonds or pine nuts)
Handful of mint leaves
1 tsp salt
Zest of 1 lemon
1/4 cup olive oil
Toppings
Flakey salt
Olive oil
Toasted sesame seeds
Sliced avocado
Optional protein topping: a fried or soft boiled egg, chopped chicken or pan-seared salmon

Directions
1. Preheat oven to 450 degrees F; add
carrots, shallots or red onion, maple syrup, 1 tbsp avocado oil, harissa paste and salt to a bowl and toss until coated
2. Spread mixture on a sheet pan and cook for about 15 to 17 minutes
3. While vegetables bake, rinse quinoa thoroughly and add to a pot with 1 tbsp avocado oil and 1⅓ cup water; bring to boil, then cover and cook on low for 17 minutes
4. Turn off heat; keep pan covered and steam quinoa for an additional 5 minutes; fluff with a fork
5. Make the dressing by mixing all dressing ingredients together in a bowl, adding salt to taste
6. Make the pesto by blending all pesto ingredients in a blender or food processor, adding salt to taste
7. In a medium bowl, mix together greens, cucumber, cooked quinoa, the baked vegetable mixture, sesame seeds, mint, dill and as much dressing as desired
To serve
Spread pea pesto along the side of a bowl or plate, and add a scoop or two of the dressed quinoa and vegetable mixture; add sliced avocado, a drizzle of olive oil, flakey salt and protein of your choice
Chef Amber Sullivan moved to Los Angeles six years ago and discovered her love for farmers’ market-driven California cuisine. She loves to cook for others, focusing on unique, seasonal ingredients for innovative and healthy yet flavorful dishes. Beyond the restaurant industry, Amber has worked as a private chef, developed menus and recipes as a consultant, taught cooking classes, catered events and promoted food pop-ups out of her home in Silverlake. Visit her on Instagram, @eatbyhand.

Cancer Wellness 15
ZAATAR-SPICED POPCORN
Yield: 2 servings
Ingredients
1/3 cup popcorn kernels

3 tbsp olive oil
2 tbsp zaatar spice
1 tsp salt
Zest from 1 small lemon
Directions
1. In a small bowl, mix together olive oil, lemon zest and zaatar
2. Pop popcorn on the stove or in a popcorn maker, then toss in the zaatar mixture until coated
3. Season with salt to taste
GLUTENFREE LEMON ALMOND COOKIES

Yield: one dozen cookies
Ingredients
2 cups almond flour
1/4 tsp baking soda
1/2 tsp baking powder
1/4 tsp salt
1/2 cup sugar, plus 1/4 cup sugar for rolling
4 tbsp butter, softened
1 egg
1 tsp almond extract
Zest of 1 lemon
Juice of 1/2 lemon
‘FISH AND CHIPS’ WITH CREME FRAICHE
Yield: 2–4 servings
Ingredients
1 sweet or white onion, thinly sliced
7 small/medium gold potatoes, rinsed and sliced into 1/4-inch rounds
2 tbsp avocado or olive oil
1 tsp salt
2 cloves garlic, minced or pressed
1 tbsp fresh thyme leaves
1 tsp paprika
1 lb sole, cod or other white fish (about 2 filets)
1 lemon, sliced into rounds
3 tbsp unsalted butter (optional)
1/3 cup creme fraiche or sour cream
Directions
1. In a bowl, mix together sugar and softened butter until light and fluffy; mix in the egg and the almond extract until combined, then mix in the lemon juice and zest
2. In another bowl, mix together the almond flour, salt, baking soda and baking powder
3. Fold the flour mixture into the wet mixture until just combined; let dough chill in the fridge for 1 hour
4. Preheat oven to 350 degrees F
5. Roll the chilled dough into golf ball-sized balls, and roll in sugar until coated
6. Place on baking sheet covered with parchment paper, then bake for about 8 to 10 minutes
7. Let cool before serving
Juice of 1 lemon
Pinch of salt
Fresh parsley
Directions
1. Preheat oven to 425 degrees F
2. Caramelize onion in a cast iron pan with 1 tbsp olive oil and a pinch of salt; cook over medium-low heat for 15 minutes until soft; transfer to a bowl
3. Toss sliced potatoes in a bowl with olive oil, garlic, thyme leaves, paprika and salt
4. Layer the sliced potatoes in the same cast iron pan used to cook onions; and cook in the oven for about 18 minutes; remove from the oven and mix in the caramelized onions
5. Pat fish dry and season with salt and pepper; layer fish filets on top of potato and onion mixture, and top with lemon slices and thyme sprigs, and bake for an additional 10 to 12 minutes, until fish is flakey and cooked through
6. In a small bowl, whisk together creme fraiche or sour cream, lemon juice and salt
7. Top cooked fish with a dollop of the creme fraiche sauce and a sprinkle of paprika
Which white fish? Known for its mild taste, white fish is the basis for this beloved, UK-inspired dish. Cod is rich in protein and contains the antioxidant selenium, while being one of the most sustainable seafood options. Sole has the benefit of being easy to cook with, as its firm texture doesn’t fall apart and holds sauces well, though it is the pricier of the two options.
Cancer Wellness 16

The Gift of Time
Kathy Hren has been a stage IV, ALK-positive lung cancer warrior for almost 12 years. Through life-prolonging medicine and art therapy in the form of quilting, she has been able to live a life she is grateful for.
 BY FRANCESCA HALIKIAS
BY FRANCESCA HALIKIAS
Cancer Wellness 18
Photo provided by Asha Miller
early 12 years ago, Kathy Hren was diagnosed with advanced stage IV lung cancer, and despite what statistics say about stage IV cancers, she’s still here. With the help of anaplastic lymphoma kinase (ALK) inhibitors, self-advocacy and the power of positive thinking, she says these years have been the best of her life.
“Lung cancer crept into my life in 2011,” says Hren. “I had a bit of a dry cough. It was in the spring. Everybody else in the family seemed to have a bit of a cough, but theirs went away. Mine didn’t.” Hren thought it could be allergies, but after noticing shortness of breath, she went to see her general practitioner.
“[The doctor] did some X-rays and there was some opacity in both lungs, which is common with pneumonia. So, we were thinking pneumonia,” says Hren. “She sent me to a pulmonologist. I went through a couple of series of antibiotics and that didn’t clear up the X-rays at all. [They] remained the same.” Hren’s pulmonologist, after conducting a series of breathing tests, a CT scan and a bronchoscopy the following week, gave Hren a diagnosis she never expected.
“The next day I got the diagnosis of adenocarcinoma of the lungs. It was in both lungs, [which meant] advanced stage IV cancer,” Hren says. “That was a real mindblower because I had never smoked. I was 59 years old.”
Life as Hren knew it changed after receiving her diagnosis. She and her husband informed their children about the devastating disease, and had a lawyer come to the house to get Hren’s affairs in order. An oxygen truck delivered tanks to be stored in their garage, and an oxygenator machine was set up not far from Hren and her husband’s bedroom.
She sought care and treatment at the University of Michigan Hospital, where her oncologist told her reaching Christmas that year would be a good goal. Hren was diagnosed Oct. 18 — meaning her outlook was less than two months. However, through biomarker testing — a way to look for genes, proteins and other substances that can provide information about cancer — Hren was discovered to have the ALK gene.
“[The gene] only makes up [around] 5% of lung cancer patients, and generally, people who never smoke are diagnosed with an ALK mutation, so it’s almost like hitting the lottery when you get that news. Of course at the time I didn’t know that,” says Hren. “If you’re going to have lung cancer, you want to fall under that slot. I don’t know how else to put it, truthfully.”
At the time of Hren’s diagnosis, there was only one approved targeted drug therapy for ALK-positive lung cancer patients — a pill called Crizotinib. Hren would take one pill in the morning and one at night. “After one week of taking the Crizotinib,” says Hren, “I was off oxygen and dancing through the house. It was remarkable. Miracle stuff. And I can tell you, there are few life experiences that compare to a cancer remission. I [was] getting a second chance.”
Hren’s next scan after starting Crizotinib showed only microscopic traces of her cancer. The drug was not supposed to be a long-term solution, as Hren’s doctor told her it most likely would only work for a year, but it allowed Hren to be around for the birth of her granddaughter 10 months after starting the pill.
According to the National Library of Medicine, the ALK gene was not discovered until 2007, when scientists found that ALK gene rearrangements were present in a small subset of non-small cell lung cancers. ALK-positive cancers were found to be highly sensitive to ALK kinase inhibitors such as Crizotinib. And while ALK inhibitors can induce remission and extend the lives of patients, once resistance to these drugs develop, a new inhibitor must be tried. Resistance will typically develop after one or two years.
Dr. Shirish Gadgeel, chief of hematology and oncology at Henry Ford Cancer Institute, has been Hren’s oncologist since 2014. “Before 2007, we didn’t know about ALK being a mutation that can drive lung cancers,” explains Gadgeel. “We knew about it only in lymphomas.” Once the report about ALK came out in 2007, the pharmaceutical company Pfizer conducted trials to test lung cancer patients for ALK, and they became the first set of researchers to link an ALK mutation with some forms of lung cancer. After giving ALK inhibitors to patients participating in the trial, they saw “remarkable benefits,” according to Gadgeel. “That led to newer drugs being developed to overcome the deficiencies of the first drug, and now we have patients who are living for eight to 10 years with stage IV lung cancer.”
And for Hren, it’s been even longer. “For 11 years, I’ve been getting scans every three months,” says Hren. She explains how getting a good report from a scan is “such a high.” That high only lasts around six weeks, however, before Hren starts to worry about what her next three-month scan will look like. “I almost compare it to post-traumatic stress disorder, where you just can’t get away from it.”
To take her mind off her “scan-itis” and to give back, Hren — an avid quilter and lover of fabric — stitched hundreds of children’s pillowcases for a cancer organization called Ryan’s Case for Smiles, whose mission is to create and distribute pillowcases that give children an emotional boost and remind them they are not alone.
Hren was able to remain on Crizotinib until March 2014 — almost two and a half years after she was first diagnosed. But her cancer progressed that spring. “There was a drug trial for those that progressed off the drug I was on, and it was offered at Karmanos Cancer Institute here in Detroit. It was a Phase II trial, and Dr. Gadgeel was leading the trial,” Hren says.
After going through the initial evaluation and testing, Hren qualified, and received her first dose of Alectinib — another ALK-inhibitor drug — the next day. The drug was only supposed to work for seven months, but Hren was on it for eight years.
N
Cancer Wellness 19
“There are few life experiences that compare to a cancer remission. I [was] getting a second chance.”
“I stayed with Dr. Gadgeel, my beloved oncologist,” says Hren. “He left Karmanos for a position at [the] University of Michigan, and then he left there for an offer where he is now, for chief of hematology/oncology at Henry Ford. And that’s where I continue to see him now.”
Side effects for Hren were minimal, and she was able to lead, in her words, a pretty normal life. “There’s never really true bliss, or going back to living with gay abandon,” she says. “It’s like living in a temporary state. Do you buy a new pair of shoes, or will the shoes you have last another six months? That’s the state of mind that one lives in, and it’s not bad because I keep telling myself, what’s the alternative? Being dead. Well, you’re not dead yet. You have to have that mindset to live in the day. Just live your life.”
After Hren’s diagnosis and throughout her cancer journey, she became an avid art quilter and has since made two dozen art quilts. “I’ve been in shows, I’ve won awards and I’ve been the featured artist in [two] shows,” says Hren. She has always loved fabric, and used to sell fabric online, but quilting was something that grew out of her cancer journey.
Whenever Gadgeel lectures and displays Hren’s scans, he’ll also show photos of her quilts. “[Quilting] has been my therapy,” she says. “You hear of art therapy, well, there’s some truth to that. I can lose myself in it. I’ve got a fabric stash upstairs, downstairs, my studio is in the back of the house. I can go in there for hours and hours.”

In March 2022, with the help of Gadgeel, Hren started her third targeted-drug therapy, Brigatinib. “It needs to be known how [Gadgeel] helped me and persevered with me,” says Hren. “He’s gifted, he’s kind, he’s dedicated, he’s very thorough.”
And because of this, two months turned into 11 years. “I can honestly say that the past 11 years of my life have been the best years of my life,” Hren says. “Being able to meet my grandchildren and attend my younger son’s wedding. One can do a lot of living in 11 years. Travel, not
so much. Every available moment was spent with my children and their children. That’s how I wanted to spend my time. If they were available, I was available.”
With research on Hren and Gadgeel’s side, the hope is that more ALK-positive patients will have similar outcomes to Hren. “We are trying to understand which ALKpositive lung cancer patients are going to have outcomes like Ms. Hren had, and which patients are not likely to have good outcomes,” says Gadgeel. “If we understand that right in the beginning, we could then tailor the treatment so that we give something extra to the patients who are not going to do well, and maybe help them have the kind of outcome that Ms. Hren had.”
Currently, the focus is on biomarker testing to see whether treatment can become even more personalized for ALK-positive lung cancer patients.“I consider myself a spoiled lung cancer patient,” says Hren. “I told Dr. Gadgeel this and I’m not sure if he appreciates that or likes it, but really, over the years, I’ve only taken a pill. In 11 years, I have never had to have traditional chemo, radiation — I’ve never had surgery, other than bronchoscopies — and I’ve been able to lead a normal life. There is the anxiety that overlays all of this. That never goes away. You can’t really get away from that.”
And while it can be disheartening to be in active treatment for over 11 years, Hren makes sure that she lives each day to the fullest. “I’m not that special of a person,” she says. “I don’t have great accolades, but I can say that I practice survivorship. I don’t really consider myself a cancer survivor. I think a true cancer survivor is someone that actually beat it, and they’re out of treatment. I’ve never really been out of treatment, so I say I practice survivorship.”
Hren urges all cancer warriors and thrivers to think positively and to be their own advocate. She also makes it a point to continue her primary wellness checks, because having cancer doesn’t mean there is no potential to have other health issues.
“Eleven years and I’m still here,” says Hren. “I don’t know how many more. I’m always thinking it’s the last Christmas, the last summer, and that’s what cancer has done for me. It has spoiled holidays and birthdays for me.” And yet, she acknowledges that without her treatment or research into ALKpositive lung cancer, she would not have met her grandchildren. And for that, she has the utmost gratitude.
“I just feel so blessed. I can’t imagine having missed meeting them. And for those that don’t get that chance, I give them an extra hug.”
Cancer Wellness 20
Inhaling Hazards
With flavors such as mango and crème brûlée, vaping among youth and teens was once seen as something enjoyable and trendy. Now, society is recognizing the more sinister side of the brands marketing these potentially harmful products. cW sits down with Dr. Faiz Bhora, chief of thoracic surgery at Hackensack Meridian Health, to discuss this pernicious threat.
 BY FRANCESCA HALIKIAS
BY FRANCESCA HALIKIAS
Cancer Wellness 21
Photo provided by Hackensack Meridian Health
With technology advancing and almost everything that was once tangible turning electronic (see: e-mail, e-book, e-commerce), it’s no surprise cigarettes have also evolved into e-cigarettes — the smoking of which is known as vaping. According to the National Institute on Drug Abuse, vaping devices are now the most common form of nicotine among youth in the United States. Vaping devices are “battery-operated devices that people use to inhale an aerosol, which typically contains nicotine (though not always), flavorings, and other chemicals.” Vapes come in all shapes and sizes, resembling traditional tobacco cigarettes or everyday items like pens or USB sticks, meaning they are easy to hide in plain sight.
Is vaping as harmful as smoking cigarettes? And if so, why is it so heavily marketed to teens and youth? According to the U.S. Food and Drug Administration (FDA) in its 2022 Annual National Youth Tobacco Survey, 14.1% of high school students and 3.3% of middle school students reported current e-cigarette use.
With the onset of the COVID-19 pandemic, respiratory illnesses are currently a hot button issue. A 2020 article from Stanford Medicine linked vaping to a substantially increased risk of COVID-19 among teenagers and young adults. In fact, after surveying over 4,000 participants between the ages of 13 and 24 in all 50 U.S. states, it was found that “those who vaped were five to seven times more likely to be infected than those who did not use e-cigarettes.” And participants who had used e-cigarettes at least once were five times more likely to be diagnosed with COVID-19. This is because of the damage vaping causes to lungs and its related effect of suppressing the immune system, making it more difficult to fight off respiratory infections.
“Some of the major issues with vaping are that there are certain toxins that are present within the chemicals that come within the vaping system,” explains Dr. Faiz Bhora, chief of thoracic surgery and regional chairman of surgery for the central region of Hackensack Meridian Health (HMH). “At least one study has shown that you can
get almost four times as much tar with vaping than you do with just smoking cigarettes.”
And he would know, as he’s seen his fair share of college students and young adults who have come in with collapsed lungs, or pneumothorax, following vaping. “You have to put in a drain in the chest if it’s the first time, [but] if it happens again, you usually need an operation to get [the lung] fixed,” says Bhora.
Surgeries to treat “vape lung” are a relatively new phenomenon, but Bhora has been working in thoracic surgery for more than 20 years. Upon entering medical school, his interest in this specialty was immediately piqued.“I was particularly fascinated by the anatomy and the physiology of the organs in the chest, the heart and lungs,” says Bhora. He was exposed to the medical world from a young age — his father was a cardiologist, and his mother was an OBGYN — so it’s no surprise that he ended up becoming a cardiothoracic surgeon. After attending medical school in Pakistan and doing his surgical residency at George Washington University in DC, he completed a cardiothoracic fellowship from the University of California, Los Angeles followed by an extra year of cancer surgery at the University of Pennsylvania.
Eventually, Bhora found his way to HMH in New Jersey, and is now the regional chairman of surgery for the central region of HMH, the chief of thoracic surgery and professor of surgery at the medical school.

