CHAPTER 1 Examination Process
Structure governs function. In the human body, anatomy is the structure, and physiology and biomechanics are the functions. To perform a competent orthopedic examination, a basic knowledge of the specific structure and function of the body part must be matched with an understanding of how these parts work together to produce normal movement (biomechanics). When injury occurs, pathomechanics, such as limping, may result. Conversely, an abnormal movement pattern, particularly one that is repeated thousands of times, such as a shortened stride length when running, can result in injury. The examination process consists of connecting the findings of dysfunctional anatomy, physiology, or biomechanics with the unique circumstances of the individual and correlating those findings to disruption in the patient’s function.
The examination process is repeated throughout all phases of recovery. The effectiveness of the treatment and rehabilitation protocol, and subsequent modification, is based on the ongoing reexamination of the patient’s functional status. Regardless of whether the examination is an initial triage of the injury or a reevaluation of an existing condition, a systematic and methodical evaluation model leads to efficiency, consistency, and accuracy in the evaluation process.
Some findings obtained during an examination will trigger referral to a physician for medical diagnosis and management. The examination process should always attempt to rule in or rule out these conditions. Much of the exclusionary process is intuitive: a patient who is talking is obviously breathing. Findings such as bone angulation associated with an obvious fracture may become evident during the secondary survey. Other findings such as localized numbness may become apparent later in the clinical examination. If the patient’s disposition is not clear, err on the side of caution and refer the patient for further medical examination.
Differential Diagnosis
The differential diagnosis includes all those possible diagnoses that have not been excluded by the examination findings. As the examination continues, many pathologies are quickly excluded. For example, the patient who is walking does not have a femur fracture (ruling out a potential diagnosis). In the case of a patient with an acute ankle injury, the initial differential diagnosis must include the possibility of a fracture that must be ruled in or out during the examination process.
Following the examination, the differential diagnosis often contains more than one possible pathology. If arriving at a definitive diagnosis is necessary for treatment, additional testing, such as diagnostic imaging and obtaining laboratory values, is used to further narrow the differential diagnosis. In some cases, identification of the specific involved structure is not necessary (or even possible) for effective intervention. Many individuals with low back pain, for example, are diagnosed with “nonspecific low back pain.”
Systematic Examination Technique
This chapter describes the examination model used in this text, one of many that are used. A comprehensive examination model must incorporate (1) the justifiable inclusion or exclusion of each step, (2) adaptability to the specific needs of the situation, and (3) the ability to rule in or rule out the possible differential diagnoses.
The examination should gather objective data to better organize, interpret, and monitor a patient’s progress and
Triage The process of determining the priority of treatment
Disposition The immediate and long-term management of an injury or illness
Pathology A condition produced by an injury or disease
Objective data Finite measures that are readily reproducible regardless of the individual collecting the information
develop treatment priorities. Baseline measurements such as pain scales obtained during the initial examination are recorded and referenced during subsequent reexaminations to document the patient’s progress and identify the need for changes in the patient’s treatment and rehabilitation protocol. The initial report serves as the baseline when planning the treatment and rehabilitation program.
The findings of the initial and follow-up examinations and any subsequent referrals must be documented in the patient’s medical record. Besides serving a legal purpose, medical records have an important practical purpose. By using clear, concise terminology and objective findings, the medical record serves as a method of communicating the patient’s current medical disposition to all who read it.
The Examination Model
For the purpose of explanation, the examination model is divided into multiple components, each with a defined objective. Each component, as well as the steps within each one, is presented sequentially, with one task completed before another is begun. Once the basic concepts are mastered, the examination sequence and content vary based on the findings obtained, and more experienced clinicians will
Box 1-1
International Classification of Functioning, Disability, and Health
combine tasks such as inspecting the injured area while conducting the history. Sometimes, too, findings during the examination dictate that components be omitted entirely. For example, when a long bone fracture is suspected, range of motion (ROM) of the adjacent joints should be excluded.
The goals of the examination process are to obtain a clinical diagnosis and to obtain sufficient information to determine a treatment plan that will improve the patient’s quality of life. The need to consider the entire patient (and not just the injured body part) is captured in the World Health Organization’s International Classification of Functioning, Disability, and Health (commonly abbreviated ICF).
The ICF model provides a broader framework for the examination process, encouraging the clinician to consider the patient beyond the immediate examination findings. The principles associated with the ICF model are applied in this text (Box 1-1). For example, identifying activity limitations by observing the patient performing the problematic tasks provides the foundation for the remainder of the examination. The clinical puzzle is to discover the underlying impairments to body structures and function that cause the activity limitations and result in participation restrictions.
Although the physical aspect of the examination is important, this model accounts for all aspects of a condition
Health condition
Body functions & structure
Disorder or disease Participation
Environmental factors
Personal factors
Contextual factors
Traditional diagnostic models focus on the patient’s pathology and tend to neglect the impact of the injury or illness on the person’s ability to function on a personal and societal level. The International Classification of Functioning, Disability, and Health, or ICF, presents a conceptual framework demonstrating that impairments, or identified problems with body structures (anatomical parts) and functions (physiological functions), are inextricably connected to a person’s activity and participation levels.Activities are those tasks or activities that are meaningful to the individual, and participation describes a person’s involvement in life situations.Activity limitations and participation restrictions describe the extent to which the condition impacts a person individually and on the societal level.The model expands to provide individual context for each patient in the form of environmental and personal factors. Environmental factors are the physical and social environments in which the person lives. Personal factors describe the influence of a person’s age, coping habits, social background, education, and experiences on the injury or illness experience.
