
11 minute read
Keeping Personnel and Patients Safe
The VA’s Safe Patient Handling and Mobility program protects nurses and patients.
By Gail Gourley
As the opening month of 2020 reveal the increasingly devastating developments of the COVID-19 pandemic, images of health care workers caring for skyrocketing numbers of patients are prevalent. A shortage of personal protective equipment is just one example highlighting their safety requirements, and those of their patients.
Underlying the crisis and inherent in all patient care, both as part of the pandemic as well as other ongoing health care functions, is the always-present need to transport, move, and reposition patients with limited mobility. The overexertion and bodily reaction from motions like lifting, bending, twisting, and reaching place nurses and other health care workers at high risk for injury, underscoring additional safety concerns.
The Department of Veterans Affairs (VA) has placed emphasis on protecting nurses and patients with its Safe Patient Handling and Mobility (SPHM) program.
Jill Earwood, MSN-HCQ, CSPHP, RN, VHA Office of Nursing Service liaison for SPHM and Asheville VA SPHM coordinator, explained the significance of injuries to nurses.
Referring to a November 2018 article in the U.S. Bureau of Labor Statistics journal Monthly Labor Review, Earwood said, “Previous research on hospitals demonstrated that hospital workers have a higher-than-average incidence rate of injury and illness. And historically, RNs have experienced some of the highest injury and illness rates in health care and the social assistance sector.”
In anecdotal terms, Earwood noted that nursing colleagues observe, “We’re the only profession that looks at a hundred pounds as ‘light weight.’ And it’s because we’ve been expected to manually handle that amount of ‘light weight,’ more than a hundred pounds, repeatedly, every day that we work.”

Sling seats attached to ceiling lifts are one method utilized by the VA to safely move patients in inpatient and outpatient settings.
She continued, “The VA committed to stopping this culture of thinking that we had to lift, and do things differently than a factory worker or construction worker; that we should have equipment to do the work that we’re doing.”
Another issue is that the percentage of bariatric patients continues to increase. “They have more co-morbidities than the average person in the hospital, so they’re even more dependent on us,” Earwood said. “They need us for the activities of daily living.”
An additional factor highlighting the necessity to keep nurses safe, Earwood added, is that “the American Association of Colleges of Nursing says that the U.S. is projected to have a shortage of nurses that’s intensifying as baby boomers age and the need for health care grows. So, all of these things make patient handling a significant issue for nurses.”
Tony Hilton, DrPH, MSN, FNP, CRRN, Veterans Health Administration SPHM national program manager, explained the importance to staff and patients of utilizing technology for patient mobility, stating that all the evidence shows the benefits of “mobilizing patients very early in admission, starting in the ICU.”
She continued, “It’s so clear in the literature and in practice that it’s important to get our patients moving very quickly and very early. The problem is that we’ve manually done it for years and years, and we have been taught to do this using our physical bodies. That has been proven through a lot of literature that the human body is not built to withstand these kinds of tasks that result not only in acute incidents of injury, but chronic injuries. … So we really started looking at it in the VA from a protecting staff perspective. But then we realized all of the benefits to the patients. So, in terms of utilizing the technology, it’s a win-win for our patients and our staff.”
Hilton pointed to VA research in reducing nurses’ injuries, beginning in the 1990s with pilot projects and demonstration sites. “Over time, this initial research group and those pilot facilities started to do work with our regulators and Congress to ask for funding,” she said. “In 2008, we were provided over $200 million in capital funds for overhead ceiling lifts and technology,” showing that “the VA has a serious commitment to really making sure we protect our staff and our patients.”
That initial funding began the VA’s national SPHM program, utilizing proven methods and the latest technology and devices to maximize the safety of patients and staff when moving or lifting patients.
As one example, ceiling lift devices utilize a sling to transfer a person from point to point along an overhead track. “The VA invested a lot of money into ceiling lifts and other technology that was deployed over a few years, from 2008 to 2010 and 2011,” Earwood said. She explained that the best option is the presence of full room coverage, which “allows for staff to be able to mobilize patients from corner to corner, wall to wall, and to the bathroom, without having barriers to care.”