“I’m in charge of most of the surgical services, [and] I’m responsible for building programs for recruitment [to make] sure that we provide the highest quality of care for all the patients in our region.”
Bhora maintains this high quality of care for patients both young and old. Though his typical lung surgery patient is decades past young adulthood, within the last eight years or so, vaping-related illness or injury has brought more and more young people under his care.
“The issue is that folks start vaping at a very young age,” says Bhora. “That inhalation of toxic chemicals and tar has a very detrimental effect on health.” The sense of invincibility common among teenagers — lending a devilmay-care attitude when it comes to their health — is not the only cause for vaping’s young demographic. There is also a heavy push from e-cigarette brands such as Puff Bar and JUUL to market their products to young users. A 2022 Bloomberg Law article accused JUUL of producing “calculated advertising campaigns [that] created a new generation of nicotine addicts.”
Connecticut Attorney General William Tong, in the Bloomberg Law article, describes the impact of JUUL’s youth marketing, noting how they “relentlessly marketed vaping products to underage youth, manipulated their chemical composition to be palatable to inexperienced users, employed an inadequate age verification process, and misled consumers about the nicotine content and addictiveness of its products.”
In an effort to halt teens and adults from purchasing vapes, in 2020 the FDA banned the sale of certain
Cancer Wellness 22
“That’s the problem with smoking and other respiratory toxins; once you actually have symptoms, the damage may already be set and in place.”
flavors that could be perceived as youth-friendly, and only permitted the sale of flavors like tobacco and menthol. However, the ban failed to serve its purpose, with “less than 5% of the 3,500 adult e-cig users quitting [the use of] e-cigs in response to the flavored e-cig ban,” according to a 2020 University of Rochester article. “The rest of the respondents switched to other forms or flavors of e-cigs not covered by the ban or other types of tobacco products.”
In June 2022, the FDA banned JUUL products on US shelves, and the company agreed to pay millions of dollars in settlements to certain states over its unlawful targeting of underage consumers. However, less than two weeks after the ban was announced, it was lifted due to an appeal from JUUL. The FDA then announced a temporary stay on the ban to review additional information.
Negative effects in the short-term may make some young people reconsider e-cigarette use, but health consequences that take time to develop are easier to ignore. “We all begin with the premise that [vaping] is harmful to your health,” says Bhora. “No matter how much you do, small or large, it’s still harmful. Obviously the more you do it, the more risks you have, but even a small amount on a regular basis will most likely lead to harming your lungs
and perhaps increasing your risk of lung cancer.”
Bhora also explains symptoms to watch out for that could point to lung damage, with chronic cough and difficulty breathing being the most common. “Once you start getting symptoms, you may be a bit far along in terms of lung damage,” says Bhora. “That’s the problem with smoking and other respiratory toxins; once you actually have symptoms, the damage may already be set and in place.”
Even vape products without nicotine, such as “wellness vapes” or e-cigarettes that are touted to have vitamins, hormones or essential oils, are not healthy for inhalation, explains Bhora, as introducing any foreign substance into the lungs can be harmful. “I can’t imagine that any of these [wellness vapes] are any better than a healthy lifestyle, eating healthy foods, moderate exercise and staying away from things that are chemicals or potential toxins.”
The FDA also wants consumers to know that no vaping products have been approved to prevent or treat any health conditions or diseases, stating that claims from wellness vapes are “unproven, and the products may be ineffective, a waste of money, unsafe and may prevent or delay you from seeking an appropriate diagnosis and treatment from a health care professional.” Inhaling products can also be dangerous and can trigger severe coughing, airway tightening and make speech and breathing difficult.
Bhora advises that all youth and young adults be cautious about using any type of vape or recreational drug, from marijuana to alcohol to nicotine, because of the potential for these to be “gateway drugs,” or drugs that may lead to the use of other addictive drugs.
As for his work, Bhora is looking forward to continuing to serve patients and spreading awareness about the dangers of vaping and other scenarios that can contribute to lung damage. His goal is to make JFK University Medical Center at HMH a flagship hospital, not just for the region, but for the state and beyond. Patients are already coming from New York City and Connecticut for operations, which Bhora hopes will make HMH a destination hospital with some of the most complex operations being performed there.
The hope is that more patients from other areas will receive the quality of care HMH provides, whatever operation they may need. “I think it’s really exciting to work at HMH,” says Bhora. “They’re the largest health system here in New Jersey, [they have] a new medical school, a great research institute in the Center for Discovery and Innovation, and [they are] committed to providing the highest quality of care for patients.”

Cancer Wellness 23
Tiny Particles, Huge Problems
All plastic products shed “microplastics” — minute particles that are infiltrating the water we drink, the air we breathe and even our own bodies. Research into the effects of microplastics is still young, but signs point to potentially devastating long-term impacts on the environment and human health.
BY MAURA KELLER
Humans tend to use large quantities of plastic every day. From grocery store bags to food containers to synthetic clothing, plastic items are a core part of daily life. Unfortunately, plastic products shed fragments — called microplastics — that make their way into the environment and our bodies and affect long-term human health.
Microplastics are plastic pieces that measure less than five millimeters across. “They are dangerous, if not more so than regular plastic waste, showing many toxic effects on living organisms and the environment,” says Dr. Mark Rosenberg, CEO emeritus at the international nonprofit Task Force for Global Health and former Assistant U.S. Surgeon General. “Microplastics come from many sources, including from larger plastic debris that degrades into smaller and smaller pieces. On the other hand, some have been made small intentionally, like microbeads in facial scrubs.”
Conventional plastic degrades into microplastics when disposed of, when littered, and even during practical use due to erosional breakdown of the plastic surfaces, according to Dr. Suvi Haimi, the CEO and co-founder of Sulapac, a material innovation company with the mission to save the world from plastic waste. Eventually, those small particles become so tiny that they are lightweight enough to be carried by wind. Consequently, microplastics have found their way up to the high altitudes of Mount Everest and the Himalayas, as well as to biodiversity hotspots undersea.
“Airborne microplastics actually originate mostly from plastic waste in the oceans,” Haimi says. “Like air pollution, which also includes plastic particles, microplastics are almost
impossible to clean once they are released into the environment. They break down into even smaller nanoplastics, which last forever, and just keep accumulating, causing a bigger and bigger threat to our ecosystem and health every day.”
How microplastics interact with soil also can affect soil functioning. Rosenberg explains that when microplastic particles enter soil, they change soil structure and texture — studies have shown that this can alter the soil’s ability to absorb water and increase its pH levels. This results in toxic effects on earthworms, snails and nematodes — organisms that play an important role in industrial agriculture. According to a March 2022 study published in the journal Frontiers in Environmental Science, “Microplastics affect the normal metabolic activities of soil organisms through physical and chemical toxic effects and multiple carriers, affect ecosystem health and service functions, and pose potential threats to human food safety, thereby causing harm to human health.”
“These plastics can also be found in water sources,” Rosenberg says, “which many animals drink from, and as a result, it affects their health.” Some health effects on marine animals include delayed growth and organ and tissue damage. While the overall consequences of microplastics on biodiversity are still unknown, Haimi says there are studies describing the adverse effects of microplastics on individual species and specific ecosystems.
For example, microplastics have been linked to causing disease in coral reefs, such as bleaching, skeletal erosion and growth abnormalities. Recently, it has been discovered that bees are carrying microplastics on their feet combined with pollen.
“If we help to tackle this threat, we can do our part to leave this world a little better than how we found it.”
Cancer Wellness 24
“What happens when there are fewer bees, and they can pollinate less due to the microplastics they carry? What will be the outcome if microplastics, like grains of sand clogging the wheels of the world, continue to spread and everything begins to function less and less efficiently?” Haimi asks. “Too little research is complete on the longterm effects, but we already have alarming signals.”
A CAUSE FOR CONCERN
Microplastics are in the air we breathe, and they travel through the food chain onto our plates.
“Microplastics run through our veins and our lungs. They have been discovered in breast milk, so even newborn babies cannot avoid being exposed to microplastics,” Haimi says.
And it is a global phenomenon, affecting consumers regardless of where they live.
Rosenberg points to research from 2021, which indicates the U.S. and U.K. tend to produce more plastic waste than any other country. Past research has also said that Asian countries with coastal communities tend to be responsible for major plastic pollution, with China, Indonesia and Vietnam as some of the worst contributors. “It’s interesting, though, because even though China and India might have the world’s largest populations, and China is a major manufacturer of plastic, both countries are far behind the U.S. in terms of who is generating the most plastic waste,” Rosenberg says. “It’s found that the overall amount of plastic pollution is made in the U.S. and is believed to be two to eight times greater than in comparable countries. The United Nations Environment Programme has said that if we continue with our routine of plastic waste use, our oceans could contain more plastic than fish by 2050.”
And while we don’t yet know all the harmful effects of microplastics, Haimi says microplastics could be compared to asbestos or lead — materials that once were considered useful until their dangerous side effects were discovered. “We can’t afford to wait around to confirm all the unintended consequences of conventional plastic. Scientists have already warned us,” Haimi says. “Just recently, in August 2022, the World Health Organization stated that we need to reduce the use of plastics and move towards a more ‘sustainable plastics economy.’” According to Haimi, this should entail a stringent circular economy in which we ensure the plastics we use are recycled, composted or renewed.
That said, Christopher Reddy, a senior scientist in the Department of Marine Chemistry and Geochemistry at Woods Hole Oceanographic Institution, has been studying ocean pollution for nearly three decades. Reddy says that without any doubt, studying microplastics is the most challenging part of his research. The reason is quite simple: “They are very much like ‘snowflakes’ — every one of them is different. There is a wide range of plastics produced — all of which are different beasts. Some float on water; some don’t,” Reddy says. “On top of the different polymers, there are a wide range of additives, [such as]
color, strength, flame retardants, in plastics that carry their own risk. Then you have different sizes and shapes. Lastly, plastics in the environment can act like sponges and pick up other contaminants like PCBs and DDT.”
Reddy notes that there are papers published every week about human health and plastics but none are definitive.
“Some indicate the likelihood of cancer in laboratory experiments, but we don’t know with great confidence if the plastics being tested in the labs are truly representative of true exposure,” Reddy says. “With time, we will know more.”
Indeed, as Rosenberg further explains, some studies have yet to demonstrate a link between microplastics and breast cancer risk, for example, but many scientists assume that such a link will eventually be demonstrated.
“Microplastics can have carcinogenic properties, basically meaning they can potentially cause cancer. Microplastics can sometimes contain a mixture of endocrine-disrupting chemicals, which can be harmful,” Rosenberg says.
“Exposure to estrogen can mimic important windows of development causing changes in breast development that increase the risk of breast cancer later in life.”
A PROACTIVE APPROACH
Consumers tend to be a big contributor to the plastic problem in general. However, there are things individuals can do to reduce the effects of microplastic; primarily, to reduce, reuse, recycle and replace conventional plastic — what are colloquially known as the “4Rs.”
“These 4Rs are needed in the fight against plastic pollution,” Haimi says. As we chop vegetables on a cutting board made of conventional plastic, we also scrape off pieces of plastic, and when we open and close plastic containers, again and again, they release microplastics. Haimi says that whenever possible, choose products made of materials that do not leave permanent microplastics behind.
“Synthetic clothing, such as polyester, also is a major contributor to microplastics. So, shopping for clothes more consciously can help,” Rosenberg says. “Try avoiding single-use plastics, and instead bring your own bags. Or instead of a plastic water bottle, use a reusable one. Don’t microwave your food in plastic, and try to regularly dust and vacuum, as a good bit of dust particles in your home are made of microplastics.”
Rosenberg stresses that controlling microplastics in the U.S. alone won’t be enough to stop the threat of microplastics globally.
“Countries will have to work together and each will have to take the necessary steps, as well as agree to what those necessary steps are,” Rosenberg says. “This will require the building and use of a coalition of nations that are willing to collaborate. And while microplastics represent a serious threat, we have some valuable lessons for how we can understand and overcome this threat. If we help to tackle this threat, we can do our part to leave this world a little better than how we found it.”
Cancer Wellness 25
American Lung Association
Celebrates Lung Health at Fight for Air Climb, Join Their Mission Efforts!
By Jill Smith & Chrissy Cohen
The Fight for Air Climb is a signature event for the American Lung Association. Climb Miami took place on March 4th at loanDepot park – Home of the Miami Marlins, where participants were challenged to climb 1,700 steps in this iconic South Florida stadium. Messages from fellow participants and sponsors on the jumbotron inspired more than 600 climbers, including first responders in full firefighter gear!
“After losing my mother to lung cancer, I took the time needed to grieve, be sad, get mad, and then do something about it,” said Colleen Fitzgerald, team captain of LGG Squad. “That is why I am dedicated to Climb Miami year in and year out.”
Events hosted by the Lung Association are entertaining and engaging and never lose sight of the mission at hand: to save lives by improving lung health and preventing lung disease. For more information about American Lung Association events, programs, and engagement opportunities in South Florida, call 954-727-0907 or email Chrissy.Cohen@Lung.org. Like us on facebook.com/ LungSoFla or follow us on Instagram at @lungsofla
Upcoming Events
April 21
Las Olas Wine and Food Festival
A culinary celebration that includes food from over 40 local restaurants and sips of 150+ different wines. Use promo code: CWCARES to receive $15 off per general admission ticket. lasolaswff.com
May 8 - 14
LUNG FORCE
Turquoise Takeover
Lung cancer awareness initiative that encourages organizations to creatively utilize the color turquoise throughout the campaign. Sign up to learn how you can get involved and stay informed of lung cancer programs and initiatives. turquoisetakeoverchallenge.org
June 3
LUNG FORCE Sunset Soiree
An annual luxury lifestyle event with a variety of custom experiences designed to entertain and engage guests, such as the Sip ’n’ Shop Style Lounge, Digital Photobooth by UKG, and silent auction by Ginsberg Shulman Attorneys at Law. lungforcesunsetsoiree.org

Ongoing Community Connections
Learn about lung health through a series of educational webinars presented by Memorial Healthcare System where the audience interacts with doctors, medical experts, and the Lung Association team. Attendees will walk away with tips on how to better manage their lung health. For more information follow us on facebook.com/LungSoFla.
The Healing Flow of Energy
Bioenergetic wellness is a healing modality that channels energy into and through the body to relieve mental and bodily stress while promoting overall wellness.
BY SARAH DIMURO
The stress of a cancer diagnosis can wreak havoc on an already vulnerable body. Invasive surgeries and grueling treatments cause many to search for ways to curb side effects and help with overall healing — this is where the field of bioenergetic wellness can help. According to the Holistic Chamber of Commerce, bioenergetic wellness is defined as “a holistic and natural way to access the body’s innate and inner wisdom so it can reveal what it needs for optimal health and wellbeing.” This type of wellness therapy insists that in order to truly heal the ailments of the body, one must also address any areas of the body and mind holding tension.
People in treatment for cancer, or anyone interested in this alternative healing modality, should not abandon or substitute bioenergetic therapy practices for conventional medicine, but employing some of the techniques of this therapy can improve overall quality of life, leading to better survival rates and lower risks of recurrence, according to the International Institute for Bioenergetic Analysis (IIBA).
The body’s innate healing potential is optimized when its major systems are in a state of homeostasis, or balance, according to the Canadian Association of Bioenergetic
Wellness (CANBEWELL). Their website states that employing these practices can help “promote, restore and maintain a clear, balanced flow of energy in the body systems.”
Targeting areas of the body that are holding tension, and releasing this stress, is one way to help energy flow more easily. CANBEWELL lists the following as examples of bioenergetic wellness techniques: “holding, massaging or tracing the acupressure points or meridian lines in the body,” with examples of the “stomach channel” located on the front of the leg, or the “lung channel” located above the wrist; “massaging neurolymphatic trigger points,” which run along the spine, ribs, sternum and collar bone; or “holding neurovascular trigger points on the head,” such as the forehead and the very top of the head. CANBEWELL says these techniques channel the flow of energy “into and through” the organs, nervous system, muscles, tendons, ligaments and fascia, supporting healing and long-term health. With a focus on the intricate connection of bodily systems, it comes as no surprise that many of the ideas associated with bioenergetic wellness originate from the science of kinesiology and how your body moves and operates.