Box 1-1
International Classification of Functioning, Disability, and Health—cont’d
While the examination process in this text focuses on the identification of impairments and activity limitations, doing this without understanding the resulting participation restriction leads to ineffective treatment. Likewise, not all impairments result in activity limitations. For example, a patient may have decreased ROM in a joint without impacting the ability to perform daily activities. In this example, a treatment approach that focuses on impairment-level treatment (increasing the ROM) will have limited impact on the patient’s quality of life.
The following illustrates the primary components of the ICF model using a sprained knee ligament as the health condition:
Definition
Health Condition
Body Structures and Functions
Interruption or interference of normal bodily processes or structures
Structural, physiological, mental, or emotional impairments
Activity Limitation
Participation Restriction
Restriction or lack of ability to perform a simple task that has meaning for the patient
How the impairment(s) impacts the patient’s ability to perform a task
An inability or limitation to perform in life situations
Examples of Assessment Techniques
Imaging
Lab work
History
Pain questionnaires
Instrumented testing
Joint play
Manual muscle tests
Stress tests
Selective tissue tests
Observation during a functional task such as walking or reaching that is necessary and/or important for the patient
Measurement/Find ing
Ligament disruption
Increased laxity with firm end-feel
Pain at rest = 3.0/10
Pain at worst = 7.5/10
that might influence recovery. For example, patients have a wide range of pain tolerance, apprehension, fear, and desire to return to activity. Each of these components will impact treatment and recovery, further illustrating the need to consider the patient’s unique values and circumstances in the examination process.
Regional Interdependence
The concept of regional interdependence can be illustrated by walking without bending your knee. The resulting gait requires functional (movement) adaptations at the foot, ankle, hip, and lumbar spine. When prolonged aberrant motion occurs at one joint, potentially injurious stresses may be applied to the proximal and distal segments along the kinematic chain.
Historically, orthopedic diagnosis and the subsequent interventions have been derived using the biomedical model that focuses on the underlying pathology. The concept of regional interdependence recognizes that impairments in body regions other than the symptomatic one
Question the patient regarding life impact. Which desired activities is the patient unable to do?
Inability to go up stairs
Unable to participate in football practice (but only if patient wants to participate in football)
can contribute to the patient’s complaints (see Chapter 6, p. 146).1
The Role ofThe Uninjured Paired Structure
The uninjured (opposite) body part provides an immediate reference point for comparison with the injured segment. In the case of an injured extremity, the patient may use the uninjured limb to demonstrate the mechanism of injury (MOI) or the movements that produce pain (Table 1-1). A portion of the history-taking process should be used to identify prior injury of the uninjured limb that could influence the bilateral comparison.
Although the role and importance of the uninjured body part are clear, where it fits into the evaluation process is not. One strategy is to perform each task on the uninjured body part before involving the injured side. The rationale for this technique is that the patient’s apprehension will decrease if the evaluation is performed first on the uninjured side. The other school of thought suggests
Table
Segment
History
1-1 Role
of the Noninjured Limb in the Examination Process
Relevance
Past medical history: Establishes preinjury health baseline and identifies conditions that can influence the current problem
History of present condition: Replicates the mechanism of injury, primary complaint(s), activity limitations, and participation restrictions
Functional Assessment
Inspection
Palpation
Joint and Muscle Function Assessment
Joint Stability Tests
Selective Tissue Tests
Neurological Test
Vascular Screening
Provides information regarding how the condition impacts the patient’s ability to perform relevant tasks; may be influenced by arm dominance
Provides a reference for symmetry, alignment, and color of the superficial tissues
Provides a reference for symmetry of bones, alignment, tissue temperature, tissue density, or other deformity as well as the presence of increased tenderness
Provides a reference to identify impairments relating to available ROM, strength, and pain with movement
Provides a reference for end-feel, hypermobility or hypomobility, and pain
Provides a reference for pathology of individual ligaments, joint capsules, and musculotendinous units, as well as the body’s organs
Provides a reference for sensory, reflex, and motor function
Provides a reference for blood circulation to and from the involved extremity
that testing the uninvolved limb first may increase the patient’s apprehension and cause muscle guarding. This text assumes that the noninjured body part will be evaluated first; however, the urgency of some acute injuries, such as joint dislocations, makes comparison with the noninjured limb irrelevant.
Clinical Assessment
The term “assessment” describes the broad array of techniques used to obtain information regarding the patient’s condition and the impact of the condition on the patient’s life, including physical activity. Compared with acute evaluations, clinical assessments are performed in a relatively controlled environment. In the clinical setting, the clinician has luxuries that are not available at an athletic venue, including evaluation tools (e.g., tape measures, goniometers), medical records, and, perhaps most importantly, time.
An injury evaluation normally includes physical contact between the patient and the clinician. At times, the physical contact may involve areas of the patient’s body— such as the pelvic region or the chest in female patients— that call for the utmost in discretion. Regardless of the area of physical contact or the sex of the patient and clinician, the patient must always give informed consent for the clinician to perform the evaluation. Patients who are younger than 18 years old or who have a cognitive impairment that would preclude an informed consent must have their needs represented by a guardian if at all possible. A patient suffering a medical emergency may not be able to give consent for treatment. In this case, a clinician’s
duty to provide emergency medical care overrides obta ining consent.
History
The most informative portion of an examination is the patient’s history. Identifying the MOI, appreciating the influence of any underlying medical conditions, and understanding the impact of the condition on the patient’s life are examples of information obtained in this component. This process involves asking relevant questions, active listening, and note-taking.2 Although “History” is identified as a discrete step in the diagnostic process, circumstances later in the examination may necessitate that the history be revisited, either to obtain more information or to confirm other findings.