In comparison to floor-based lifts, Earwood said ceiling lifts are preferred because they require less force to push them. “If you have a floor-based lift, you have to actually use force to push the patient that’s in it. Also, the ceiling lifts require zero space for storage. And we know that in hospitals, space is defi- nitely at a premium.”

advertisement
Ceiling lift usage is widespread in the VA. “The good news is that the majority of VA [hospitals] have ceiling lift coverage in at least 50 percent of all the rooms; most are at 75 percent, and some at 100 percent, in the 24/7 spaces,” Earwood said. “But, we’re for- tunate to also have ceiling lifts in other departments, like outpatient therapy, imaging, the EDs [emergency depart- ments] – which are 24/7 but we con- sider those outpatients – and our com- munity-based clinics.
“Ceiling lifts are definitely the choice of technology for those patients who are completely dependent,” Earwood continued, “or if we’re trying to create early ambulation for patients who can’t bear weight, you can actually use a ceiling lift to get them upright, feet touching the floor, but the ceiling lift is actually bearing the weight of the patient. So, patients are able to ambu- late earlier with the use of special slings and harnesses.”
The VA also uses technology for fall recovery. “They have several air-assisted devices that raise [patients] off the ground so that we’re not using a backboard and the strength of as many people as we can get to lift someone off the ground, which is safer for staff, obviously, and safer for patients,” Earwood said.
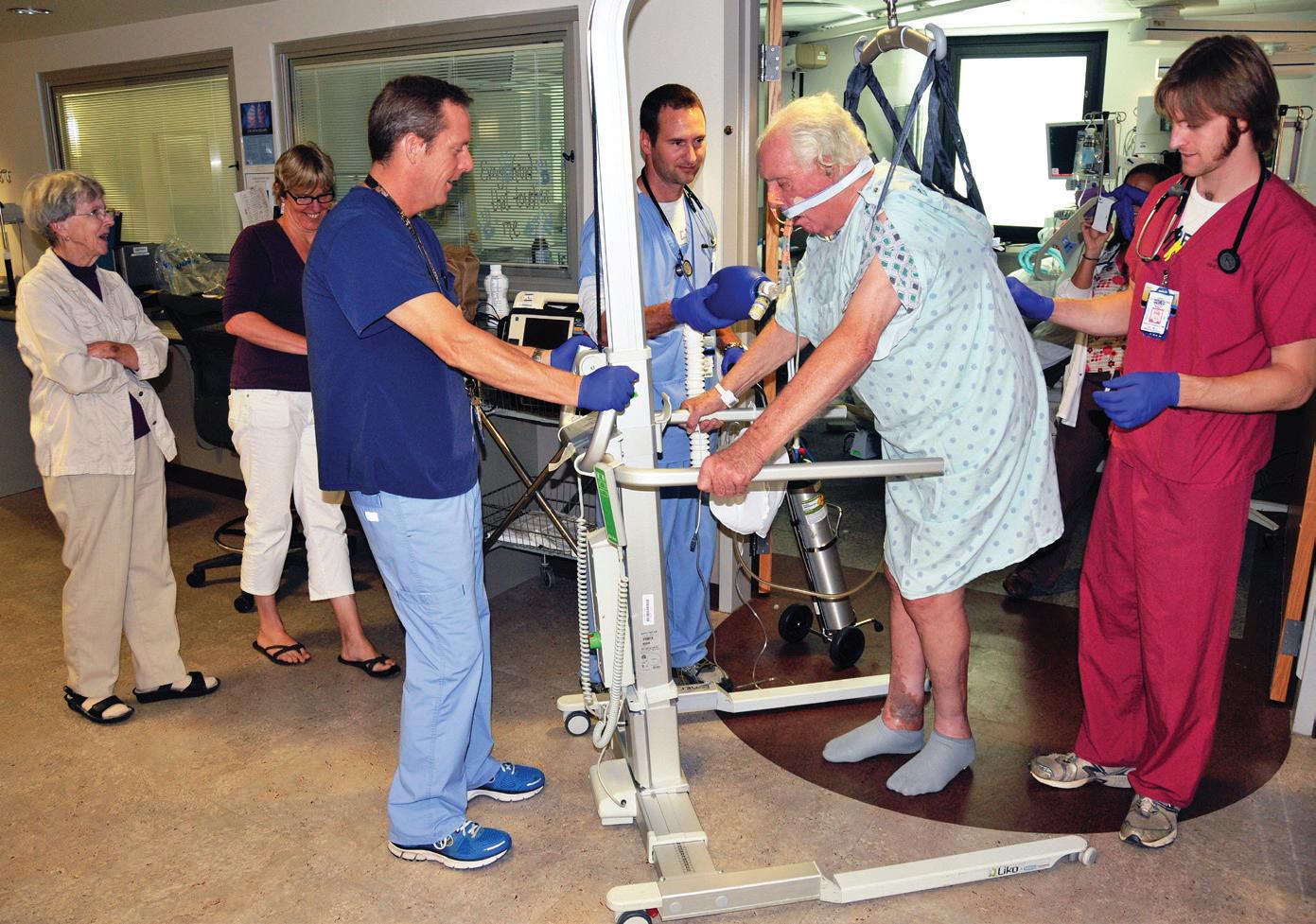
Stand-assist technology facilitates early mobility, which evidence shows is beneficial to patients.
Devices also function to assist patients out of their vehicles when they arrive for emergency care or routine appointments, as well as to help them back into their vehicle. “These devices range from a ceiling lift in a covered area outside, to floor-based equipment that will do this, to using air-assisted technology in an emergency situation where we just need to use that technology to move them from the vehicle to a stretcher,” she said.