Cancer Wellness 27
WHAT TO EXPECT DURING A BIOENERGETIC WELLNESS APPOINTMENT
Once you have located a bioenergetic wellness practitioner in your area — either through your own research or by contacting an integrative medical doctor for a referral — you can expect your practitioner to take a very personalized approach during your first visit.
Dr. Jonathan Fields, clinic director and founder of Florida’s Integrative Medicine US, explains that each appointment is tailored around the needs and issues of each patient. Fields says the initial appointment focuses on educating the patient about the systems of the body, then doing a deep dive into their medical history, diet and lifestyle, while discussing emotional stress and any past trauma. A focus on nutrition is especially important when it comes to bioenergetic modalities, according to Dr. Michelle Greenwell, who holds a doctorate in Complementary and Integrative Health and is the president of CANBEWELL. “It’s important to identify which foods raise your energy up and which foods drop the energy down, and that will not be the same foods for each person,” Greenwell says.
Collecting all of this information from new patients is critical for practitioners to best individualize treatment protocol. According to Fields, practitioners may prescribe some of the following modalities that utilize bioenergetic techniques: reiki, mantras, EFT tapping (which stands for emotional freedom technique), Qigong, hypnosis, meditation, visualizations, shaking, breathwork and psychotherapy.

Fields explains that bioenergetic wellness practices have a long history. “Since ancient times, it was believed that blockages of energy would lead to pain and disease,” he says. “Science has confirmed this. You need only look at a condition like atherosclerosis — a buildup of fat on arterial walls that impedes circulation — to see how this makes sense.” Decades ago, Fields was introduced to practices such as Qigong and acupuncture, which he says would later be keys in his recovery from a chronic illness.
According to Ron Baker, bestselling author and bioenergetic wellness practitioner, the philosophy behind this modality has been essential in healing many of his wellness coaching clients. “It is focused on moving energy through the body, which creates flow. That, in turn, promotes health and wellbeing,” Baker says. “It also focuses on releasing charged emotional energy that most people collect in their bodies. That is what is often responsible for creating energetic blocks and inflammation in the body. To release those energies has had a profound impact on all types of illnesses,” he says.
Fields echoes Baker, noting that bioenergetic wellness can also be paramount in helping cancer patients survive and thrive during and after treatment. “These practices make for wonderful complementary therapies while undergoing cancer treatments,” says Fields. “By releasing unwanted tension from
the body and ensuring that blood and energy are flowing unobstructed, you can potentially speed up the healing process, as well as improve your mental [and] emotional health throughout.”
“BIOENERGETICS” IS DIFFERENT THAN BIOENERGETIC WELLNESS
Greenwell says it’s important to not confuse bioenergetics with bioenergetic wellness. Bioenergetics uses tools and electronics to help patients get better, “but with bioenergetic wellness, you energize yourself in activities that increase the energy and vitality that you live with; it doesn’t require extra things,” Greenwell says. She herself saw firsthand the role of bioenergetic wellness in cancer care and recovery. When her daughter was diagnosed with Hodgkin’s lymphoma at the age of 15, Greenwell called upon her wellness training to support her daughter during treatment, employing touch and movement therapies. “During her chemo treatments, my focus was to energetically bring her body into flow with the chemicals going into her body,” Greenwell explains. She says that when you focus on balance and flow you are able to help the medication go right where it needs to for the best results. “Chemo, radiation, whatever cancer treatment you have to undergo, we have the ability to take stress out of it so your body can optimize its wellness,” Greenwell says.
She also says the bioenergetic wellness philosophies are valuable for cancer survivors post-treatment. “Anyone who has had cancer knows that any little ache or pain you experience afterwards can cause you to wonder, Oh no, is the cancer back? But bioenergetic wellness is about bringing balance and flow in so those thoughts don’t have to be there,” Greenwell says. “Very simple techniques [help] bring everything back into flow, and those stressful thoughts disappear.”
TRY IT OUT
Greenwell uses a simple exercise to describe how bioenergetic wellness actually works: Turn your head and look over your shoulder, noticing how far you are able to move your head and what it feels like. Then take your hand and gently rub your ear from top to bottom three times. Then turn your head again and you’ll notice your range of motion has changed. Greenwell says this is the crux of bioenergetic wellness. “It’s all about engaging with the body so you can get the signals going in the right way,” Greenwell says.
Bioenergetic wellness, particularly for cancer patients and survivors, is another tool that can be added to the care arsenal. Greenwell says that unlike going to a clinician for a massage or acupuncture treatment, where you lie back and let them do the work, bioenergetic wellness requires patients to participate in their own treatment. You set your own goals for your wellness and as a result feel incredibly empowered. Even years after diagnosis and treatment, patients can be triggered by routine checkups and follow-up scans, but with the practice of bioenergetic wellness, you can arm yourself with tools to help better navigate those necessary visits.
Cancer Wellness 28
“By releasing unwanted tension from the body and ensuring that blood and energy are flowing unobstructed, you can potentially speed up the healing process, as well as improve your mental [and] emotional health throughout.”
couture cancer couture cancer
While Stacie Fleming was living out her fashion-fueled dreams in Paris, France, strange symptoms called her back to the U.S. The diagnosis? Late-stage ovarian cancer. But Stacie refused to allow cancer to consume her identity, and she used treatment sessions as an opportunity to don a show-stopping outfit and strut her stuff on the “chemo catwalk.” The results? Nurturing her creative spirit allowed her to ultimately find healing.
BY STACIE FLEMING

Cancer Wellness 29
was living my dream life in Paris, successfully navigating the cobblestone streets in high heels, blissfully unaware of the clandestine cancer brewing inside me. As a fashion blogger and journalist, I attended runway shows from Paris to Milan, writing rave reviews, getting up close and personal backstage with designers and enjoying champagne-soaked soirées. I often had to pinch myself as I walked around the fashion capital of the world, enthralled by its beauty, charm and sophistication. Little ole me, The Blonde Cherie (the name I had given my brand, fashion blog and Instagram), a California girl living her best life abroad in the City of Light. Enchanted by the concept of la parisienne, I hoped to embody the attitude, spirit and style of this ultra-feminine, chic woman — think Audrey Hepburn and Grace Kelly. Joie de vivre filled my heart each day as I lived out my fashion dreams, oblivious to the foreboding future that lay ahead.
My beautiful Parisian life came to an abrupt halt when strange pains in my lower abdomen brought me back to the States. I had been diagnosed with fibroids while living in Paris — even rushed to the hospital a few times for abdominal pain — but I always brushed it off as nothing. Having lived abroad for almost a decade, culture shock was omnipresent when I first returned to Southern California. I fell into what I call a “suburban slump.” I gained weight; my stomach was bloated and distended. I figured it was the culmination of food changes, lifestyle differences and feeling down in the dumps. Again, I brushed it off as nothing, like my doctors had done.
At this point, my lower abdominal pain was worsening, and I had a new strange pain in my left femur.
At the height of my suburban slump came the onset of the global pandemic. Why not add a little more drama to the mix? By the time COVID19 entered the scene, I had already seen a gastroenterologist, gynecologist, orthopedist and been to the emergency room to no avail. My gynecologist at that time enlightened me that I had fibroids and ovarian cysts, but had a rather laissez-faire attitude about removing them. Not once did she suggest that I might have cancer. To make matters worse, elective surgeries were put on hold indefinitely due to the pandemic.
back to Paris? Joking aside, my life turned upside down in the blink of an eye when I was diagnosed with a rare form of ovarian cancer, called clear cell carcinoma. The chaos that ensued in my head the next several months was nothing short of pandemonium. An amalgamation of anxiety, denial, fear and sadness permeated every thought. I went so far as to research an assisted suicide clinic in Switzerland. I was highly staged, so I thought I was a goner for sure. I felt out of control, overwhelmed and ugly. My second surgery left me with a 10-inch scar on my stomach, and with surgical hernias. Yikes! I needed to get a grip if I was going to beat this disease!
In May 2020, my lower abdominal pain had reached a level 10. Thankfully, I was finally able to get in for a laparoscopic myomectomy to remove what the doctor thought was an ovarian cyst. I woke up happily sedated, only to have my high abruptly interrupted with three ghastly words: You have cancer. I was thinking to myself, Excusez-moi? I think you have the wrong girl. Can I please get another sedative, and hop on a plane

After a cacophony of protest, and some deep reflection, I had a little tête à tête with myself to get my head in the game. My type-A personality kicked in, I put on my investigative journalism hat and I armed myself with knowledge. I felt compelled to get creative in my approach to fighting and beating cancer. I coined the term “couture cancer,” and “chemo catwalk,” vowing to fashionably beat my cancer with style, grace and panache. Fashion immediately became a driving force in my cancer journey, providing me with renewed hope. Karl Lagerfeld, the iconic designer who helmed Chanel for more than 30 years, once said, “Sweatpants are a sign of defeat. You lost control of your life, so you bought some sweatpants.” I was determined to not turn into that person. I would fight an un-chic disease with style. I would turn this negative into a positive. I would radiate light! Straight off the Paris runways, I would strut my stuff on the “chemo catwalk.”
Dressing up for chemotherapy, 32 immunotherapy sessions and oncology appointments made me feel confident, empowered and fierce. I felt like I could take on the world. My ensembles were my armor, shielding me from the negativity of my treatments. I harnessed the hidden power that lies in what we wear. I learned a lesson a long time ago: Wearing something that made me feel good positively impacted my mindset, wellbeing and mental health. If I looked good, I felt good. I chose colors that sparked feelings of joy and happiness, making my treatments more manageable. I expressed my unique style from head to toe, flaunting either my bald

“Fashion immediately became a driving force in my cancer journey, providing me with renewed hope.”
I
Cancer Wellness 30
head or capricious curls, wigs and other sassy looks. I even boldly rocked my birthday suit for an Instagram post, wearing my scars as a badge of honor. Before each treatment, I would stop somewhere that made me happy. Whether the beach, a coffee shop or a beautiful view, I would take a few meditative moments to get mentally prepared, and take a photo of my OOTD (internet speak meaning “outfit of the day”). By dressing up, the fashionista in me was still alive, honoring an important part of the old me.
As fate would have it, my oncologist was a bit of a style icon himself. Divine intervention definitely brought us together. He expressed himself through his stylish socks. My triweekly checkups became our own exclusive fashion show. He would demonstrate his flair for fashion through his dapper dress socks, and I would rock my cancer-chic, warrior wardrobe. I began adding to his sock collection. The first pair I bought him was a set of whimsical teal butterflies to symbolize hope. It brought me immense comfort to see him wearing those socks. To my delight, my fashion choices also brought joy to the infusion center team of doctors and nurses. They couldn’t wait to see what I would wear next. Serving up a side of sass at each infusion allowed me to flex my creative muscle and bring joy to an otherwise depressing situation.
Fashion became my creative outlet during the “two Cs” (COVID-19 and cancer). Similar to drawing and painting, it became a way to express myself artistically. It got my creative juices flowing again and opened my heart, allowing me to honor and recognize
my new identity. I used fashion as a form of self-expression at a time when I felt nothing like myself. When my life became consumed by doctor’s visits, dressing up allowed me to still live creatively. Honing in on my personal style during my cancer journey was a powerful tool to reinvent myself and reinforce my self-image. I learned a powerful lesson during this transformative journey: Fashion is a creative outlet that allowed me to express and recognize my unique identity. I am grateful for fashion’s healing effects, and the joy it brought me during such a trying time.
this life-changing journey to cultivate creativity. Fashion provided me with an outlet to fiercely fight this disease. Find your outlet — let creativity be your guiding light and use its forces to heal you. Be bold! Be courageous! Through embodying the spirit of la parisienne and kindling feelings of joie de vivre, I fashionably beat my cancer, and I hope sharing my story inspires warriors everywhere.
I may no longer live in Paris, but I will forever radiate Parisian-chic wherever I go. My suburban slump has subsided, having triumphed over my “couture cancer” while looking très chic. I shed my sickness and reclaimed my femininity through style and grace. I encourage everyone on




Cancer Wellness 31
“I used fashion as a form of self-expression at a time when I felt nothing like myself. When my life became consumed by doctor’s visits, dressing up allowed me to still live creatively.”
Super Clean Solutions
Stage is on a mission to empower the breast cancer community with knowledge, confidence and style. When their founder, Virginia Carnesale, learned about the harmful toxins in most beauty products after receiving her breast cancer diagnosis, she was shocked at how difficult it was to find products that were free of the most concerning ingredients — like endocrine disruptors and carcinogens. With Stage, Carnesale provides a curated selection of high-performing skincare, haircare and cosmetics to help take the guesswork out of switching to clean beauty.
BY VIRGINIA CARNESALE
Launched in February 2022, Stage is a mission-driven marketplace created to help women with breast cancer feel stylish, supported and confident at every stage of treatment. Stage is a one-stop shop for patients and supporters to find products, gifts, uplifting stories, tips and advice — all from a community of women who have been through a breast cancer journey.
Stage’s marketplace also offers survivor-approved products such as lingerie, loungewear, activewear, swimwear, bags, headwraps, home goods and gifts. They also donate five percent of annual net proceeds to charitable organizations who offer grants and supportive services within three pillars: financial assistance, fertility preservation and integrated wellness-based therapies.
Stage’s selection of beauty products are free of harmful toxins, including sulfates, parabens, phthalates, aluminum, talc, triclosan, formaldehyde and oxybenzone. Learn more about Stage’s banned ingredients list in the Advice section of their website. Shop some of Carnesale’s favorite beauty products for treatment and beyond, which can all be found at ShopStage.co.
COCOBABA
During chemo, I discovered the magical properties of coconut oil. It was the only thing I could put on my dry skin that delivered lasting hydration. Enter Cocobaba — an ethically sourced organic line of coconut oil-based products. Founded by Emma Willis, the daughter of a breast cancer survivor, this line is made with love.


COCONUT BUTTER MOUSSE
I recommend this for all-over use after the shower or whenever your skin feels like it needs a drink.
COCONUT BODY OIL
This oil is a staple for those of us affected by radiation dermatitis. This coconut oil blend won’t solidify in lower temperatures, comes in a mess-free pump and can be used daily for maintenance of skin. Layer this body oil with Cocobaba’s butter mousse or pure shea butter for a lasting effect!
Cancer Wellness 32
SEEN
Searching for a sulfate-free shampoo and conditioner that leaves your hair feeling clean, healthy and hydrated? Search no more, because Seen is changing the hair game. Founded by Harvard-trained dermatologist, Iris Rubin, Seen’s gentle hair-care duo is one of our favorites for its performance and offering of both scented and unscented formulas.