The remainder of the examination refines the information derived from the history. The history provides information about the structures involved, the extent of the tissue damage, and the resulting activity limitations and participation restrictions. When examining acute conditions, identifying the MOI is vital to understanding the forces placed on certain structures. For chronic conditions, a determination of changes in training routines, equipment, or posture will help narrow the diagnostic possibilities and directly influence the intervention strategy.2
Obtaining a medical history relies on the ability to communicate with the patient. The quality, depth, and breadth
Muscle guarding Voluntarily or involuntarily assuming a posture to protect an injured body area, often through muscular spasm
Examination Map: Overview of the key elements of the examination model used throughout this text.
PAST MEDICAL HISTORY
Establish general information
- age, activities, occupation, limb dominance
Establish prior history of injury to area
- When (in years, months, days)?
- Number of episodes?
- Seen by physician or other healthcare provider?
- Immobilization? If so, how long?
- Surgery? Type?
- Limitation in activity? Duration?
- Residual complaints? (Full recovery?)
- Is this a similar injury? How is it different?
Establish general health status (medications, mental status, chronic or acute diseases, etc.)
HISTORY OF THE PRESENT CONDITION
Establish chief complaint
- What is the patient’s level of function? What are the participation restrictions?
- What is the primary problem and resulting activity limitations with regard to activities of daily living (ADLs) and/or sport?
- What is the duration of the current problem?
- Mechanism of injury?
- Self-initiated treatment (ice, rest, continue to participate) and its effectiveness
Establish pain information
- Pain location, type, and pattern: does it change?
- What increases and decreases pain?
- Pattern relative to sport-specific demands
Establish changes in demands of activity and/or occupation
- Changes in activity?
- New activity pattern?
- New equipment?
- ADLs?
Other relevant information
- Pain/other symptoms anywhere else?
- Altered sensation?
- Crepitus, locking, or catching?
FUNCTIONAL ASSESSMENT
What functional limitations does the patient demonstrate?
What impairments cause the functional limitations?
Which are most problematic?
INSPECTION*
Obvious deformity
Swelling and discoloration
General posture
Scars, open wounds, cuts, or abrasions
PALPATION*
Areas of point tenderness
Change in tissue density (scarring, spasm, swelling, calcification)
Deformity
Temperature change
Texture
JOINT AND MUSCLE FUNCTION ASSESSMENT*
Active range of motion
- Evaluate for ease of movement, pain, available ranges (quantified via goniometry)
Manual muscle tests
- Evaluate for pain and weakness
Passive range of motion
- Evaluate for difference from active ROM, pain, end-feel, available range (quantified via goniometry)
JOINT STABILITY TESTS*
Stress testing
- Evaluate for increased pain and/or increased or decreased laxity relative to opposite side
Joint play
- Evaluate for increased pain and/or increased or decreased mobility relative to opposite side
*Compare bilaterally of information gained from the patient’s responses will correspond to the clinician’s communication skills. Sociocultural differences between the clinician and patient may create an unrecognized communication barrier that can negatively influence the rest of the evaluation. An awareness of these differences can facilitate communication and improve patient care (Box 1-2).
SELECTIVE TISSUE TESTS*
Provocation testing
- Stress increases pain/symptoms and/or indicates instability
Alleviation testing
- Application of force decreases pain or symptoms
NEUROLOGICAL ASSESSMENT*
Sensory
- Assess spinal nerve root and peripheral nerve sensory function
Motor
- Determine spinal nerve root and peripheral motor nerve function
Reflex
- Assess spinal level reflex function
VASCULAR ASSESSMENT*
Capillary refill
- Assess for adequate perfusion
Distal pulses
Assess for adequate blood supply
DIFFERENTIAL DIAGNOSIS
Include all diagnoses that have not been excluded by the differential diagnosis process. Ideally, the clinical diagnosis is obtained by ruling out all of the potential differential diagnoses.
DISPOSITION
rognosis
- Predict probable short- and long-term outcome of the intervention
Intervention
- Identify treatment goals (such as return to activity) based on identified impairments, activity limitations, and participation restrictions
Open-ended inquiries are useful during the history-taking process because they encourage the patient to describe the nature of the complaint in detail. Asking questions that can be answered “yes” or “no” limits the amount of information that can be deduced from the patient’s response. Consider the different responses to, “Does your shoulder hurt when you raise your arm?” versus, “Tell me about what makes
Box 1-2
Culturally Competent Care
The information gained during a patient examination must be pertinent and accurate to arrive at the proper clinical diagnosis. The environmental factors described in the ICF model capture the influence of culture on an individual’s response to an injury or illness. Miscommunication or misinterpretation often can occur because of differing cultural conventions between the clinician and the patient, possibly leading to an incorrect diagnosis, inappropriate care, or patient noncompliance.3,4 To minimize this risk, clinicians should learn to:
•Involve patients in their own health care
•Understand cultural groups’ attitudes, beliefs, and values as related to issues of health and illness
•Use cultural resources and knowledge to address health care problems
•Develop care plans that are holistic and include patients’ cultural needs
“Culture” is the values, beliefs, and practices shared by a group and influences an individual’s health beliefs, practices, and behaviors. Evaluating patients within a cultural context helps the clinician gain accurate information. It also conveys concern about the patient as a person, not as a body part or injury (e.g., “my ACL patient”). Therefore, using patient-first language, that is, addressing the patient rather than the condition is more appropriate (e.g., “my patient who has an ACL injury”).