“We also have stand-assist devices,” she continued. “Our therapy partners agree, and our therapy partners are definitely onboard. We’ve had conferences where we’re collaborating with therapists – physical therapists, occupational therapists, and kinesiotherapists. We don’t want to limit patients, and we don’t want to do more than we need to when it comes to assisting them, so we have stand-assist devices, both powered and non-powered, for those patients who are able to bear weight and able to use some upper body strength.”
There are also multiple devices for assisting with hygiene. Earwood described mechanical-lift seat toilets. “They function much like the recliners you see in a home, where the recliners raise so that the person can kind of perch on it, and then it lowers so they can sit. These toilets do the same,” she said, adding that this device is especially helpful for postoperative patients following knee or hip surgery. “If they’re struggling with toileting, this is a device that’s great to use for getting them out of bed, getting them to the restroom on their own, and then advancing them on.
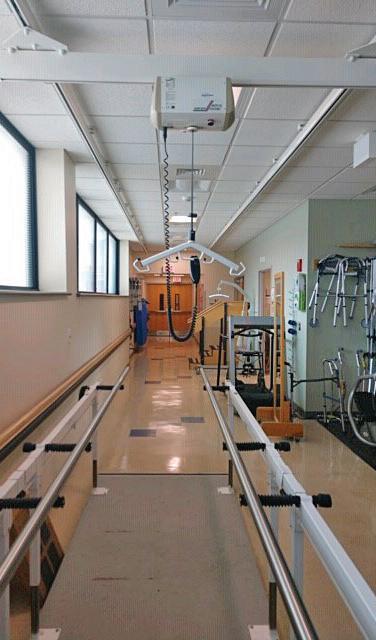
A ceiling lift for gait training enables patients who can’t bear weight to ambulate earlier using special slings and harnesses.
“And we also have mechanical shower chairs now, which are wonderful,” Earwood enthused. Primarily used for residents in long-term care, shortstay rehab, and hospice settings, these shower devices recline, raise and lower, and have protective seatbelts. Earwood said she’s heard story after story from nurses across the country referencing patients who were unable to be in a regular shower chair, and with this device, they “were able to get a shower, instead of maybe a whirlpool bath or a bed bath, for the first time in years.”