FRAGRANCE-FREE SHAMPOO & FRAGRANCE-FREE CONDITIONER
Seen’s shampoo is appropriate for use during cold capping and beyond, and its creamy conditioner leaves hair feeling super silky so detangling is a breeze.
THE SEXIEST BEAUTY
There’s nothing more empowering than a bold lip. The Sexiest Beauty’s extra hydrating and nourishing formula is long-lasting and comes in a wide range of colors. Founded by a breast cancer supporter and beauty industry veteran, Heather Fink believes sexy is a state of mind, and hopes her products help clients feel more confident and empowered. Pair your new look with a cute turban and earrings for a mood boost during treatment and beyond.

LASH LASH

Does applying false lashes seem like an impossible feat? We thought so too, until we discovered natural-looking lash slices from Lash Lash. The brand was born when celebrity makeup artist, Mari Shten, couldn’t find natural looking lashes on the market — so she created her own. Whether you need to fill in your entire lash line or just a spot or two, these lashes have you covered.
LAMIK BEAUTY
After losing her mother to breast cancer, make-up artist and LAMIK founder Kim Roxie made it her mission to give women of color access to safe, natural beauty products.
Revelation Brow Duo

Eyebrow Stencils
Power Brow Duo Brush

Available in 10 different shades, the Revelation Brow Duo features a powder and cream in a mirrored compact to help you create the thicker, fuller brows of your dreams. Add LAMIK’s brow stencils and brush to your routine for a fool-proof look that’s so easy to achieve.
About Virginia
Virginia Carnesale is the founder and CEO of Stage, an online marketplace, resource and community designed for women with breast cancer. In 2018, Virginia was diagnosed with breast cancer. Through her 18-month journey to wellness, she couldn’t shake the feeling that there was an opportunity to better serve other patients and their loved ones with the knowledge, sisterhood and style tips that only come from walking this road. So in 2021, she put her ideas into practice and created Stage. Prior to Stage, Virginia built a successful 20-year career with top retailers and emerging ecommerce startups in the fashion/beauty industry. Virginia has a passion for product, learning and creating exceptional experiences. Learn more about Virginia and Stage at ShopStage.co.

Cancer Wellness 33
Lashing Out
From working out of her New York City apartment to opening two brick-and-mortar lash spas in sunny LA, celebrity lash expert Dionne Phillips is now using her platform to share her experience with breast cancer to inform and empower others.
BY MEGHAN MCCALLUM
With a storied history in the beauty and fashion industry, Dionne Phillips has provided countless aesthetics services to an international portfolio of customers over the course of her career. Based in Los Angeles, Phillips is a celebrity eyelash extension and beauty expert, and founder of the eyelash extensions brand D’Lashes by Dionne Phillips.
From early beginnings as an aesthetician working out of her kitchen in New York City, Phillips followed her dream to California, where she would eventually open a brick-and-mortar lash spa in the affluent neighborhood of Beverly Hills, called D’Lashes Luxury Lash Spa. Following her breast cancer diagnosis in 2022, Phillips began to combine her professional talents and passion for helping others with her personal cancer experience. Not only does she now provide beauty services for those in or recovering from cancer treatment, she also uses her platform — primarily through Instagram, where she has over 40,000 followers — to educate and empower. In particular, she encourages women to get regular cancer screenings and to self-advocate for their own health.
Looking back, Phillips explains that she first ventured into the world of eyelash extensions while working as a model and actress in New York City, doing her own lashes for auditions. “My Polaroids always looked better with my lash extensions,” she says. Soon enough, with just $65 in supplies, Phillips started her small business in her New York apartment, offering eyelash extensions to other models and actresses.
Her innovative silk fiber lashes and unique talents proved to be a big hit, and through word of mouth, Phillips’ business was soon booked out months in advance. Since moving to Los Angeles in 2005, her celebrity clients have included Serena Williams, Victoria Beckham, Sandra Oh, Paris Hilton and Mindy Kaling, among many others.
As the popularity of Phillips’ work spread in the Los Angeles area, she was connected with a local oncology center and started offering beauty services to patients undergoing cancer treatment, prior to her own diagnosis. Phillips explains these services can provide confidence, relaxation and a sense of normalcy to those experiencing hair loss and other physical side effects of cancer treatment. According to Phillips, eyelashes in particular are slow to grow back post-treatment, and she started gaining more customers for post-chemotherapy extensions as well.
While Phillips’ talent and dedication speaks for itself given her years of success in the beauty industry, her passion became personal following her diagnosis. Like many people, Phillips had fallen behind on her health screenings due to the pandemic. A mammogram in 2019 had been clear, she explains, but after noticing a lump during a self-exam in the shower, she made an appointment for breast imaging. She would ultimately receive her cancer diagnosis following 3D mammogram imaging (also known as breast tomosynthesis — a type of imaging she hadn’t received in breast cancer screenings prior to 2022) and pathology.
Cancer Wellness 34
“I wanted to have my own journey. I didn’t want pity, for people to feel sorry for me.”

Cancer Wellness 35
“I was shocked, but I didn’t cry right away — I was stunned,” she says. Phillips learned that the tumor may have been present in her breast tissue for many years, but had not been detected on her earlier scans.
Phillips soon had a team of doctors who quickly devised her treatment plan. She would have chemotherapy first to shrink the tumor, followed by surgery — the details of which would be decided based on the cancer’s response to chemo. She learned her doctors would monitor the disease through these initial steps and determine whether or not she’d need radiation therapy as well.
Thinking ahead to her five-and-a-half-month chemotherapy regimen, followed by surgery and various other treatments and monitoring, Phillips was initially hesitant to share her diagnosis publicly. She wanted to avoid the unsolicited comments and opinions that often come with sharing a diagnosis, as Phillips knew they would not be helpful for her. “I wanted to have my own journey. I didn’t want pity, for people to feel sorry for me,” she says. Instead, she was determined to “persevere through anything, just like I did when I was getting started in New York,” Phillips says.
While taking ownership of her personal experience was essential, Phillips also realized that sharing glimpses of her life in cancer treatment could help educate and empower others. So when the time came for her chemotherapy port to be installed and to start infusions, she was ready to share her news with the outside world. She posted to social media and even live-streamed her infusion session, telling others about her diagnosis and treatment process. She also encouraged her followers to stay up-todate with their own cancer screenings, and in particular to ask their doctors about 3D mammogram options. While in active treatment, Phillips maintained her positive attitude and energy, and continued to run her lash business. “I’m lashing out on breast cancer!” she wrote in her posts.
Phillips dedicated herself to protecting her positive energy while taking care of her body and mind in the best way she knew how. She had a healthy lifestyle before her diagnosis, but she explains her cancer experience motivated her to ultimately commit to clean, plant-based
nutrition. She also found strength in the mantra, “I am healed and cancer-free.” Combined with her conventional cancer treatment, Phillips says, these approaches helped her manage cancer treatment both physically and mentally.
After completing chemotherapy, Phillips proceeded with a bilateral mastectomy and DIEP flap reconstruction surgery (in which autologous tissue is used to reconstruct the breasts). Phillips then underwent 25 sessions of radiation therapy, which she finished in late 2022 — and, fortunately, led her to achieve her cancer-free status.
Phillips expresses deep gratitude for the success of her treatment and the support from her loving community. While she celebrates her outcome, she knows firsthand why the cancer experience is so difficult — not just for those in active treatment, but even individuals well into cancer recovery and survivorship. Seeing the inside world of cancer enlightened her to the complex challenges of navigating insurance, employment and treatment decisions — not to mention the shock and information overload in those early days of a diagnosis.
While the pandemic “taught us about self-care,” Phillips says, the general public needs to expand this mindset into maintaining regular health checkups as well. Phillips stresses the importance of early cancer detection and genetic testing, in particular. She also strives to normalize self-breast exams as a quick and easy routine to maintain every month. “This is just something you do, like getting a tune-up for your car,” she says.
Phillips carries this experience and knowledge with her as she continues to serve others through her beauty and personal care services. With the opening of her new business location, the D’Lashes Luxury Lash and Wellness Spa, in early 2023, she looks forward to offering additional services that are particularly beneficial for anyone who has been through cancer treatment, including facials and lymphatic massage. Above all, she resolves to continue educating others and urging them to take an active role in their own health. “I will continue doing whatever I can do to encourage others,” she says.
For more information about Dionne Phillips and D’Lashes, go to www.DLashes.com, or find her on social media at @dlashes

Cancer Wellness 36
Supporting cancer thrivers and survivors for over 20 years. www.vogelzanglaw.com 312.796.6167

Cancer Wellness 38
The Light Ahead
Roots & Wings Foundation raises awareness about metastatic breast cancer (MBC), connecting those diagnosed with integrative therapies to help them live longer, healthier lives.
BY CATHERINE EVES
hat can’t be cured must be endured.” This Salman Rushdie quote is a favorite of Diana Keen’s, founder of Roots & Wings Foundation. It’s also fundamental to her foundation’s mission to help members of the metastatic breast cancer (MBC) community live longer, healthier lives. An MBC diagnosis means a person’s breast cancer has metastasized to other parts of the body — it is a stage IV, incurable, lifelong diagnosis.
“W
And despite the severity of MBC, very few breast cancer research dollars are allocated to metastatic types. According to METAvivor, one of the first (and only) foundations dedicated to MBC, only 2% of total dollars raised for breast cancer research goes toward metastatic research, and as approximately 30% of all breast cancers will metastasize, the work of foundations like Roots & Wings is becoming increasingly necessary.
“As a patient myself, I was noticing that there wasn’t a lot of awareness yet about MBC,” Keen says. “Not only do we lack resources and research, the part that we are getting [is] coming up with really amazing things to extend our lives.” Keen has been living with MBC for nine years. She is on chemotherapy, in one form or another, every single day. Chemotherapy is known for its harsh side effects on the body and mind, meaning that research into medicines and therapies that can help alleviate some of these side effects is incredibly important, as it can help the body indefinitely sustain standard cancer treatments, like chemotherapy, radiation and surgery.
“As our days get extended — and we’re so grateful for those days and we fight really hard for them — we need to start taking care of our minds, bodies and souls to endure this constant barrage of treatment,” says Keen. Roots & Wings supports integrative oncology (also known as integrative wellness) programs at hospital systems around the country, raising awareness about the unique needs of the MBC community and connecting patients with integrative therapies like acupuncture, oncology massage, reiki and much more — therapies that became integral to Keen’s own treatment plan from the very beginning.
“I was really lucky that I was introduced serendipitously to integrative oncology,” Keen says. “I don’t know if I would be here so strong and with so much perseverance and grit without it. That’s why I created Roots & Wings.” Keen was young, healthy and had just had a baby when she received her diagnosis. On the same day she was diagnosed, she started treatment at Rush University Cancer Center. “I was in complete shock and denial,” she says.
During that first treatment session, she walked around the hospital’s breast cancer floor and found the
integrative oncology reception desk. She was intrigued by their menu of services but didn’t want to spare the time away from her family. “I thought, if I just got a prognosis in months, why would I spend an hour away from my family and loved ones?” she remembers.
But she made an appointment, picking acupuncture off their menu of services, knowing she could cancel if she changed her mind. “A week after my initial treatment, I had my first appointment with Angela [Lorbeck] at Rush, and it was life-changing,” Keen says. “Angela spoke to me about when getting a metastatic breast cancer diagnosis, it’s really important that I [deal with] the trauma and get myself situated in a mindset that is ready to fight every day.” Keen continued to take advantage of the integrative oncology services — meeting with a functional nutritionist, an oncology therapist, an energy healing practitioner and others to help her manage treatment side effects. Because there is no cure for MBC; instead, it must be endured. “The amount of things that you go through when you agree to be on this journey with MBC is overwhelming,” she says.
But Roots & Wings’ origin story doesn’t just begin with Keen, but with three women Keen overheard during one of her in-hospital treatment sessions. Before her infusion that day, Keen had received an oncology massage, and she was feeling good. “I was so grateful that my body was really clean to accept the infusion,” she remembers. Patients in the infusion room are separated by curtains, but Keen couldn’t help but overhear others’ conversations. Three women in particular were having exceptionally tough days. “They were all different ages, all different demographics, but they all had one thing in common: That day they had no hope they would have any better days,” Keen says. “There I was just feeling so much hope and perseverance from this integrative appointment, and I wanted to give them [this hope].” So she did, assembling a group of eight women to volunteer their time to assist Keen on the mission to “give these three women better days.”
Roots & Wings helps connect MBC patients with integrative wellness therapies at top cancer centers around the country. By helping patients access complimentary appointments or providing the funds necessary to cover their cost, Roots & Wings is also raising awareness about MBC. “It’s our hope that we will inspire the treatments for MBC, engage people with complimentary appointments and continue to grow [existing] programs,” says Keen.
Since its start in August 2020, Roots & Wings has established partnerships with some of the country’s best hospitals, including Rush University Medical Center,
Cancer Wellness 39
Dana-Farber Cancer Institute and Duke Cancer Center, among others. Through grassroots advocacy from Roots & Wings, these top institutions have increased those integrative oncology, or integrative wellness, therapies specific to the unique needs of the MBC community. “Our therapy needs to be different,” Keen says. “We’ll never ring that bell. […] We’re going to be dealing with this until medicine stops working or the side effects from the medicine are [unmanageable].”

According to Angela Lorbeck, manager of Integrative Medicine at Rush, these therapies can be very beneficial for MBC patients. “When a person makes the decision to incorporate integrative wellness therapies into their Western care, it can be a path to personal empowerment and improved health outcomes,” she says. “At Rush, we understand that there are many ways cancer can affect your life. To meet the various challenges associated with cancer, our Supportive Oncology team offers tailored services to support a person’s well-being and quality of life.”
Integrative oncology refers to the many different kinds of healing modalities to complement cancer treatment, but specific therapies and appointments tailored to an MBC
patient include functional nutrition, in which patients can learn how to keep the body strong for ongoing treatment; MBC-specific exercises, as MBC treatments affect things like bone density and the body’s ability to move; oncology massage, as limited mobility can affect the lymph system and how the body gets rid of toxins; and oncology therapy, or talking with therapists who are trained to understand the full scope of an MBC diagnosis. Unlike early stage breast cancer, MBC is a lifelong diagnosis. This is why Keen also wants Roots & Wings to be a resource for an MBC patient who is looking to find a community of people who understand what they are going through. Keen says it is important to treat MBC holistically — focusing on the mind, body and spirit. “You need to find your faith, whatever your faith is,” she says. “I know faith is one of those funny words that has a religious connotation behind it, [but] there’s ways to find faith through community. You have to feel connection, whether it’s through community, religion, yoga, energy work — things that will support your mental health and spirituality.”
That’s why access to services like these, available under the same roof as a patient’s oncology team, is so
Cancer Wellness 40
“I have wild dreams that we’ll be able to [make] integrative oncology available to under-resourced and the under-served areas [for patients who] don’t have the connections to empower themselves or advocate for themselves.”
important. And the medical community is taking note, with some institutions moving toward incorporating integrative wellness therapies into the standard of care. Keen notes that some of the institutions they work with are creating treatment plans that include a meeting with an “integrative liaison” from the start. “[The liaison] will sit with them and talk with them initially about what they might need, help them get those appointments, and will help them with the journey to make sure their mind, body [and] spirituality needs are met,” Keen says, noting that integrative wellness therapies should always be scheduled in conjunction with their oncology team — “not going out and trying things without their oncologist knowing; that’s a really important part of the message,” she says.
Roots & Wings’ impact on the MBC community is significant, despite the organization’s relative youth. Keen’s initial goal was to positively impact the lives of the three women she overheard in her infusion room, but as the foundation continues to grow, so do Keen’s goals. “In the next five years, I would love to create more of a donor base and be able to expand [our reach] to the top MBC institutions from coast to coast, border to border,” she says. “Beyond that, I have wild dreams that we’ll be able to [make] integrative oncology available to under-resourced and the underserved areas [for patients who] don’t have the connections to empower themselves or advocate for themselves.”
Every year, Roots & Wings hosts Move IV MBC, a virtual four-mile event to raise money to provide more MBC patients with complimentary, integrative oncology appointments. Move IV MBC is held around Aug. 8
every year, commemorating Keen’s first day of treatment.
“It was really important for me since 2014, every year on my cancerversary to have some sort of physical challenge, [because] right away I realized [treatment] was going to diminish my ability to move like I used to,” Keen says.
“We just ask you to move — walk, swim, bike or drive if you need to.” Or even dance — this year’s event, “Bust a Move,” will be held on Aug. 6, 2023. “We try to keep it uplifting and fun; cancer is heavy,” Keen says.
Raising awareness about MBC and how integrative oncology can support those diagnosed is so important to Keen because of how beneficial she found those first complimentary appointments at Rush. Despite her initial hesitancy to schedule the appointments, they gave her hope for her future. “If I could do that for someone else, reminding them when they’re in their darkest nights that there’s a light ahead, that it’s not linear; you can have better days even after you feel like you’ve had your worst,” Keen says.
“Integrative oncology supports you and can help you feel better and live better.”
With the recent trend of cancer-care institutions expanding their integrative oncology departments, it’s clear that healing modalities supported by organizations like Roots & Wings should no longer be labeled as “alternative” treatments, but treatments that should be included in the standard of care. “This is life-sustaining support,” Keen says. “I know right now it’s not as en vogue to use battle words, but I am fighting for more time. […] There are days where you’ve got to have every resource possible to get through them.”