Remember that culture is present, operating, and influencing the interchange in every evaluation (whether the interaction is be tween members of different cultures or within the same culture). The following are some cultural aspects that must be considered during the evaluation process.
History
Clear communication between the clinician and patient is critical for taking an accurate history. Whether you are using verbal and/or nonverbal communication skills, it is important to understand the cultural context in which the exchange is occurring.
•Convey respect: Patients, particularly adult patients, are addressed formally (Miss, Mr., Mrs., Ms.) unless otherwise directed to do so by the patient.
•Language: Barriers can exist when English is spoken as a second language or if the patient does not speak English. Likewise, barriers can exist even when speaking the same language or dialect. Some communication interventions include:
•Determine the level of English fluency.
•Obtain the services of an interpreter, if needed.
•Recognize that dialects are acceptable.
•Avoid stereotyping because of language and speech patterns.
•Clarify slang terms.
•Use jargon-free language.
•Use pictures, models, or materials written in the patient’s language.
•Speak more slowly, not more loudly.
•Ask about one symptom at a time.
To ensure that the patient understands your instructions, have him or her paraphrase what you said. If you are working in a setting where other languages are spoken, consider learning the languages of the patient or obtain the services of an interpreter. If an interpreter is used, speak to, and make eye contact with, the patient, not the interpreter.
• Verbal versus nonverbal communication: The actions of the clinician can be just as important as what is said (or not said). If patients have difficulty understanding what you are saying, they will increase their reliance on secondary forms of communication such as body language and facial expressions. Likewise, the clinician should be familiar with assessing patients’ body language from a cultural perspective, including level of eye contact and use of silence.
• Narrative sequence: Clinicians often ask history questions and expect answers in a chronological order. However, not all patients describe the history chronologically. Some relay what happened episodically, indicating those “episodes” or “stories” deemed important to the injury. Allow patients to respond to the question in the sequence that is comfortable for them. Taking notes will help orga nize the pertinent information.
• Religious considerations: Some religions prohibit or limit the amount of medical intervention that can occur. In organized sports, obtaining cultural information, including religious considerations, as part of the preparticipation medical examination history potentially minimizes the risk of providing unwanted or prohibited care. For example, if an acute injury situation arises where the patient is unconscious, knowledge about the patient’s preferences will assist the clinician in providing care that is consistent with those preferences.
• Family considerations: Including immediate and extended family in the decision-making process is often important. Family members can assist with therapeutic regimens, thereby improving compliance.
• Use of complementary and alternative medicine(CAM); traditional and folkmedicines or practices: Ask patients if they are using home remedies, traditional medicines or practices, herbal supplements, or other healthcare practices not considered a part of conventional medicine.As a clinician, you want to work cooperatively with patients, understanding and respecting their healthcare practices in order to provide the best possible care. In addition, some alternative medicines or treatments may negatively interact with mainstream medical care.
Box 1-2
Culturally Competent Care—cont’d
Inspection
When inspecting your patient, remember that differences in skin pigmentation and conditions must be considered.
• Skin assessment(coloration and discoloration): Skin pigmentation varies between and within cultural groups. Use enough lighting to differentiate changes in skin tone. When inspecting dark-pigmented skin for pallor, cyanosis, and jaundice, check the mucous membranes, lips, nail beds, palms of hands, and soles of feet to determine the problem.
• Skin conditions: Be aware that keloids, scars that form at the site of a wound and grow beyond its boundaries, are most common in African American and Asian patients. Ascertain whether the patient is prone to keloids, particularly if surgery is indicated. There may be steps the physician can take to minimize the scarring.
Issues Regarding Physical Contact
When palpating the patient, care must be taken to touch in a manner that is culturally appropriate.
• Religious considerations: Permission must be granted before touching any patient. In some cultures and religions, the act of physically being touched or exposing body areas may carry with it certain moral and ethical issues.
• Gender considerations: The standard for the “appropriateness” of touching can be influenced by the gender of the patient and the clinician. Some patients may not feel comfortable being examined by an individual of the opposite gender. If a clinician is of the opposite gender of the patient, the process should be observed by a third party (e.g., another clinician, coach, parent/guardian, or family member).
Not all individuals in a given ethnic or racial group behave the same way. The levels of acculturation and socioeconomic status are just two factors that influence healthcare beliefs and practices. Therefore, use this information as a guide during the evaluation process.
your shoulder hurt.” Occasionally, however, when time is critical, such as the immediate examination of an acute, potentially catastrophic injury, closed-ended questions are necessar y; for example, “Can you move your fingers?” (see Chapter 2).
Past Medical History
For nonacute examinations, patients or their parents are usually asked to complete medical history forms that detail baseline information such as any underlying health conditions, prior injuries, factors that might predispose them to injury, and the course of the current condition. Increasingly, clinicians are asking patients to complete questionnaires that quantify the extent and nature of the impact of a condition on a patient’s life. These questionnaires provide valuable baseline information and can be repeated to determine the effectiveness of any intervention. Commonly used outcome measures are described in each Section Opener. When used over a large population, outcome measures help to identify optimal interventions.5
The past medical history portion of the examination includes the items below. Information such as operative reports or documentation from other providers should be reviewed.
■ Previous history: Is there is a history of injury to this region on either side? If so, ask the patient to describe and compare this injury with the previous injury. Was the onset similar? Do the present symptoms duplicate the previous symptoms? Asking about injury to the entire extremity is important because injury to one structure, even though not currently symptomatic,
can impact forces imposed on the adjacent, currently injured structure.