Earwood also described simple, friction-reducing devices like slide sheets, which are very effective in moving patients laterally and up and down the bed, or to help move patients’ legs across their car seat if they only need help getting their legs turned.
Motorized stretchers and beds are other technologies that have an impact, as many injuries occurred in the past, Earwood noted, with staff pushing heavy equipment with a patient in them. “Motorized stretchers and beds have definitely made ease of transport accessible to the staff.”
Additionally, Hilton described a powerlift device available for emergency medical services staff, who are also at high risk for injury. The system connects to the floor of the ambulance and lifts the patient on a stretcher into the ambulance, instead of personnel lifting the patient and stretcher manually.
There are many opportunities for innovation in utilizing these devices, Hilton said, such as adapting much of this technology for veterans not only in hospitals but across all settings, including home and community. With the ability to participate in recreation and sports and improve their quality of life, she said, “we think that makes a big difference when it comes to reducing depression scores. All of this has such a huge impact on patients and their families, not only in the acute care setting, but also in the home and the community setting.”

advertisement
To assist health care providers by bringing information about this safety technology and its use to the point of care, the VA developed its Safe Patient Handling App. Hilton said that the app, utilized in VA, non-VA, and international settings, includes video clips of how the technology works, patient assessment algorithms, and other SPHM resources useful at the bedside, adding, “This has been extremely helpful by making the algorithms that we’ve created over the last few years into a much simpler way to get to the answer of ‘How do you do this?’”
Another method for assessing which equipment to use during patient care or movement is the Bedside Mobility Assessment Tool (BMAT), an industrydeveloped instrument widely used in the VA under a national agreement.
Earwood said, “Objective screenings are necessary so that we can decide what [equipment] patients may need at any given moment during care or during movement. BMAT is the only tool that we have now that marries the patient’s response to screening to the equipment.”
Using this tool, a nurse can perform an objective assessment of a patient’s capabilities, asking them to perform physical tasks and observing their response. Based on that response, Earwood said, “you know which equipment you need.”