Cancer Wellness 41
& The Brightened and Enlightened S ies
presents
TOUCH The Black Breast Cancer Alliance

Breast cancer is killing Black women at alarmingly higher rates than their white counterparts. Ricki Fairley’s breast cancer diagnosis set her on a path to demanding better for Black women — better treatments, better representation in the white-washed world of breast cancer and better opportunities to enable Black women everywhere to be proactive about breast health.
BY CaTHERINE EVES
Cancer Wellness 42
icki Fairley, CEO and cofounder of TOUCH, The Black Breast Cancer Alliance, lives and works by the golden rule: Treat others as you want to be treated. More than a decade ago, Fairley was diagnosed with triple-negative breast cancer (TNBC) and given two years to live, but now 11 years into survivorship, she’s just getting started. She founded TOUCH in 2020 — a practice of her golden rule, even if just in foresight — when she realized she needed to fill an obvious lack in the traditionally white-centric breast cancer space.


Before founding TOUCH, Fairley became aware of some startling breast cancer statistics. “I had been working in the space as an advocate since I was sick, but I started to look at the numbers for Black women, and they’re devastating,” Fairley says. Black women are twice as likely to be diagnosed with TNBC (an aggressive form of breast cancer that is difficult to treat) than white women, and once diagnosed with breast cancer, Black women have a 41% higher mortality rate and a 39% higher recurrence rate than white women. “We started digging back to see if Black women were included in the clinical trials of the drugs that are standard of care [for breast cancer], and we were not,” Fairley remembers. “So I said, ‘Something’s got to be done here.’”
She got in touch with her friend, Valarie Worthy, who had an idea. Worthy was on the board of directors for a nonprofit started 15 years earlier by a fellow TNBC breastie, Wanda Hall McCullough, called Wanda’s TOUCH. Worthy maintained the foundation after McCullough passed away, until handing it over to Fairley in 2020. “When I told her my vision she said, ‘Here’s a 501c3 for you; you have it,’” Fairley says. “[Then] we went to work.”
TOUCH was founded on the hope that one day, foundations like TOUCH will help eradicate Black breast cancer. “We don’t want anyone to die from breast cancer,” Fairley says, “but we at least want mortality rate parity for Black women.” And the first step in getting there, according to Fairley, is to “change the science.”
Fairley notes Black women make up less than 3% of breast cancer clinical trial participants. “Frankly, the drugs aren’t working for us,” Fairley says. “In order to get better drugs, we needed Black women and Black bodies in the clinical trials, in the research.” This is a significant part of TOUCH’s mission — to increase Black women’s participation in trials testing drugs that very well may save their life. And thus, TOUCH’s first campaign, When We Tri(al), was born.
When We Tri(al) makes direct connections with the community to educate and empower Black women for increased representation in clinical trials. Fairley says it’s not enough for Black women to participate at a level commensurate with population, but the burden of disease — again, she notes the TNBC diagnosis rate is three times that of white women. “That should be the number we use to calculate who should be in the clinical trial for TNBC drugs,” Fairley says.
Fairley notes myriad reasons why participation levels are low — first and foremost, doctors are not inviting Black women to participate, either due to implicit bias or blatant racism, says Fairley. And how can we address this deep-seated and egregious problem? Fairley goes straight to big pharma.
When We Tri(al)’s slick marketing has landed Fairley media appearances at places like “The Today Show,” “Oprah Daily,” Dennis Quaid’s “Viewpoint” and more, increasing TOUCH’s reach and helping Fairley make connections across the pharmaceutical industry. “I’m sitting at that table, and I’m holding my knife and my fork [and] I’m not moving until we get better drugs,” Fairley says. “Now we have a voice with pharma to help influence some of their work to get better drugs for Black women.” Whether she’s on a three-hour phone call with AstraZeneca or inviting pharmaceutical reps to TOUCH’s in-person events, Fairley and her team are demanding better treatments for Black women. They’re even working with a company to help design a clinical trial, which includes developing a
Cancer Wellness 43
R
logo, writing the recruiting materials and helping patients navigate the trial once they’ve agreed to participate.
But lack of access is just one reason for the low participation rates. Medical mistrust — developed from centuries of abuse at the hands of the medical industry — means that Black women are reluctant to be part of research studies, but Fairley knew there was more to the story. There was “something within the mind of a Black breastie that was preventing her from participating,” Fairley says. So she teamed up with a friend to conduct a study with 300 Black breasties to help TOUCH better understand how to increase these participation levels. And they learned a lot.
“There’s a severe fear of the unknown. They don’t understand how a trial works. [They think], ‘I’m going to get the sugar pill and die. I don’t want to be a guinea pig,’” Fairley says. But simplifying the information and having it delivered by a fellow Black breastie is the key to alleviate these fears. “I learned pretty quickly [that] I could convince a breastie who was sick to do a clinical trial in five minutes,” Fairley says. “We built WhenWeTrial.org [to] deliver the message for Black women, by Black women, about Black women.” Then, TOUCH hit the road, visiting over 25 U.S. cities from May to November 2022 to connect directly with the community, meeting women where they “live, work, play, pray and slay,” Fairley says. And it was immensely effective — in those six months, TOUCH signed up more than 5,000 Black women into clinical trial ports. “[But] it’s a drop in the bucket of where we need to be,” Fairley says.
TOUCH’S new campaign, which launched Jan. 31, 2023 with the help of their Mission Partner, Bright Pink, is focused on connecting with a younger generation of Black women to help start them on a proactive breast health journey. For the Love of My Gurls is designed to “take the scariness out of cancer [and] make it into this regular thing,” says Hayley Brown, TOUCH’S director of programs and partnerships (and Fairley’s daughter).
With a target demographic of young Black women ages 18 to 35, For the Love of My Gurls is a resource for many stages of life. “We’re in the young women’s space [to] move the needle on this disease state, seeing that Black women under 35 are diagnosed at twice the rate [of white women], well before they would ever reach their first mammogram,” says Emily Powers, TOUCH’s director of strategy and storytelling. The campaign’s mission is to “change the data; change those numbers,” says Brown. “We also want young women to understand their herstory,” she says, so they can take precautionary steps based on shared health history.

The new campaign will also repurpose one of TOUCH’s most popular resources, a weekly show called “The Doctor Is In.” Hosted on BlackDoctor.org (the “WebMD for Black people,” according to Fairley) this show provides a platform for education and conversation about everything related to Black breast cancer, and is hosted by Fairley and Dr. Monique Gary, a breast surgical oncologist. For the Love of My Gurls will bring the popular show to the younger set, focusing on health issues relevant to young Black women and hosted by Brown and a breast surgical oncologist who also falls in the campaign’s targeted age range.
All of the resources they provide and all of their efforts to find commensurate representation of Black women in the breast cancer space aligns with TOUCH’S philosophy — that
to create sustainable, empowered change, you must seek to build the agency, health literacy and self-advocacy of Black women. They do this, in part, with the power of storytelling. “The entire erasure of the experience of the community we work for means that storytelling and representation [are] actually instrumental in getting services, in promoting awareness, in meeting the needs of the community,” Powers says. “As soon as Ricki founded TOUCH, that was a central tenant — [to] start from the stories of the community and build out all of these resources and all of these needs from there.”
“The status quo is not working for black women,” Fairley says. “We have to change things and we have to be different. We live in this world of health and equity — there is no equity here.” Fairley’s reminder to treat others how you want to be treated is a good practice to live a happy and productive life, but for Black women especially, it’s a sentiment that will help save more lives. “If everybody in our ecosystem woke up with that thought and that simple premise every day, we would have different outcomes in health,” says Fairley.
Learn more about TOUCH by visiting TOUCHBBCA.org, WhenWeTrial.org and LoveOfMyGurls.org, or visit them on Instagram: @TOUCHBBCA and @LoveOfMyGurls
Since 2007, Bright Pink has been a national leader in educating, equipping and empowering millions of women to be proactive with their breast and ovarian health. Today, Bright Pink operates as a nonprofit venture philanthropy fund, building on their proven success and deep expertise to find and fund the next generation of groundbreaking breast and ovarian health initiatives. Laser focused on moving the needle on young women’s breast and ovarian health outcomes, Bright Pink has continued to deepen its focus on health equity and finding solutions that remove barriers to care and help save lives. Why? Because despite advancements, millions of women continue to needlessly die of breast and ovarian cancer every year.
Cancer Wellness is partnering with Bright Pink to highlight their Mission Partners — nonprofits that embrace evidence-based practices, make steadfast commitments to ensure health equity and are working toward a common goal. Together, Bright Pink and their Mission Partners have the power to develop systemic change.
That’s why Cancer Wellness and Bright Pink are pleased to announce the “Brightened & Enlightened Series.” Each issue, Cancer Wellness will sit down with officers and executives from one of Bright Pink’s Mission Partners to highlight their triumphs in the cancer prevention space.
Cancer Wellness 44
Stand Up & Support Stand Up & Support
BY CATHERINE EVES
 PHOTOGRAPHY BY JUSTIN FOX BURKS
PHOTOGRAPHY BY JUSTIN FOX BURKS
Up To Cancer’s
inspires innovation to help break the
of
for cancer research.
Stand
Stephanie Herron
model
fundraising
Cancer Wellness 45
have an attitude of gratitude,” says Stephanie Herron, chief development officer (CDO) of Stand Up To Cancer (SU2C). “It’s a privilege to do this work, and when I get to the end of my days, I want to know that it mattered.” SU2C is the gold standard of cancer research foundations — in just 15 short years, they’ve funded more than 270 clinical trials testing breakthrough cancer drugs and therapies, and they’ve pledged over $746 million dollars to 3,000 scientists across the world. They’ve been able to do all this because their research model was designed to initiate collaboration, accelerate the pace of cancer research and clear the way for high-impact breakthroughs.
As CDO, Herron is responsible for SU2C’s fundraising strategy, which includes major gifts, corporate philanthropy, digital engagement and innovation. And it’s a formidable position — one that sometimes has Herron logging 13-hour days with meetings across multiple time zones — but one that suits her perfectly. She’s razor sharp, incredibly passionate about improving outcomes for people with cancer, and she has an innate creative drive that has already inspired innovation within SU2C, despite assuming the role only a few months ago.
But the position, nor Stephanie, could ask for anything less. Especially if Herron is to fulfill personal goals in helping the foundation evolve into one that will be at the forefront of supporting research that will, ultimately, “turn all cancer patients into long-term thrivers.” This is the focus of SU2C’s Convergence team, which Herron says is at an important point of understanding cancer biology, prevention and treatment, noting their studies into cancer genomics, the microbiome’s impact on treatment effectiveness and the use of mRNA vaccines to treat cancer. “Aligned with our mission to bring together the best and the brightest minds in cancer, the SU2C Convergence grants unite various scientific disciplines to investigate fundamental questions about cancer biology and to reimagine the way we bring promising new cancer treatments to patients quickly,” Herron says. “We won’t stop until every cancer patient is a long-term cancer survivor or thriver.”
Herron, like the foundation as a whole, is understandably hesitant to use the word “cure,” but SU2C’s fundraising model is innovative in that they funnel fundraising dollars into research across the cancer spectrum, bringing together researchers with different skill sets united under one goal. “If you can start to bring these disciplines together and this research together [from] across the world, we really have a chance to defeat this disease,” Herron says. “My hope is that we raise the money that will fund these world-class scientists and researchers, and that through them, we will save more lives, and cancer patients will have less-toxic treatments and better quality of life.”
Herron knows too well how cancer and its treatment can be devastating — not just for the person diagnosed but for their loved ones, as well. In 2005, her brother passed away
from esophageal cancer — a rare and aggressive form called small-cell carcinoma of the esophagus. “I’m close in age to my brother, we went to the same high school together, he was a senior when I was a freshman, he married his high school sweetheart, [who] is a good friend of mine, and I couldn’t believe how quickly it all happened,” Herron says. “That is what led me to want to figure out how I can impact this cancer space; how I can make a difference.”
Herron says the loss of her brother represented a turning point in her life. When he was diagnosed in 2004, she was working in academia as the director of development at California State University Channel Islands. She started volunteering to raise money for cancer research in her personal life, participating in 5k or 10k fun runs. “I felt like it was so important just to be out there,” Herron says. “That’s where it started. […] All of my experiences in philanthropy, in business, personally, have led me to Stand Up To Cancer — led me right to the place I am today.”
Herron’s career in cancer research fundraising spans more than 20 years, but she’s been working in the nonprofit space since the early 90s, when she became executive director of a downtown revitalization organization in Bristol, Tennessee. “It really showed me the power of when a small group of passionate people […] come together, what can be achieved,” Herron says. Following her brother’s diagnosis, Herron knew she could harness this power and aimed to refocus her career on “the fight against cancer.”
“What I love about Stand Up is it’s not just focused on one cancer, it’s across the spectrum of many different cancers [and] studying how and why cancer takes hold,” she says. Initially, she was intrigued by SU2C’s founding, noting media personality Katie Couric and the former CEO of Paramount Pictures Sherry Lansing, along with a “group of really extraordinary women” that were all connected to the entertainment industry.
“And each one of the SU2C founders has a different story about how cancer has touched their lives,” says Herron. “These women banded together to say, we’re not scientists, we don’t know what we’re going to do here, but we know we want to do something to save more lives and to advance how cancer is detected, how it’s potentially prevented [and] how it’s treated.”
SU2C is unique in that they were the first to establish a “collaborative, multi-institutional research model,” according to Herron, which has resulted in remarkable progress in the organization’s 15 short years, including the development of nine FDA-approved therapeutics. Herron notes that the traditional research model rewards individuality and individual discovery, but SU2C aims to foster collaboration among researchers across disciplines and institutions. “For its time, it was a totally revolutionary model,” says Herron, adding that other organizations noted SU2C’s success and followed suit. “[SU2C] challenged the status quo.”
“I Cancer Wellness 46
“My hope is that we raise the money that will fund these world-class scientists and researchers, and that through them, we will save more lives, and cancer patients will have less-toxic treatments and better quality of life.”
One pillar of their fundraising model — drawing on the renown of stars from film, TV, sports and journalism to encourage donations and help SU2C become a household name — is also one-of-a-kind. “Because of [SU2C’s] relationship and involvement with the entertainment industry, we are the beneficiary of very unique integrations that celebrities bring forth, and it’s a wonderful partnership,” Herron says. Perhaps most well-known is SU2C’s live telecast, which occurs every two years and features well-known celebrities coming together to highlight SU2C’s collaborative research, share patient stories, perform live music and collect donations from the public. Past telecasts had appearances by Reese Witherspoon, Sofia Vergara, Tom Hanks, Matthew McConaughey and many, many more.
Those in the cancer community know SU2C’s name well, but it would be difficult to find anyone who isn’t at least vaguely familiar with the organization — especially given major corporate partners like Major League Baseball, American Airlines and Mastercard, to name a few. “It’s really interesting, as I’ve gotten to know more of our corporate partners especially, how often the leaders of the organization or the employees [have all] somehow been touched by cancer,” Herron says, noting how SU2C’s partners share a genuine commitment to advancing cancer research.
Herron believes it’s this thread of authenticity that will carry SU2C into the future. “We will continue to be an honest broker and break down barriers and support multi-disciplinary, multi-institution, multi-country [research efforts],” Herron says. SU2C is funding research into immunotherapy, disease progression, the role of the microbiome in preventing and/or treating cancer and so much more. Again, Herron nods to SU2C’s commitment to innovation, sharing that they will continue to fund “highrisk, high-reward” grants, awards and early career investigators.
“What I mean by that is, we want to fund young investigators, or early career investigators or ideas that are so novel they have a hard time getting funding from traditional sources,” Herron says. “You’re going to see Stand Up To Cancer continue to drive access to [SU2C]-funded