A history of injury to the body area, prior medical conditions, and congenital conditions can predispose the person to further injur y or influence the evaluation findings. If the injury appears to be a chronic condition or if previous injury to this body part has occurred, determine the prior medical intervention. Understanding how similar prior injuries were managed and their subsequent outcome provides a baseline reference for future diagnostic procedures and rehabilitation planning.
•When did this episode occur? Has it reoccurred since the initial onset?
•Who evaluated and treated this injury previously?
•What diagnosis was made?
•What diagnostic tests were performed? (e.g., radiographs, magnetic resonance imaging [MRI], blood work)
•What was the course of treatment and rehabilitation?
•Was surgery performed or medication prescribed?
•Did the previous treatment plan change the symptoms?
•Was there a successful return to the desired level of activity?
Catastrophic An injury that causes permanent disability or death
Symptom A condition not visually apparent to the examiner, indicating the existence of a disease or injury; symptoms usually obtained during the history-taking process
Congenital A condition existing at or before birth
■ General medical health: What is the patient’s general health status and what, if any, comorbidities are present? Athletes are often assumed to be in prime physical health. Unfortunately, this is not always correct. Prior physical examinations, including preparticipation and annual physical examinations, may reveal congenital abnormalities or diseases that could affect the evaluation and treatment of the injury.
The use of medications and other medical treatments now allows individuals to compete with conditions that once would have excluded them from competition. Conditions such as cystic fibrosis, asthma, human immunodeficiency virus (HIV), spastic colitis, Crohn disease, renal disease, hypertension, and undescended testicles may not preclude strenuous physical activity. A prudent examination involves questions regarding the existence of any underlying medical conditions and review of any existing medical records.
The signs and symptoms of certain tumors and other systemic pathologies may masquerade as overuse injuries, strains, sprains, and other inflammatory conditions.6,7 For example, testicular cancer may clinically appear to be a chronic adductor injury. Patients who present with apparent musculoskeletal injuries, but are lacking a relevant history to explain the symptoms or have symptoms that fail to resolve within a typical time frame, must be promptly referred to a physician (Table 1-2). Many of these referral alerts may be first recognized during the acute (on-field) examination (see Chapter 2).
■ Relevant illnesses and lab work: Chronic systemic illnesses or laboratory findings that can affect injury management and influence the healing process should be noted at the time of examination. For example, people with diabetes often have associated sensory and vascular deficits that delay healing and alter pain perception.
■ Medications: What prescription or over-the-counter medications, supplements, and/or herbal remedies is the individual taking? Certain medications impede tissue healing and may interact with any medications used to treat the current condition (Table 1-3).
■ Smoking: Cigarette smoking is associated with a decreased tolerance for exercise, an increased risk for low back pain and musculoskeletal disorders, and an increased risk for cardiovascular disease. In addition, smoking is associated with delayed fracture and wound healing.14
■ Family medical history: Some conditions have a hereditary component, such as osteochondral defects, anterior cruciate ligament tears, or foot abnormalities. A family history of cardiac abnormalities and cardiacrelated sudden death are strong predictors for hypertrophic cardiomyopathy, myocardial infarction, and other heart-related conditions.15-17 The strongest indicator of an athlete’s predisposition to sudden death is a family history of cardiovascular-related sudden
Table 1-2
Referral Alerts
Finding
Chest pain
Dizziness
Shortness of breath
Unexplained pain in the left arm
Unexplained swelling of the ankles/legs
Unexplained weight gain
Unexplained weight loss
Moles or other acute skin growths
Slow-to-heal skin lesions
Blood in the stool
Unremitting night pain
Blood in the urine
Pain in the flank following the course of the ureter
Low back pain associated with the above
Loss of balance/coordination
Loss of consciousness
Bilateral hyperreflexia
Acute hyporeflexia
Inability to produce voluntary muscle contractions
Unexplained general muscular weakness
Bowel or bladder dysfunction
Fever, chills, and/or night sweats
Insidious joint or bone pain
Possible Active Pathology or Condition
Congestive heart failure
Myocardial infarction
Splenic rupture Cancer
Kidney stones
Kidney/bladder infections
Neurological involvement
Amenorrhea
Severe dysmenorrhea
Systemic disease or infection
Ankylosing spondylitis (spine)
Rheumatoid arthritis
Lyme disease
Osteomyelitis
Osteosarcoma
Septic arthritis
Gout
Pregnancy
Ectopic pregnancy
death. The preparticipation examination’s medical history questionnaire must identify any family history of cardiac-related sudden death and any such history warrants full examination by a cardiologist.
Comorbidities Disorder(s) unrelated to the condition for which the patient seeks assistance
Sign An observable condition that indicates the existence of a disease or injury
Sudden death Unexpected and instantaneous death occurring within 1 hour of the onset of symptoms; most often used to describe death caused secondary to cardiac failure
Table 1-3 Potential Medication Effects on Musculoskeletal Healing
Medication (or medication family)
Beta-blockers
Corticosteroid
Cox-2 Inhibitor
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)
Salicylate
Anticoagulant
History of the Present Condition
Generic Name (trade name) Example
Metoprolol (Lopressor®)
Propranolol (Inderal®)
Atenolol (Tenormin®)
Methylprednisolone (Medrol®)
Dexamethasone (Decadron®)
Celecoxib (Celebrex®)
Ibuprofen (Motrin®)
Diclofenac (Voltaren®)
Aspirin
Warfarin (Coumadin®)
The following information should be obtained during the history-taking process:
■ Mechanism of the injury: How did the injury occur? The description of the MOI helps to identify the involved structures and the forces placed on them (see Chapter 4). Was the trauma caused by a single traumatic force (macrotrauma), or was it the accumulation of repeated forces (microtrauma), resulting in an insidious onset of the symptoms? For example, “I got hit on the outside of my knee” describes a mechanism that produces compressive forces laterally and tensile forces medially.