Training the staff in the use of these SPHM devices is based on the directive requirement, Hilton said, “which includes some very specific criteria that we expect their facility to utilize so we can measure our program outcomes.”
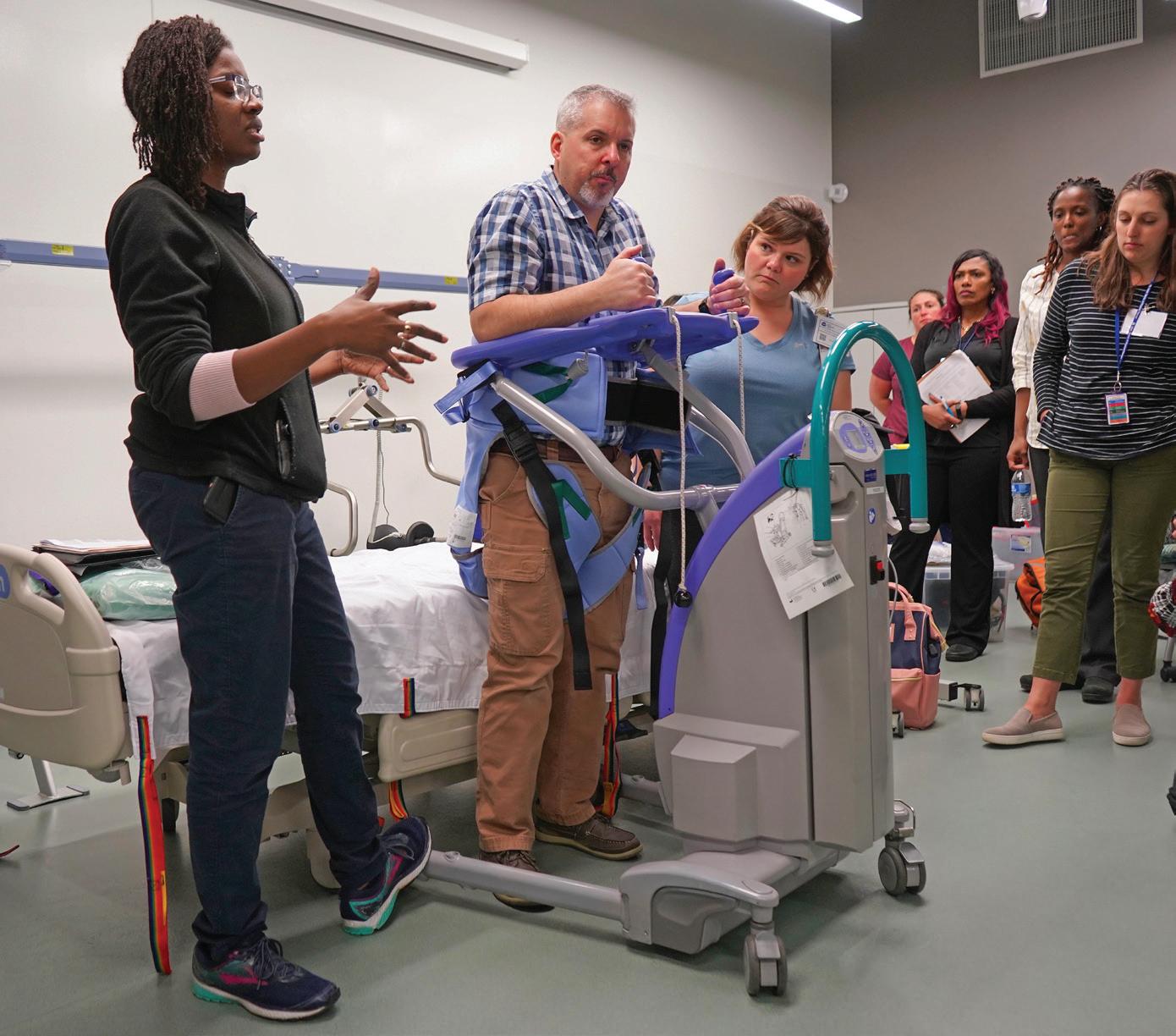
Training personnel to utilize Safe Patient Handling and Mobility technologies is accomplished using several methodologies, including competency development with peer leaders, didactic instruction, and simulation.
She explained that they use several separate methodologies, including an electronic system, new employee orientation with hands-on exposure, and training with a unit peer leader to ensure competency.
Hilton continued, “We have a national conference for [SPHM] facility coordinators, and this is where we not only provide didactic [instruction], but we focus on the simulation of competency within all of our technologies that we offer. This is done at our SimLEARN center in Orlando, at our simulation hospital. It’s a three-day training program where we have simulation happening within multiple settings. … We walk small groups through each of those scenarios so that they can see how they actually use the technology.”
Asked about the biggest barriers and challenges in utilizing this technology, Hilton pointed to traditional nursing culture, which has focused on manual patient handling for years, as well as the fact that traditional body mechanics training was based on moving “boxes,” which are very different from humans. Also, she said, it is not a standard of care in the schools of nursing, where students are still taught manual handling techniques.
“We try to mitigate that by participating in community and university hospitals as faculty speakers, and by getting our staff to really engage with modern-day life technology. One good example is to look at your smartphone. How long did it take to get familiar with your smartphone? And now, you can’t be without it,” she said.
Looking toward the future, Hilton enthused over the exciting potential of the VA’s five-year strategic plan, which will address “improving the employee experience with safe patient handling and all of the components that include ergonomic, education, and learning how to buy equipment,” as well as quantifying improved patient outcomes associated with that care.
The benefits of this technology to personnel and patients are evident. “We’ve been monitoring our staff injuries and found that our injuries have been reduced by 50 percent in 10 years, which is incredible,” Hilton said. “We know that if you don’t take care of your caregivers, the patients’ care is being affected. So, it is ultimately for the patients’ benefit … and improving our patient outcomes.”