Cancer Wellness 47
clinical studies and continue to drive our mission into medically underserved communities.” Looking ahead five or 10 years, SU2C also wants one of their focuses to be on artificial intelligence and its potential to further accelerate cancer research. “I really do think this is the decade in which we’re going to see major breakthroughs in the prevention and treatment of cancer,” Herron says.
Being pulled in so many different directions undoubtedly results in hectic days for Herron, but it also allows her to flex her creative muscles — “My role for years, really, in whatever fundraising seat, [has had] a creative component,” Herron says, explaining that fundraising strategies are often “audience-led,” and it’s Herron’s job to determine what messaging will have the greatest impact. “When you think about fundraising, you have to first create awareness, and then get people to take action, and how do you do that?” she says. “There are those creative through-lines, [and] I really enjoy that part of the work.”
Herron knows the importance of nurturing her creative spirit out of the office, as well — she’s a gifted nature and bird photographer. “It involves being present in the moment, and I think that’s what really helps me to get centered and renew my
soul,” Herron says. “In our workdays, [we’re] always looking at what’s next, [but] when I’m out in nature, and I’m with my dog or my husband and I have my camera, I’m just right there in that moment, and enjoying God’s creation and the beauty — it really grounds me.” (Herron’s dog, Honey Badger, is rarely far from Herron’s side; they’re pictured together on pages 5 and 49.)
“Being out in nature fills my soul, and it gives me the energy and the quiet that I need, but also the creative outlet that I need,” Herron says. Wherever her day-to-day life takes her — flying across the country to meet with donors, waiting patiently for a new species of bird to find its way behind her camera’s viewfinder, and everywhere in between — Herron’s passion rings true. “I have experienced tremendous personal loss, [and] you can focus on the grief, or you can choose to take these life experiences, and say, ‘What am I going to do with this life, to change the outcome for other families?’ And that’s what fuels me,” she says. “I think there is incredible power when you live your life with purpose.”
Learn more about Herron and Stand Up To Cancer at StandUpToCancer.org

Cancer Wellness 48
“It’s a privilege to do this work, and when I get to the end of my days, I want to know that it mattered.”

Cancer Wellness 49
Artists of the Cancer Community
These six artists have all been touched by cancer — as supporters, survivors or thrivers. Here, they share creative works inspired by the cancer experience, each one utterly unique but with a shared message of perseverance and hope.
BY CATHERINE EVES
PATRICIA MARKOS DOLAN
“I always tell my children: Look at your journeys as white canvas. You can create what you want,” says artist Patricia Markos Dolan. “In creating, be open to the universe and allow it to speak to you.” Dolan’s works have been in group and solo exhibitions for more than a decade. Taking a message from the universe, she finds inspiration for her pieces from her Greek heritage juxtaposed with her current home of Winnetka, Illinois.
“Greek was my first language; it was my core,” she says. “At my present moment, I’m in a different culture, [but] all cultures are fused together. We’re all the same, and that’s what makes us one. So on the canvas is where it becomes one for me.” Gazing at one of Dolan’s paintings hanging on a gallery wall is an experience unique to each person, allowing them to tell their own story of love or grief, joy or pain. “As we experience life, all our challenges, our love, our loss, everything, will put us in a deeper consciousness,” Dolan says. “As I work with my paint on the canvas, it starts taking its own form, its own story — It’s void of any human presence. It allows the individual to place themselves in their own existence.”
This spring, Dolan has decided to donate the proceeds of one of her paintings to the Hippocratic Cancer Research Foundation (HCRF). “When creating the piece, I felt the optimism and the power of now through visual and emotional healing, allowing our internal positive voice to surface,” Dolan says. The piece — Θετικα , Thetika — means “Positively,” according to Dolan, and her donation to HCRF reflects the organization’s “commitment to relentless research in discovering breakthrough treatments through holistic approach to integrate the full spectrum of cancer from all angles,” she says. “Their innovative approach is incredible and inspired me to bring Θετικα into existence.”



Cancer
50
“ Θετικα” by Patty Dolan
Wellness
“Art helps us to accept and explore our emotions, to embrace our choices, foster self-compassion, connect with others, discover how we feel to alleviate stress and create calm in our life. Whether it’s in a journal, on a canvas or drawing with chalk on a sidewalk with the kids, taking that time each day to stop, breathe, be mindful and reconnect with yourself will help heal the mind, body and spirit.”
 — Christine Wilson
— Christine Wilson

Christine is a licensed medical massage therapist based in Saint Charles, Missouri. Through her work, she has seen how stress manifests in the body, and promotes the value of self-care to help manage her clients’ stress and anxiety. This became all too important in Christine’s personal life when she was diagnosed with breast cancer in the spring of 2019.
“I had many breast cancer clients, so I didn’t ask ‘Why me?’ I knew the odds,” Christine says. “I needed to take a hard look at how I handled stress and how I took care of myself.”
Christine knew the most important part of self-care is making time to do something that brings you joy. “For me, that was painting,” she says. She taught herself how to watercolor paint a few years earlier as an outlet to help manage her mental health — “[It was] a healthy outlet for bad dating and my hospice work,” she says — but she struggled to find this inspiration during cancer treatment. Her therapist told her to give it time, so Christine continued to watch art-making videos and treated herself with art supplies after radiation sessions.
“Love & Light” by Christine Wilson (2022)
CHRISTINE WILSON
“ Συχνά
Cancer Wellness 51
” by Patty Dolan
“After treatment was done, I literally made myself sit down at my art table and put a brush in my hand, [because] you have to start somewhere,” Christine says. “I needed to find that spark again. It doesn’t have to be a masterpiece; simply just enjoy the process. And do you know what happened? Yes, of course I started to paint again.”
She was surprised to find that her cancer experience had led to an evolution in her artistic journey. “It became apparent that nothing made sense to me anymore, so I developed more of an abstract style and kicked perfection to the curb,” she says. “This became a healing process for me and is reflected in my art work today.”
Christine believes good health inspires creativity, and she is now using her experience as a therapist and mixed-media artist to encourage and support others. She owns an art studio in her hometown of Saint Charles, called Heart Centered Studios, where she hosts art-making classes with an aim to decrease stress and anxiety while promoting mindful self-care. “Like a butterfly, we transform, spread our wings and share our beauty with others,” she says.
outlet to relieve stress as well as distract my brain and body in a more productive way,” Mandi says. “I find that redirecting my focus to creating something beautiful for someone else to love allows me to relax, accept and forget. It’s my escape.”
Creating became even more necessary in 2021, when Mandi experienced what she thought was a cancer recurrence. Mandi’s scans came back clean, but she documented the tumultuous time with a series of personal essays, which she published as part of cW’s Slice of Life essay series. Meditating on strong feelings through the act of writing can help cancer thrivers and survivors manage the negative mental health effects of their cancer journey. This was true for Mandi, as she found solace in offering a glimpse into the life of a cancer survivor, so others could maybe feel less alone when faced with similar circumstances.
Mandi has been focusing her visual art practice on “fluid art” over the past few years. Her “bloom technique” creates abstract cells and lacing across the surface of her canvas — lately, she’s been creating one-of-a-kind homeware pieces and accessories with this technique. “I love the fact that the process is partially defined by a lack of control of the way the paints interact, blend and spread,” she says. “There’s so much in this life that we fight to manage, and knowing that the end result of my art isn’t completely up to me frees me up to be playful and experimental. […] Relinquishing control can be liberating.”
Learn more about Mandi and view her latest pieces on her Instagram @chamblessmandi, and read Mandi’s three-part essay series, “Tomorrow I’ll Know,” at CancerWellness.com.
KELSEY TOWNEND
“Cancer survivors, I see you; I feel you and understand you, even when I don’t understand this process, there is an unspoken bond between those who have come close to death and survived, I think, because we all know the reality of surviving can carry some heaviness. They should give us a little heads up about this in the chemo debrief, or maybe they don’t on purpose, because it’s something you can’t quite articulate with words, but I know when I meet another survivor, without a spoken word, it can be felt.”
— Kelsey Townend
In February 2016, Kelsey was diagnosed with stage II choriocarcinoma at 30 years old. She had two young children, but she would have to leave them at home for four long months to receive treatment at the Cross Cancer Institute in Alberta, Canada. “I shaved my head before my hair started to fall out, [which was] my attempt to keep something in my own control,” Kelsey says. Aggressive treatments would allow the greatest chance of survival, but Kelsey, missing her children, wondered, “What kind of survival is it?”
diagnosed with stage IIIC ovarian cancer. Her doctors told her she had a 20% chance of surviving five years, but 14 years later, Mandi is still here, fostering her creativity through writing and creating art.
Mandi was always artistic, but painting became an avenue for healing following her cancer diagnosis. “I needed a healthy

She finished treatment and returned home with emotions that were hard to manage. “What they don’t tell you is what happens in life after cancer,” she says. “There was no going back to anything normal. I felt so angry and sad, as if a large part of who I was before my cancer was gone.” But the memory of everything she had been through reminded her that she was a survivor. “I don’t deserve to be angry, sad, depressed, anxious; I should be making the most out of every single moment I have, [because] they’re all borrowed,” Kelsey says.
During treatment, Kelsey says she was “too ill to do anything beyond survive,” but once back in her hometown she started a cancer sharing circle called The Karuna
Cancer Wellness 52
still here. by
Kelsey Townend

Group. Soon after, during a long family road trip, she started doodling to create a logo for the group. “I was shocked by how quickly my creative side took hold of me,” she says. She continued making art after vacation, and painting became a way for her to release the emotions she couldn’t articulate with words. “Through painting, I was able to release my sadness, my anger and my frustration that had built up over the course of my treatment.” Painting, Kelsey says, “created a safe space for me and brought me a peace I couldn’t find anywhere else.”
Residual treatment side effects like chronic pain can sometimes prevent Kelsey from creating art, but the promise of a blank canvas keeps her spirits up. “I love painting, because although there are definitely days where I cannot paint due to a bad pain day, I am able to create with no timeline; I can paint at my own pace,” she says. “When I finish a piece, I step back, I see the darkness around the areas where I experience most of my pain and the lightness in areas I so desperately want to show the world. […] I think that during treatment, I came close to death, more than once, and to survive, I had to leave pieces of myself behind. When I paint, I feel like I am slowly putting some of those pieces back.”
Visit Kelsey on Instagram @iamlifeaftercancer
JOELY SERINO
Words have always been my best friends. For as long as I can remember, purging my feelings and turning them into poetry soothed and relieved me from anxiety and the effects of chronic illness. Sharing my poems on social media over the past few years has been cathartic. I immediately feel less alone because I know there is someone who can connect with my words.
After I was diagnosed with invasive ductal carcinoma, I knew I needed to once again lean on my poetry to get me through the mental battle of cancer. I wrote every day about the pain, about feeling alone, about hair loss, about chemotherapy and radiation, about the fear of recurrence. It just spilled out of me, each poem like a therapy session, freeing me from mental and physical anguish. However, quickly into survivorship, I started to notice that my ability to write poetry was being stolen by a chemically induced writer’s block — what is often called “chemo brain.” I just couldn’t find the words anymore.
I couldn’t lose my best coping mechanism. I couldn’t just lay my creativity and love of poetry aside, knowing that it was the best way to protect my mental health. So I started writing blackout poetry. This is when you redact words from a piece of text, like a page from a book or a magazine article, and what’s left forms a micro poem. When I can’t write my own words, I borrow them from the pages of books. After I have chosen which words to leave on the page, I black out the rest of the text with artwork that captures the same emotion. Learning how to add illustrations to my blackout poems also helped me feel accomplished again.

My blackout poems usually discuss cancer, living with chronic pain and illness, mental health, or navigating my way through survivorship. I’ve been able to connect with so many other cancer survivors who feel seen in my work. We relate over the sentiment and artwork that each poem portrays, teaching me that creating is a way to bring people together. It has also taught me that we, as cancer patients, can do what we loved before; we might do it a little differently, but maybe with even better results in the end. While I may always struggle with writer’s block, I will never stop writing poetry; I bleed ink. My poetry just looks a little different now. Some may say it’s even better.
Follow Joely on Instagram: @beautifulmesspoetess
Cancer Wellness 53
KATHLEEN CASTAGNOLI, AIFD, CCF
From playing among my grandmother’s Sterling Silver rose bushes to being awestruck by a florist who visited my kindergarten class, flowers inspired me from a young age. While I ultimately pursued a career in journalism, my love of flowers never wavered. When I got burnt out on writing, I decided to take a floral design course at a local community college, and it changed my life. I delved headfirst into flowers and never looked back. I eventually began my own freelance floral design business, specializing in weddings and events; started competing in floral design competitions; and set my sights on higher certifications, namely with the American Institute of Floral Designers (AIFD) and the California State Floral Association (CCF).
It was the evening after I designed a wedding with over 200 guests that I discovered the coughing, body itching and crappy feelings were not actually symptoms of COVID-19, but stage II non-Hodgkin’s lymphoma. To say I was in complete and utter shock was an understatement. I was officially diagnosed on Nov. 1, 2021, and from there experienced complication after complication — from an infection in my chemotherapy port to blood clots in both arms to fluid buildup in my lung. Because of this, I endured many procedures in addition to week-long hospital stays for my treatments, at times receiving up to five different injections in my stomach per day.
Although I couldn’t practice floral design for some time, I missed flowers. I missed getting up at 3 am to hit the Los Angeles Flower Market, putting together bouquets and centerpieces for weddings. Mostly, I missed the ability to be creative and design something beautiful.

So I signed up for a virtual floral class on color theory taught by a few of my mentors. It was a struggle, but I managed to complete one of the student projects. My wife, Kylie, brought in the bouquet I designed so I could enjoy it in my hospital room, where it received many compliments from my nurses. I
remember nighttimes being hooked up to chemo and watching my floral class on an iPad in my hospital bed. Taking part in this class brought a sense of normalcy and brightness to my long and sometimes lonely medical-filled days.

Toward the end of treatment, I was invited by a luxury traveling floral company, Fleurs de Villes, to be one of their featured florists and design a mannequin as part of their “Femme” show highlighting notable women in history. Fleurs de Villes was something I had longed to be part of, but I didn’t know if I would feel well enough or have the stamina to put such a massive floral installation together on my own.
I called one of my best florist friends, Tee Dryer-Torres, and asked for help. From loaning me the use of her floral studio and supplies, to helping me install late into the night, I still get tearful thinking about all that Tee, Kylie and other florist friends did to help bring my female Native American chief, Coronne, to life.
While I’m grateful to say that I am now in remission, cancer has forever changed me. While I may have won the battle for my health, the mental and financial war is far from over. My advice to fellow cancer survivors and thrivers is to be patient and kind with yourself. Getting “back to normal” feels like a fallacy to me; in reality, it’s more about figuring out what’s next. And as I’m starting to learn, there’s absolutely nothing wrong with that.
At the same time, I am forging a new path in my floral journey, perhaps doing fewer weddings and more floral instruction and artistry. Designing and creating flowers — not just for others but for myself as well — helps me heal and continues to inspire that little girl who still loves Sterling Silver roses.
Kathleen Castagnoli, AIFD, CCF, is an accomplished writer, editor and floral designer in Huntington Beach, California. In addition to playing with words and flowers, Kathleen is a coffee aficionado and hockey fanatic, and she loves spending time with her wife Kylie, their 15-year-old son Max and their spoiled puppy Mocha Bean.
Photo by Kathleen Castagnoli
Cancer Wellness 54
Finding Strength in Flowers by Kathleen Castagnoli
Join us on Saturday, September 2, 2023 for the
6 th Annual Mesothelioma Race for Justice!
We can’t run from our problems, but we can run towards a cure. We honor National Mesothelioma Awareness Month through our support and your voice.




Proceeds from the race will benefit the Meso Foundation.

Scan here to register. Use promo code Cancerwellness for $10 off.