For athletic injuries, practice and game videos can be used to help identify the MOI. These films may allow the medical team to actually view the mechanism and circumstances surrounding the injury.
■ Relevant sounds or sensations at the time of injury: What sensations were experienced? Did the patient or bystanders hear any sounds, such as a “pop” that could be associated with a tearing ligament or a “crack” associated with bone fracturing? Determining the relationship between true physical dysfunction and the reported sensations is useful. For example, true “giving way” or instability would involve the subluxation of a joint (see Chapter 4). The physical sensation of a joint’s giving way, but without true joint subluxation, indicates pain inhibition or weakness of the surrounding muscles.
■ Onset and duration of symptoms: When did this problem begin? With acute macrotrauma, the signs and symptoms tend to present themselves immediately. The signs and symptoms associated with chronic or insidious microtrauma, such as overuse syndromes, tend to progressively worsen with time and continued stresses. In the early stages, patients with overuse syndromes complain of pain associated with fatigue
Potential Negative Effect
Decreased tolerance to exercise coupled with reduced perceived exertion
Prolonged use: Muscle weakness, loss of muscle mass, tendon rupture, osteoporosis, aseptic necrosis of femoral and humeral heads, spontaneous fractures8
Possible inhibition of soft tissue and bone healing9
The effect of NSAIDs on bone healing is unclear. Some studies indicate a delay,10-12 but a systematic review indicated that there was no detrimental effect on bone healing.13
Prolonged bleeding times
Prolonged bleeding times
and after activity. As the condition progresses, pain is also described at the onset of activity and then progresses to pain of a constant nature.
■ Pain: Because of changes in physiology following an injury, acute injuries often have a localized “stinging” type pain. A few hours later, the pain becomes more diffuse and may be described as “burning” or “aching.” Valuable outcome measures to gauge a patient’s progress, the location, type, and severity of pain should be quantified and documented whenever possible (Box 1-3).
• Location of pain: Ask the patient to point to the area of pain. In many cases, the location of the pain correlates with the damaged tissue. Conversely, the patient may be experiencing referred or radicular pain in a region without tissue damage. Often, following an acute injury, the patient is able to use one finger to isolate the area of pain and is more likely to isolate the involved structure or structures. As time passes following the injury, pain becomes more diffuse, and the patient tends to identify the painful area by sweeping the hand over a general area.
• Referred pain: Referred pain, or pain at a site other than the actual location of trauma, can mislead the patient and the clinician as to the actual location of the pathology. Resulting when the central nervous system (CNS) misinterprets the location and source of the painful stimulus, referred pain patterns can indicate internal injury, such as when damage to the spleen results in left shoulder pain (Fig. 1-1). Musculoskeletal injury can also cause
Insidious Of gradual onset; with respect to symptoms of an injury or disease having no apparent cause
Overuse syndrome Injury caused by accumulated microtraumatic stress placed on a structure or body area
Box 1-3
Pain Rating Scales
Visual Analog Scale (VAS)
Pain as bad as it could be No pain
Using a 10-cm line, the patient is asked to mark the point that represents the current intensity of pain. The VAS value is then calculated by measuring the distance in centimeters from the right edge of the line.
Numeric Rating Scale (NRS)
Pain as bad as it could be No pain 012345678910
The patient is asked to circle the number from 0 (no pain) to 10 (worst pain imaginable) that best describes the current level of pain. Only whole numbers are used with this scale. The VAS and NRS are common outcome measures that are used to quantify the amount of pain that a patient is experiencing over time. They are also useful for measuring pain before and after treatment.
McGill Pain Questionnaire
A. Where is your pain?
Using the drawing on the right, please mark the area(s) where you feel pain. Mark an “E” if the source of the pain is external or “I” if it is internal.. If the source of the pain is both internal, please mark “B”.
B. Pain rating index
Many different words can be used to describe pain. From the list below, please circle those words that best describe the pain you are currently experiencing. Use only one word from each category. You do not need to mark a word in every – Only mark those words that most accurately describe your pain.
1. Flickering Quivering Pulsing Throbbing Beating Pounding
6. Tugging Pulling Wrenching
11. Tiring Exhausting
16. Annoying Troublesome Miserable Intense Unbearable
2. Jumping Flashing Shooting
7. Hot Burning Scalding Searing
3. Pricking Boring Drilling Stabbing
8. Tingling Itchy Smarting Stinging
4. Sharp Cutting Lacerating
9. Dull Sore Hurting Aching Heavy
12. Sickening Suffocating 13. Fearful Fightful Terrifying 14. Punishing Grueling Cruel Vicious Killing
17. Spreading Radiating Penetrating Piercing
18. Tight Numb Drawing Squeezing Tearing
19. Cool Cold Freezing
5. Pinching Pressing Gnawing Cramping Crushing
10. Tender Taut Rasping
15. Wretched Blinding
20. Nagging Nauseating Agonizing Dreadful Torturing
Pain assessment instruments such as the McGill Pain Questionnaire are often used for patients who have complex pain problems. In Par t A, the patient identifies the area(s) of pain and whether the pain is deep or superficial. Part B provides descriptors that the patient uses to determine the intensity and nature of the pain. A visual analog or numeric rating scale is often included as a part of the outcome measure.