Cancer Wellness 55
Tuning In to Hope
Dr. Diane Reidy-Lagunes of Memorial Sloan Kettering Cancer Center combines her training as an oncologist and her passion for helping others by hosting the informative and inspirational “Cancer Straight Talk” podcast.

If you are part of the cancer community, arming yourself with knowledge can be vital to feeling empowered when facing this complex disease. Countless tools are available to help navigate cancer and its treatment — books, pamphlets and diagrams collected after appointments, and even the dreaded “Dr. Google.” It’s a lot to aggregate and sift through, and if we’re lucky, these materials can provide solace and peace of mind. But often what’s needed most is access to person-to-person advice and evidence-based facts to help us feel confident and comfortable on the road ahead.
Dr. Diane Reidy-Lagunes of Memorial Sloan Kettering Cancer Center (MSK) is one such champion of knowledge-sharing. She’s taken on the noble task of sharing her discoveries and conversations developed inside the four walls of one of the world’s leading cancer centers with the outside world. She is the creator and Host of “Cancer Straight Talk” — a podcast unlike any other before it.
“What I’ve learned as I’ve gotten even more comfortable in the world of oncology is the importance of transparency and honesty — and hope,” Reidy-Lagunes shares from her office in the heart of New York City.
BY LEA GUCCIONE
“Even for a patient with an incurable disease, there is always hope.”
As an awarded medical oncologist with a focus on gastrointestinal (GI) cancers, the breadth of Reidy-Lagunes’ work is impressive. “I take care of common bread-and-butter pancreas, colon, appendix cancers, but [I] also have a primary research interest in these neuroendocrine and adrenal cancers,” she explains. “It runs the gamut of different types of malignancies.”
[with] the best available data we have, that can make a connection to anyone touched by cancer, could really be a gift.” Reidy-Lagunes says she loves how the podcast allows her to connect with patients — or anyone interested in cancer content — more broadly. “That’s what my team and I really strive to do,” she says.
And the wide range of topics covered leaves almost nothing out: cannabis and cancer, sexual health following treatment, insurance costs, sugar and cancer; she even has an episode exploring what makes life meaningful — topics that are most likely not being covered during an average oncology appointment. This is not the fault of doctors; the process just isn’t set up for these types of deep dives into very real and very personal discussions, Reidy-Lagunes explains. So, each topic is chosen for that very reason: its complexity.
When she’s not spending her time caring for rare cancers, she’s recording a new episode of “Cancer Straight Talk.” Since its launch in 2020, the podcast has tackled some challenging topics with the intention to help listeners from all walks of life find answers to the questions that arise following a cancer diagnosis.
“I really felt like we were missing out on an opportunity to teach our patients and their loved ones more about the disease,” she says. “I also found that Dr. Google, which can be very helpful sometimes, can also just make the hurricane even more difficult by throwing in these curveballs about what you’re supposed to do that may be inaccurate or, quite frankly, just false.”
“I felt like to be able to have a platform that’s really evidence-based
“I think it’s a responsibility for us to share that type of information so that patients — even if they’re too far from MSK or a cancer center — can get that type of information, which can be critically important in terms of their quality of life,” Reidy-Lagunes says.
“Cancer Straight Talk” allows listeners to take a remarkable peak under the hood — not only on how oncologists work, but how Reidy-Lagunes herself navigates the patient-doctor relationship with tremendous integrity, care and joy. Many find it refreshing to hear interviews with her own patients, as she does frequently on the series, who share personal stories. Reidy-Lagunes makes it clear she knows her patients well.
“My own relationships with my patients have evolved over the years. As oncologists, this is that path we’ve chosen, and I do think it’s a privilege.” she says. “There are brilliant oncologists out there, and a wall doesn’t mean they don’t care. It’s just their way of coping, because we’re all
“Cancer is the great equalizer. [...] It doesn’t matter who you are or how much money you have; whatever it is, anyone can be affected by these terrible diseases.”
Cancer Wellness 56

Cancer Wellness 57
human, and I think that is so critically important.”
Reidy-Lagunes says her favorite episodes are those that feature her patients as guests. “Every episode, we have to have a patient voice in there, because it’s so important to us,” she says. “So, if we have an expert on, where [the episode] really lends itself to the expert, then we’ll make sure we have those soundbites where, at least, we get that patient voice.”
By default, the podcast has developed into a library for Reidy-Lagunes’ patients to browse, full of episodes brimming with helpful and relevant information and advice. Best of all, it’s free. Listeners even have access to episodes in Spanish, reaching as many patients and loved ones as possible.
The thread throughout ReidyLagunes’ work is that she consistently champions health equity and access for all — her podcast serving as just one example. Recently, ReidyLagunes interviewed MSK’s President and CEO Dr. Selwyn Vickers, whose episode discussing “incomplete narratives” is a great starting point for new listeners.
“Cancer is the great equalizer,” Reidy-Lagunes says. “It doesn’t matter who you are or how much money you have; whatever it is, anyone can be affected by these terrible diseases.”
When you peel back the layers of the doctor herself, it’s easy to see why she is so passionate about her work. Her mother is a math teacher, so math and science have always been part of her life, and her father was a New York City firefighter. From an early age, she felt the need to make a difference.
“I knew I wanted to go into a field where I wanted to care for patients, but ideally use the math and science background that I had,” she says. “When I got into college, medicine — and cancer in particular — was just on the cutting edge; you could feel that there were going to be opportunities to have science transform the way we care for patients, but it wasn’t quite there yet. To me, here was the explosion we were waiting for. So, I knew that there was just tremendous possibility to be in the world of cancer research.”
Since joining MSK faculty in 2008, her passion has never wavered. “For me, the most important thing is the patient of today; trying to care

for them and understand,” ReidyLagunes says. “It’s such an absolute, tremendous privilege. Cancer is one of the most terrifying diagnoses that anyone could get, and it shatters your world. [...] So, to be able to help patients navigate that and say, ‘We’ve got a plan,’ is such a tremendous gift for patients and their family members, and for me as well.”
Reidy-Lagunes feels positively about the strides we’ve made in cancer treatment so far, and is hopeful for the future. “We’re headed somewhere really good, I can tell you,” she says with a smile. “It’s very, very exciting that the technology has really exploded. I think AI [artificial intelligence] and other technology is going to allow us to do things much faster.” She cites cellular therapies in particular, which “engineer” a patient’s white blood cells to attack their cancer. “These are phenomenal, game-changing therapies that right now cost a lot of money,” she says, but notes that advancements in technology are quickly changing that.
“I anticipate that a lot of the therapies that we’re doing today that cost up to one million dollars are going to come down to [being] able to do
them in a much more easily translatable way. [...] The more we learn, the more we realize that cancer is probably hundreds, if not thousands, of different diseases,” Reidy-Lagunes explains. “But we’re getting much better at putting all those cancers into different buckets, so that we can appropriately personalize the therapy for these different types.”
Reidy-Lagunes’ mission is to positively impact anyone affected by cancer. “We really want to empower anyone touched by cancer to take a listen and to learn, so that you can live a happier and healthier life,” she says. “We do want to debunk the myths that are out there, and we try very hard to do that, because we want our patients to have the truth, [but] that doesn’t mean that we’re giving up hope — we’re always hopeful.”
Upcoming episodes of the “Cancer Straight Talk” podcast will be driven by listener feedback, so the team would love to hear from you! Email MSKPodcast@ mskcc.org for more information or to submit ideas for future episodes.
Cancer Wellness 58

One (Potentially) Giant Leap for Mankind
Creating a single test to detect multiple cancer types is one goal of President Joe Biden’s Cancer Moonshot Initiative, but how close are we to making this dream a reality?
BY JOHN OTROMPKE, JD
In a milestone December 2022 webcast, the National Cancer Institute (NCI) described their plan for a multi-cancer early detection test — the first study in the agency’s Cancer Screening Research Network and an important part of the Beau Biden Cancer Moonshot Initiative. Cancer Moonshot was founded in 2016 following former President Barack Obama’s final State of the Union speech, and has the goal of reducing cancer deaths by half within 25 years. The National Institutes of Health (NIH) has provided the initiative with $1.8 billion in funding.
The initial effort, a randomized controlled vanguard study, will assess the effectiveness of cancer screening in asymptomatic patients with mammography, colonoscopy and liquid biopsy (or assay) — the latter of which is a multi-cancer early detection method. Each method will be tested on 8,000 human participants.
Participants will be recruited for the trial from 10 to 15 hospitals and hospital systems. “These tools are a screen,” says Dr. Lori Minasian, referencing the methods listed above. “They don’t diagnose cancer. If it gives you a ‘yes’ answer, that means there is a signal that you may have cancer.” Minasian is a clinical oncologist and deputy director for the Division of Cancer Prevention at the NIH. The NIH hopes that smaller pilot studies like this will ultimately help them design a larger study to determine if early detection tests make a difference in reducing mortality, and have shared future plans of a randomized control trial of 225,000 patients.
AN IMPORTANT PART OF THE PLAN
A lot is already riding on multi-cancer liquid assays, as President Joseph Biden described the possibility of “detecting many cancers at once through blood tests” as a “dream [now put] within our reach” in a speech on Feb. 2, 2022, which he summarized again in his Sept. 12, 2022 speech honoring the 60th Anniversary of President John F. Kennedy’s Moonshot Address.


But making the dream a reality hasn’t been easy. In November 2022, Elizabeth Holmes, founder of Theranos, Inc. was sentenced to prison for claiming technology she developed could screen people for diseases using only a comparatively minute amount of blood. In October 2020, the Centers for Medicare & Medicaid Services (CMS) distributed a national coverage determination (NCD) for tests that look for signs of colorectal cancer in the bloodstream, and proposed the agency would pay for assays that would alert providers to the possibility of colorectal cancer at least 74% of the time. However, the only bloodbased test currently available, the Epi proColon test, did not meet the standard, as it had been found in one or more studies to produce false negatives more than half the time. (Medicare does cover ColoGuard, on the other hand, which the 2020 NCD described as “a multi-target sDNA colorectal cancer screening test.”)

Cancer Wellness 60
And as cancer research into genetically targeted treatments has developed over the past eight years — dependent as it is on diagnostics that actually measure genes, potential cancer cells in the blood and other markers accurately — the U.S. government has not been able to dispel arguments that such cancer blood tests are entirely unregulated. (However, the FDA does regulate the laboratories who make them.) Scientists, scholars and public advocates alike note that a special pathway for licensing “companion diagnostics” is not used often enough, according to a 2016 article in the journal Public Health Genomics.
Efforts in Congress to pass legislation regulating these types of blood tests have been unsuccessful so far. Currently, many such personalized liquid assays are regulated as products of clinical laboratories. As the 2022 VALID Act (Verifying Accurate Leading-Edge IVCT Development Act) did not pass, FDA officials recently announced they would issue rules to finally regulate the field.
“We haven’t had a multi-cancer blood test,” says Minasian. “There are a wide variety of different assays that test for different things [to] detect cancer. Some measure circulating DNA, some mutations, while others look for RNA or other biomarkers.” Minasian says the NIH’s 20-plus years of research in cancer biology has resulted in increasingly effective cancer detection tools, but with “no understanding what to use right now in what context,” she says. “Each of these companies said we have this new assay that tests for four, five or 10 cancers — usually a different grouping of cancers. Our goal is to create a network of investigators so we can have the data to provide to physicians, patients and payors that we know how to use different technologies in different contexts,” says Minasian, who noted the organizers of the vanguard trial have not yet decided which assays to test.
A MULTI-PRONGED RESEARCH EFFORT
However, the vanguard study is only one prong of the Biden Administration’s multi-faceted approach to creating one multi-cancer early detection assay. “Seventy percent of cancer deaths are caused by cancers we don’t have a screening for,” says Jody Hoyos, MHA, CEO of the Prevent Cancer Foundation in Alexandria, Virginia. “There are only five routine screenings available right now: lung, colorectal, cervical, breast and prostate. Prevention is not a sexy topic. It’s not financially beneficial, so there are not a lot of companies pouring money into it,” she adds.
Hoyos’ foundation is a member of the BLOODPAC Consortium, which was launched by President Obama in October 2016 to implement liquid biopsies in clinical settings. BLOODPAC’s membership involves academics, start-up companies and health officials — all as stakeholders. BLOODPAC is not the only group to come out of the cancer blood test arm of Cancer Moonshot. There is also the Liquid Biopsy Consortium, which is in its fifth year. “The mandate of this academic-industry partnership is that as technology is being developed, there needs to be an industrial partner,” says Professor David Wong, DMD, DMSc, the director of oral and head and neck oncology research at UCLA and the chair of the Liquid Biopsy Consortium.



Wong said the funded academic participants in the Consortium partner with university corporate spin-offs: Harvard’s Massachusetts General Hospital with a company called Exosome Diagnostics, Johns Hopkins University with Thrive, and Wong’s group at UCLA with Liquid Diagnostics. According to the NCI, the groups were divided into two teams, but Wong could not confirm that. “At least two of the groups in the consortium are looking for a non-bloodbased liquid biopsy,” says Wong, noting that his own group at UCLA is researching the use of saliva or cerebrospinal fluid to detect lung, gastric, and head and neck cancers.
The carrot used to get the researchers to work together was government funding — Wong’s project was funded for $5 million. Another group, the Brain Liquid Biopsy Consortium, is trying to solve the biological problem of the brain-blood barrier, which some fear may prevent cells and other biological material (which could indicate the first arrival of deadly brain cancers) from leaking out into the general bloodstream, among other functions.
AVOIDING FUTURE DISASTERS IN THE INDUSTRY
Despite advancements over the past decade in blood tests, genetics tests and other personalized assays, none have been subjected to the same rigorous requirements as biopharmaceutical drugs and devices to prove they are safe and effective before being made available for clinical use. But that was in flux even before the global pandemic, says Carmel Shachar, JD, MPH, executive director of the Petrie-Flom Center for Health Law Policy, Biotechnology and Bioethics at Harvard Law School.
“These laboratory-designed tests were regulated by a CMS structure which looked at lab practices. Is the lab doing good practices? Is the test doing what it says it’s doing? They look at [if] the lab [is] doing the test correctly, but they’re not looking at the clinical validity of the test,” Shachar says. “But there was a lot of regulatory ink spilled after the start of COVID-19, because as of December 2020, an at-home COVID kit does need FDA premarket approval.” Shachar notes a concern of self-collection kits is the greater potential for error, compared with tests administered by trained professionals. “Judging from those regulations, an at-home, laboratory-designed test would need FDA approval,” Schachar adds.
“The most remarkable example in the last couple of years was Theranos, which argued that their products fell under the laboratory-designed test rubric, and so managed to escape FDA oversight. Perhaps things could have been flagged earlier,” concluded Shachar.
Otrompke, JD, is a bar applicant in New York City.
John
Cancer Wellness 61
“Seventy percent of cancer deaths are caused by cancers we don’t have a screening for.”
A Picture Worth
BY FRANCESCA HALIKIAS
According to Merriam Webster, “resilience” is the “ability to recover from or adjust easily to misfortune or change.” With the help of his wife, Nicole, photographer Ramzi Mansour created a book of the same name, exploring the many ways in which a cancer diagnosis can both devastate and inspire, take strength away but restore it anew.
“My father had cancer when I was young, and I will never forget the toll it took on my family,” explains Mansour. “It was one of the most terrible times in my life as a young boy, and one that made me grow up very quickly.” The book, which features the stories of 42 women, gives firsthand accounts of their unique cancer journeys, through diagnosis and treatment, as well as what inspired them to keep going despite it all. Each portrait is in Mansour’s signature black-and-white style and accompanied with interviews conducted by his wife, Nicole.
Mansour wasn’t always a photographer. Before he was behind the lens, he was a businessman. After the birth of his second child and his family’s international move, he decided to play around with one of his passions: photography. He bought his first camera and started taking pictures of his family and friends, and one of those shots ended up at a modeling agency. The agency asked if Mansour would be willing to take more pictures, and the rest is history. The more time Mansour spent with his camera, the more he learned about himself. “I started looking at pictures and people in a different light,” he says. “For me, taking someone’s photograph signifies a moment in time in that person’s life that will be remembered forever. This
inspired me to create pictures that tell stories of how I view the subjects using my camera.”
After shooting the cover image for a magazine publication centered around South Africa’s Cancer Awareness Month, Mansour quickly realized he could combine his black-and-white portraiture with his desire to tell a meaningful story. “That was how the concept of our book, ‘Resilience,’ was born,” Mansour says. “We wanted to present a raw and authentic insight into the experiences of South African women as they journeyed with cancer.”
Nicole was the one to convince Mansour to embark on the “Resilience” journey, using her background in journalism to conduct interviews with all 42 women featured in the book. “It was [Nicole’s] ability to truly connect with each person and to create a safe space that allowed them to be vulnerable and authentic,” Mansour says.