Figures from Starkey, C. Therapeutic Modalities (ed 4). Philadelphia: FA Davis, 2013, pp. 49-50.
Heart Appendix
Ovaries and testicles
referred pain, such as when rotator cuff involvement refers pain to the insertion of the deltoid muscle.
• Radicular pain: Radicular symptoms can result when a nerve root or peripheral nerve is compressed or otherwise damaged. Radicular pain occurs along relatively common distributions of innervation (dermatomes) and is discussed further in the appropriate chapters of this text.
• Type of pain: When injured, different tissues may respond by producing different types of pain. Pain associated with fractures is often described as “sharp” due to the rich innervation of the periosteum. Nerve pathology can be described as “electricity,” “lightning,” or “pins and needles” extending from proximal to distal (or, on rare occasions, distal to proximal) in the extremity. Sharp, localized “stinging” pain is common immediately following acute injury; with time, the pain will transition to an “aching” or “throbbing” sensation.
• Daily pain patterns: When during the course of the day is the pain worse? Better? What is the pattern during activity? Does the location vary throughout the day? Pain that is worse in the morning and eases as the day progresses may be associated with tissue creep that occurs when tissues are shortened during the night (see Chapter 4). The opposite pattern, better in the morning and worse later in the day, can be associated with muscular fatigue or prolonged compressive forces, as in the case of a herniated disc.
• Provocation and alleviation patterns: What activities or positions relieve and worsen the pattern? The patient’s description of a position that provokes the pain may direct the sequence of the examination and also helps identify what tissues may be stretched or compressed. For example, a patient
Esophagus/ stomach
Spleen
Heart
Spleen
Lung
may describe the activity limitation of increased shoulder pain with overhead movement, a provoking movement that can be replicated during the ROM portion and selective tissue testing portion of the examination. Patients with a cervical disc problem may describe certain positions that decrease pain, such as lateral bending, illustrating an alleviation pattern.
■ Other symptoms: Does the patient describe other symptoms, such as weakness or paresthesia? Does the limb “give out”? Does the patient complain that the extremity feels “cold,” indicating possible arterial involvement, or “heavy,” indicating possible venous or lymphatic involvement? Questioning the patient about the onset of symptoms such as effusion may help identify the involved structure.
■ Treatment to date: Has the patient attempted any selftreatment or sought help from anyone else for this condition? A complete description of medications, alternative therapies, first aid procedures, and any other interventions such as prescription or over-thecounter foot orthotics is necessary to understand the full scope of the condition.
■ Affective traits: Does the patient have any influences that would impede or exaggerate the desire to return
Proximal Toward the midline of the body; the opposite of distal Distal Away from the midline of the body, moving toward the periphery; the opposite of proximal
Tissue creep The gradual and progressive deformation of tissues to adapt to postural changes including immobilization or pathomechanics
Paresthesia The sensation of numbness or tingling, often described as a “pins and needles” sensation, caused by compression of or a lesion to a peripheral nerve
Effusion The accumulation of excess fluid within a joint space or joint cavity
Gallbladder
Diaphragm
Diaphragm R. Kidney
Gallbladder
FIGURE 1-1 ■ Referred pain patterns from the viscera. Pain from the internal organs tends to radiate along the corresponding somatic sensory fibers.
to activity? Patients may understate the magnitude of their symptoms if an injury may prevent them from participating. Sometimes patients may overstate—or exaggerate—their symptoms either as a reason for poor performance or for possible financial gain.
Depression is frequently associated with chronic pain, such as with nonspecific low back pain, and can negatively impact treatment outcomes.18 Questioning the patient specifically about recent feelings of depression and a decline in interest or pleasure in doing things can help identify those with depressive tendencies.19 Fear-avoidance behaviors, where patients opt not to participate in a given activity due to fear of further injury or re-injury, and emotional distress may also be associated with poor outcomes in patients with chronic musculoskeletal conditions; however, treatment plans tailored to the individual may equalize outcomes.20
■ Resulting activity limitations and participation restrictions: What is the patient unable to accomplish and what activities are restricted? As described in Box 1-1, the concept of connecting identified impairments with activity limitations and resulting participation restrictions is key to developing an effective intervention strategy that works for the individual. For example, a runner who experiences pain at mile 20 may not have a disability if his goals can be met with runs of 10 miles.
At the conclusion of the initial history-taking process, a clear picture of the events causing the injury; predisposing conditions that may have led to its occurrence; and the activities, motions, and postures that increase or decrease the symptoms should be formed. The impact of the injury on the patient’s life should be known. The remainder of the examination is used to further investigate the findings obtained during the history-taking process. Expand on the history during the remainder of the examination, backtracking or asking further questions as you follow leads to fully ascertain all the facts regarding the patient’s condition.
Physical Examination
Next in the process is the physical examination, during which the clinician continues to pare down the differential diagnosis, determine a clinical diagnosis, and identify activity limitations and underlying impairments.
Blood, synovial fluid, saliva, and other bodily fluids can potentially transmit bloodborne pathogens such as the hepatitis B virus (HBV) and HIV. All bodily fluids must be treated as though they contain these viruses. The treatment of acute injuries that involve bleeding, postsurgical wounds, and the handling of soiled dressings, instruments, or other blood- or fluid-soiled objects must be managed as if contaminated.
Functional Assessment
Ask the patient to perform those functional tasks that are performed regularly and/or were identified as problematic during the history-taking portion of the clinical examination. The patient might describe problems with tasks during ADLs, such as reaching or walking or during more complex tasks such as throwing a baseball. Consider the underlying impairment that could lead to the activity limitations. For example, painful or limited knee flexion can cause a compensatory hip hike to sufficiently shorten the limb while climbing stairs. The results of the functional assessment form the framework for the remaining physical examination, where the impairments are identified and measured.