With the interviews and photoshoots taking place at the height of COVID-19, both Mansour and his wife had to take extra precautions and handle each profile separately. They needed to be cognizant of each woman’s physical capabilities, as well as emotional well-being. Over 2,000 hours were spent on the project, and 2,500 free copies of “Resilience” were sent to cancer wards and hospitals around the world, with over 300,000 downloads of the e-book. Mansour’s mission of using his talent to touch others in a meaningful way is well on its way to completion.
Each story in “Resilience” shows a unique viewpoint on cancer and the many ways it can impact an individual’s life — making them want to run, cry, hide, fight and live each day as if it were their last. Mansour wanted the
Ramzi Mansour and his wife, Nicole Mansour, showcase 42 women’s strength, beauty and vulnerability in their photography book, “Resilience.”
Cancer Wellness 62
a Thousand Words
book to show that despite each cancer journey being different and highly personal, there are shared experiences and connections to be made with other people walking a similar path. “I hope that ‘Resilience’ can offer anyone on their path with cancer, or any other hardship in life, to take solace in reading that they are not alone,” says Mansour, “and to read of everyday women who journeyed with cancer and how they approached it. The book is filled with hope.”
In hopes of reaching a wider audience, Mansour also made the book available as a free online download. Knowing the fear he went through when his father was facing cancer, he hoped that as many people as possible, whether cancer warrior, thriver, supporter or caregiver, could use this book as a way to know they are not alone. “If this book can somehow bring a glimmer of hope [or] shine a light in a dark tunnel, or resonate with and lift the morale of just one person, then I know that what we set out to do has been realized,” says Mansour.

The title of the book came from a common thread Mansour says he and his wife noticed through each woman’s cancer story: “The resilience of the human spirit to face and walk through seemingly insurmountable odds,” says Mansour. We all will face our own hardships, he explains, but the true connection comes from hearing how others faced their battles and walked their journeys.
As for Mansour’s favorite part of creating “Resilience,” his highs intertwine with his lows. From meeting the women and photographing them, to distributing copies around the world and to the public, Mansour loved every minute of the process. However, two of the interviewees in the book passed away upon nearing the completion of the project. “Their losses were truly felt by the whole team,” says Mansour. “And, feeling much sadness, we resolved to honor these women as best as we could by continuing to share ‘Resilience’ with the world.”



The whole experience of “Resilience” has made Mansour look for more projects with meaning attached to them. He and his wife are already bouncing ideas for a new book they can create together. The most important question that Mansour asks himself, however, is this: What are you doing with the platform you are given? “How will I use my platform to empower and inspire others?” he says. “How will I support my fellow human being? To me, this is what humanity is about — connecting us all and supporting each other so that we may face our journeys with a shared sense of togetherness and a reminder of who we really are.”
But above all, Mansour and his wife want to shed light on the women who made “Resilience” possible, and the ones who found beauty and strength amidst the toughest journey of their lives. “These 42 women are the real heroines of this project,” says Mansour. “We have simply told their stories and brought their beauty to the world. They are the ones who have faced their journeys, shared their stories and walked each step of their realities.”
Cancer Wellness 63
In Plain Sight
In a sleepy, midwestern town, thousands of people who lived and worked near the medical medical device sterilization company Sterigenics experienced daily exposure to cancer-causing rates of ethylene oxide. Years later, the community is finally seeking justice.
 BY FRANCESCA HALIKIAS
BY FRANCESCA HALIKIAS
Cancer Wellness 64
In the town of Willowbrook, Illinois, just 30 minutes from Chicago, one might notice the stretches of trees lining the neighborhood streets; the tan stucco strip malls and grocery stores; the expanses of grassy fields and ponds home to ducks lazing around on sunny days. But hidden in plain sight, something more nefarious was putting lives at risk.
From the outside of the modest-looking office building, one wouldn’t think it housed a sort of danger that would toxify the surrounding air for years, with its multi-colored brick, bright interiors from floor-to-ceiling windows and friendly green shrubbery dotting the entrance. But it was in the name — those simple black letters stamped on a white sign on the side of the wall: Sterigenics.
Sterigenics, a medical device sterilization company, was toxifying the air surrounding its Willowbrook plant location with dangerous levels of ethylene oxide (EtO) — a flammable, colorless gas used to sterilize equipment and plastic devices that cannot be sterilized by steam. EtO is a known carcinogen, and Sterigenics, which describes itself as “a global leader in comprehensive sterilization solutions meeting industrial sterilization needs in the medical device, pharmaceutical, advanced applications, commercial and food industries,” had been emitting the toxin since 1985.
Sterigenics states on their website that “EtO sterilization effectiveness depends on its ability to freely diffuse through a product and packaging. All products must be placed in breathable packaging that allows gas to penetrate the sterile barrier and reach all surfaces of the device or product.” Without medical sterilization, hospital patients would have a higher risk of developing infections, but those who work with EtO must also be protected against dangers, as the CDC stresses it should be considered a known human carcinogen.
The reason EtO is used in medical sterilization is because it can react with and destroy microbial DNA, but if the poisonous gas is exposed to humans, it may result in “respiratory irritation and lung injury, headache, nausea, vomiting, diarrhea, shortness of breath and cyanosis,” according to the U.S. Department of Labor’s Occupational Safety and Health Administration. EtO exposure has also been associated with cancer occurrence, reproductive issues, cell mutations and neurotoxicity.
In September 2022, a jury ordered Sterigenics to pay Willowbrook resident Susan Kamuda $363 million for exposing her to the carcinogen. Sterigenics plans to appeal the verdict, reiterating that it has always safely complied with environmental regulatory requirements.
Kamuda developed breast cancer after moving to Willowbrook with her family in 1985. That same year, Sterigenics moved only a third of a mile from her home and was emitting dangerous levels of EtO until February 2019, when the plant shut down following testing from the U.S. Environmental Protection Agency (EPA). More recently, Kamuda’s son was diagnosed with lymphoma, another type of cancer.
According to a September 2022 Bloomberg Law article, Willowbrook’s Sterigenics plant has had over 760 lawsuits filed due to the toxic emissions, with claims the company knew of the dangers of these chemicals in the surrounding air without warning nearby residents.

“Ethylene oxide is a powerful sterilizer but also has cancer-causing properties due to its capacity to damage DNA,” says Jacques Ferlay, informatics officer at the International Agency for Research on Cancer, an intergovernmental agency forming part of the World Health Organization. “Humans are primarily exposed to ethylene oxide by inhalation and ingestion, which can happen as a result of occupational, consumer or environmental exposure.”
According to the CDC, the basic EtO sterilization cycle takes approximately two and a half hours, excluding aeration time. “Most modern EtO sterilizers combine sterilization and aeration in the same
Cancer Wellness 65
chamber as a continuous process,” says the CDC. “These EtO models minimize potential EtO exposure during door opening and load transfer to the aerator.” Aeration is required because EtO is absorbed by many materials, and aeration will remove residual EtO.
In 2019, CBS News Chicago uncovered concerning information about how Sterigenics completes these processes, reporting that Willowbrook Sterigenics workers were allegedly told to dump toxic chemicals into the public sewer system on the company’s orders. Higher ups were also allegedly covering up how much was actually released into the air. CBS says that former workers (who did not want to be identified) explained how “plant supervisors would dump ethylene oxide’s byproduct — ethylene glycol — down the public sewer drains to avoid the cost of shutting down operations.” Former workers also said the company manipulated alarm systems that were in place to warn workers when they were overexposed to dangerous chemicals.
And while the news was a sigh of relief to Willowbrook residents, there are multiple Sterigenics plants throughout the U.S. that must be monitored to ensure this is not happening in any of their other locations. The EPA also published revised regulations in 2020 for Miscellaneous Organic Chemical Manufacturing facilities that require additional controls on certain equipment and processes that emit EtO to reduce risk to surrounding communities. The EPA is continuing to gather information on EtO emissions, and in January 2022 sent requests for information to eight chemical manufacturing entities subject to air emission standards. The EPA announced it is also aiming to revise regulations for commercial sterilizers.
Kamuda developed breast cancer after moving to Willowbrook
her
Even when the alarms did go off, workers were told to ignore them. The article includes testimony from a forklift operator describing the frequent warnings, but “he was repeatedly told to ignore it, not talk about it and just deal with it or find work elsewhere.” This worker was also told to “just open the doors and let the gas out,” and to leave the doors to the ventilation rooms open despite dangerous vapors off-gassing from the sterilized products in those rooms, which would leak throughout the plant. The workers were then told to open all overhead doors to get rid of the gas. This eventually resulted in Willowbrook Sterigenics workers and community residents being exposed to the toxins without their knowledge, leading to untold numbers of cancer diagnoses and, in some cases, death.
moved only a third of a mile from her home and was emitting dangerous levels of EtO until February 2019, when the plant shut down following testing from the U.S. Environmental Protection Agency (EPA).
In January 2023, a deal was reached between Sterigenics and the almost 900 lawsuits filed in Cook County against the Willowbrook plant. Ultimately, the company will pay $408 million to settle these claims. Sterigenics denies wrongdoing, releasing a statement that “years of biased media coverage in the greater Chicago area, the significant costs of posting a large bond in support of the appeal of the Kamuda verdict and the time and expense that would have been required to continue to contest hundreds of additional lawsuits through a multiyear process in the Illinois court system led us to conclude that resolving the pending Willowbrook [EtO] cases would be in the best interest of the Company and its stakeholders.”
While the Willowbrook plant is shut down, that does not bring back any of the lives lost to EtO emissions, and it does not change the outcome of the many cancer diagnoses in the surrounding area. Still, Sterigenics denies all claims of wrongdoing.
Distressingly enough, the EPA knew about Sterigenics and the risks it posed to the people of Willowbrook long before the initial 2019 report. “The U.S. EPA has amassed an abundant body of data about ethylene oxide, its health risks and Sterigenics’ emissions of the chemical to decide a course of action,” a 2019 Chicago Tribune article states. EPA officials said that despite having sufficient data revealing Sterigenics’ toxic emissions, including finding that “the cancer risk in one census tract near the facility was nine times higher than the national average,” it wasn’t able to take immediate action.
Finally, in September 2019, after being temporarily shut down since the prior February, Sterigenics announced in a statement that it would be permanently closing its Willowbrook location due to the “inaccurate and unfounded claims regarding Sterigenics and the unstable legislative and regulatory landscape in Illinois [that] created an environment in which it [was] not prudent to maintain critical sterilization operations in Willowbrook.”
A Facebook group titled “Stop Sterigenics” has almost 8,000 members from all over the nation dedicated to keeping the public up to date on advancements related to any of the Sterigenics locations. Despite having thousands of members, they have developed a strong bond as they unite in the same fight, sharing heartbreaking stories of lives impacted by Sterigenics and anger that it took so long for the Willowbrook plant to shut down for good. However, due to the success of the community’s collective impact on a company as monumental as Sterigenics, other communities around the nation may start to believe they too can make a difference in keeping their neighbors safe from dangers like those posed by Willowbrook Sterigenics.
As for Kamuda, while the successful lawsuit against Sterigenics does not cure her or her son of cancer, it’s a start on holding big companies accountable. “Best three words I’ve ever heard, honestly,” Kamuda said in a September 2023 CBS article about the verdict of her case. “Just such a relief.”
with
family in 1985. That same year, Sterigenics
Cancer Wellness 66
ComesWhatNext
cW’s resident cancer coach reminds supporters and caregivers about the importance of self-care when supporting someone else on a cancer journey.
 BY MIRELA KOPIER
BY MIRELA KOPIER
Iabsolutely love when we devote an issue to the incredible supporters that show up for those battling cancer. The National Cancer Institute’s guide for caregivers reminds supporters to “do something for yourself each day. It doesn’t matter how small it is. Whatever you do, don’t neglect yourself.” I am always preaching about the benefits of selfcare through physical movement, but there are many other ways to practice self-care — let’s get creative. This may be a bit controversial, but I believe in choices and think this one could possibly help some supporters and caregivers: Visit a “rage room.” These types of experiences are popping up all over the world — rage rooms are specially furnished rooms filled with objects to smash to help release rage, anger and frustration. Some therapists believe smashing things in a fit of rage is not the healthiest way to manage anger, but others believe it can provide short-lived relief. Yes, of course caretakers experience feelings of anger. The person they love has been diagnosed with this disease, and that may feel overwhelming, unfair, undeserving, frustrating, inconceivable and everything else in between.
Scott Bea, a clinical psychologist at the Cleveland Clinic, says “repressed anger produces all sorts of problems. The way in which we manage anger is significant.” He says rage rooms provide only short-term relief, and may not make much of a difference in the long run. I agree with this, but if breaking some stuff in a controlled environment gives you even a moment of relief, why not try it out? People have been known to incorporate rage rooms with other forms of self-care, like yoga, exercise, meditation and talk therapy. It’s imperative that you find something that works for you. I also think it is super important to speak to a trained professional about any emotional issues you are trying to manage.
My next suggestion is for caretakers or anyone who wants to give back to the cancer community: knitting. There are many organizations that collect knitted pieces to donate to those on a cancer journey, such as Knitted Knockers, a volunteer group that provides handmade breast prostheses for women who have undergone mastectomies or other breast surgeries. They have patterns for volunteers available on their website and have donated over half a million “knockers” to those in need. Another amazing organization
is Knots of Love. They provide free patterns as well as complete starter kits for those new to knitting. All of the proceeds from their starter kits go to people undergoing cancer treatment. (They also provide blankets for babies in neonatal ICU incubators.) Of course, this may not be for everyone, but from personal experience I have found the act of knitting or crocheting to be very therapeutic. I also believe performing acts of kindness has numerous positive health benefits.
My last suggestion for supporters requires much less materials and research: journaling. Researchers at the University of Iowa College of Nursing conducted a writing study with family caregivers to determine if and how journaling improves health. After 13 studies with 800 participants, they concluded that caretakers who journaled were making fewer trips to the doctor due to reduced stress and the resulting boosts to the immune system. Journaling is your own personal sanctuary that can be practiced however you see fit — regardless of writing experience or skill.
The best part of journaling is the freedom in format. Some people like to get a fancy notebook, some like to use their phones or computers, but some will just use a school notebook. My own journaling practice varies day to day — sometimes I make lists of my thoughts, sometimes complete sentences and sometimes really bad drawings. Every time I put pen to paper or finger to keyboard, I have found it to be a stress reliever. Those who appreciate a little more structure can easily go online for help getting started. Try it out, and visit HopeGrows.org — a site dedicated to providing care for caregivers, with writing tips and prompts to kick start your journaling practice. Whatever approach you take, I ask one thing — try out various self-care techniques until you find one that works for you. If you can’t support yourself, how are you going to support somebody else?
Stay well and enlightened until next time!
Cancer Wellness 67
: Our mesothelioma support group is a safe space for patients and their loved ones to find encouragement, comfort, advice, and fellowship. www.vogelzanglaw.com 312.796.6167 sup • port group / action; a helping hand / Visit MesoSupport.org to join.
































 BY FRANCESCA HALIKIAS
BY FRANCESCA HALIKIAS



 BY AMBER SULLIVAN
BY AMBER SULLIVAN






 BY FRANCESCA HALIKIAS
BY FRANCESCA HALIKIAS

 BY FRANCESCA HALIKIAS
BY FRANCESCA HALIKIAS






























 PHOTOGRAPHY BY JUSTIN FOX BURKS
PHOTOGRAPHY BY JUSTIN FOX BURKS






 — Christine Wilson
— Christine Wilson

























 BY FRANCESCA HALIKIAS
BY FRANCESCA HALIKIAS

 BY MIRELA KOPIER
BY MIRELA KOPIER