Standardized, reproducible functional tests are designed to assess how the body parts work together to produce functional activity (e.g., reaching, one leg hop for distance, ROM, strength, and balance). These assessments are then expanded to replicate the activity to be performed by the patient under the precise demands faced during real-life situations (e.g., running, jumping, stair climbing, stacking boxes on a pallet). Specific functional tests, which can also serve as outcome measures, are described in the Section openers. By assessing a patient’s functional status throughout the course of a condition, the relative effectiveness of an intervention can be determined.
Inspection
The inspection is a continual process that begins as soon as the patient enters the facility. Bilateral comparison of paired body parts such as the extremities or eyes must be performed when applicable, noting and exploring any deviation from the expected mirror image of the contralateral side.
Inspect the injured body part and compare the results with the opposite structure for:
■ Deformity: Visual deviations from normal can be subtle, gross, or somewhere in between. Some fractures and joint dislocations result in gross deformity, with angulation or clear disruption of normal joint contour. Signs of joint displacement or bony fracture warrant ruling out any other significant trauma, appropriate splinting, and the immediate referral to a physician. This process is explained further in Chapter 2.
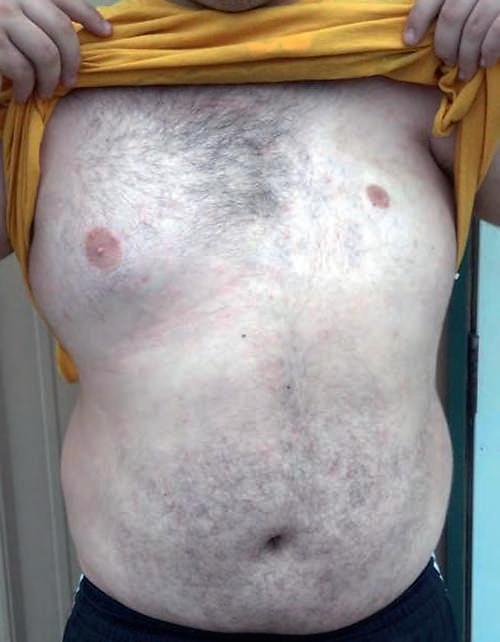
Careful bilateral inspection may reveal differences in otherwise healthy-looking body parts (Fig. 1-2).
■ Swelling: Any enlargement of a body part can be subtle or dramatic and occur rapidly or over time. The onset, look, and feel of a swollen body part can help identify
Contralateral Pertaining to the opposite side of the body or the opposite extremity
Gross Visible or apparent to the unaided eye
the nature of injury. Increased girth (volume) across the joint line relative to the opposite limb suggests the presence of swelling. Increased girth across muscle mass is indicative of hypertrophy or edema; decreased girth across muscle mass is indicative of atrophy.
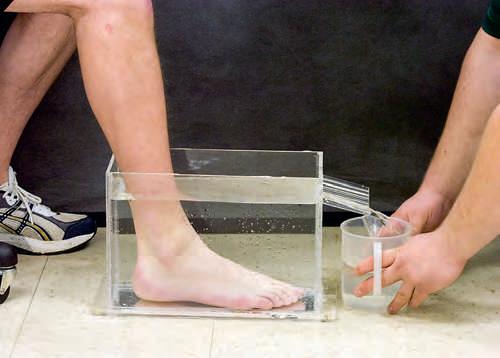
For example, an acute joint effusion resulting from a hemarthrosis is typically readily apparent. Joint swelling that forms over a number of hours or days is most likely the result of excess synovial fluid production. Edema resulting from a tibial stress fracture can be slight and localized. The amount of swelling can be measured in a quantifiable manner using girth measurements (Selective Tissue Tests 1-1) or volumetric measurements (Fig. 1-3). Girth measurements require less equipment and demonstrate high interrater reliability, and results closely represent the results of volumetric measurements.21-23
✱ Practical Evidence
When used to determine muscle volume, most body-composition methods, including girth measurements, tend to be more accurate on males than females because of the overlying adipose tissue layer in females.24 Intrarater and interrater reliability of girth measurement are significantly improved when landmarks are consistently identified and used.
Bwater up to the specified level and the
The overflow water is collected and poured into a calibrated beaker to determine the mass (volume) of the limb. This measurement is obtained by either reading a graduate cylinder or, more accurately, by weighing the water expelled. Volumetric measurement of limb volume is most commonly used as a research tool, but can provide important clinical information. Answer to Figure 1-2: The patient is missing his left pectoralis minor muscle.
■ Skin: Does the area show redness that may be associated with inflammation? Is ecchymosis present, indicating a contusion or other soft tissue disruption? Is the ecchymosis located at or distal to the injured structure? Ecchymosis located distal to the site of injury indicates pooling of the blood secondary to the effects of gravity. Are there any open wounds that warrant referral or first aid? Are there signs of
Hemarthrosis Bleeding into a joint cavity
Edema The collection of fluids in the intercellular spaces
Ecchymosis A blue or purple area of skin caused by blood escaping into the extravascular spaces under the skin
FIGURE 1-2 ■ What’s wrong with this picture? (The answer is given in the legend of Fig. 1-3.) The patient has decreased scapular control. There is no history of trauma to the body area. Carefully observe this picture to determine the cause of the lack of scapular control.
FIGURE 1-3 ■ Volumetric Measurement. (A) The tank is filled with
limb is gently immersed. (B)